Research Article
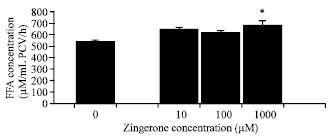
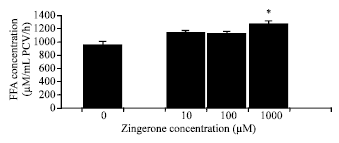
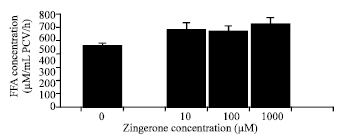
Lipolytic Effects of Zingerone in Adipocytes Isolated from Normal Diet-Fed Rats and High Fat Diet-Fed Rats
Pharmaceutical Chemistry and Natural Product Research Unit, Faculty of Pharmacy Mahasarakham University, Mahasarakham, 44150, Thailand
Klangnapa Thunchomnang
Pharmaceutical Chemistry and Natural Product Research Unit, Faculty of Pharmacy Mahasarakham University, Mahasarakham, 44150, Thailand
Karakate Lawa
Pharmaceutical Chemistry and Natural Product Research Unit, Faculty of Pharmacy Mahasarakham University, Mahasarakham, 44150, Thailand
Apiwat Mangkhalathon
Pharmaceutical Chemistry and Natural Product Research Unit, Faculty of Pharmacy Mahasarakham University, Mahasarakham, 44150, Thailand
Pattarapong Saenubol
Pharmaceutical Chemistry and Natural Product Research Unit, Faculty of Pharmacy Mahasarakham University, Mahasarakham, 44150, Thailand