Research Article
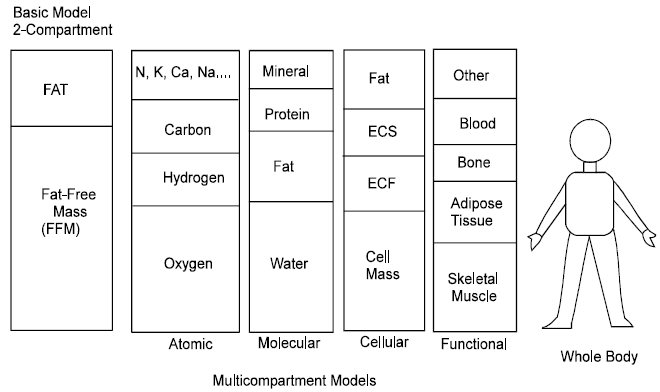
Body Composition, its Significance and Models for Assessment
Life Sciences Group, Isotope Application Division, PINSTECH, P.O. Nilore, Islamabad, Pakistan
Rakhshanda Bilal
Life Sciences Group, Isotope Application Division, PINSTECH, P.O. Nilore, Islamabad, Pakistan