Research Article
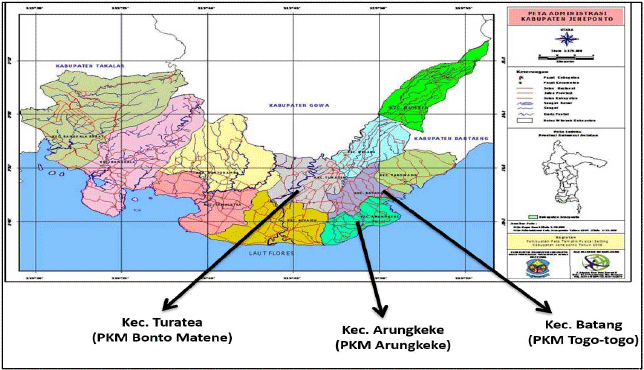
Interprofessional Collaboration Practices: Case Study of the Handling of Malnutrition in Three Public Health Centers in South Sulawesi
Faculty of Public Health, Hasanuddin University, Makassar, Indonesia
Veni Hadju
Department of Nutrition, Faculty of Public Health, Hasanuddin University, Makassar, Indonesia
Ida Leida Maria
Department of Epidemiology, Faculty of Public Health, Hasanuddin University, Makassar, Indonesia
Werna Nontji
Department of Education Hospital, Hasanuddin University, Makassar, Indonesia