Research Article
Consumption of Traditional Saudi Foods and Their Estimated Glycaemic Index and Glycaemic Load
Department of Nutritional and Food Sciences, Faculty of Agricultural and Food Sciences, King Faisal University, AL-Hassa, Saudi Arabia
Traditional foods are defined as whole, unprocessed, healthy and nutritious foods that are enjoyed for generation upon generation. All traditional foods are beneficial because of their contribution to physical health and nutritional well-being1. The beneficial properties of traditional food are attributed to the fact that they are prepared from unprocessed and unrefined foods such as whole grains, legumes, fresh fruits and vegetables2,3. It is evident that most unprocessed and unrefined foods are rich in non-starch polysaccharides (NSP), vitamins, minerals and some phytochemicals4,5. Studies have shown that high NSP foods are associated with a favourable effect on satiety and may protect against the development of obesity6-11. In addition, the carbohydrates (CHOs) of unprocessed and unrefined foods are digested at a slower rate, producing a more gradual rise in blood glucose and insulin responses12,13. These features of dietary CHOs have been identified using the concept known as the glycaemic index (GI), which allows foods to be ranked based on the rate of digestion and absorption of their CHOs14,15. High GI foods (>70), in general, produce a high glycaemic response, thus altering fuel partitioning in a way that may be conducive to body-fat gain16. However, consumption of low GI foods (<55) has been found to be associated with significant reductions in energy intake and body weight17,18.
The GI per se takes only the type of CHO into account, ignoring the total amount of CHO in a typical portion. It is important to note that both the quality and quantity of CHO influences the postprandial glycaemic and insulinemic responses to a food19,20. To assess simultaneously the type and amount of CHO consumed, the concept of glycaemic load (GL) was introduced21,22. The GL is a qualitative and quantitative indicator used to estimate the overall impact of CHOs on the blood glucose response23.
The GI and GL values of more than 2500 different types of foods have already been published24. The GI value of most of these foods has been measured in a single food but people usually consume food in combinations as a meal. The applicability of the GI approach to mixed meals by using the GI values of individual foods has been studied. There was a strong correlation (r = 0.88-0.98, p<0.05) for the observed GI versus the predicted GI of mixed meals25-28.
In Saudi Arabia, the daily intake of finely milled cereal and grain products has increased over recent years29, there has been a concomitant reduction in the consumption of some healthy traditional starchy foods. However, there is still some commonplace traditional practice that remains. Traditional Saudi foods are based on whole grain wheat and rice and a handful of them have been tested for the GI, which ranged between 14 and 8930-32. These foods are not usually consumed individually but they are served along with cooked vegetables, meat and sometime legumes. These complementary components can make a change in the glycaemic response and, subsequently, the GI value of the mixed meal. The GI and GL are two methods that have been investigated as potential tools for meal planning or assessing disease risk associated with dietary carbohydrate intake and there is a lack of knowledge about the GI and GL of the traditional Saudi meals.
The effects of traditional Saudi foods consumption on body mass index may help lead to more effective lifestyle prevention strategies for the prevalence of overweight and obesity. In this respect, our hypothesis is that traditional Saudi foods will have a low estimated GI and GL, making them a good choice for losing and maintaining weight. The objectives of the study were to evaluate the consumption of traditional Saudi foods and to estimate their GI and GL.
Subjects: A total of 480 Saudi females participated in the study, with a response rate of 98% (480 of 491). Height, weight and blood pressure were initially taken at baseline. Body mass index (BMI) was estimated from weight in kilograms divided by the square of the height in metres33 and the mean blood pressure (MBP) was calculated34. The frequency of consumption of traditional Saudi foods (TSFs) was reported. Four-point scales were applied to assess the students’ consumption of TSFs and they selected from options 1 = never to 4 = always. Students’ beliefs regarding the quality of TSFs were measured by selecting options from 1 = not healthy or nutritious to 3 = very healthy and nutritious. This study was conducted at the Department of Nutritional and Food Sciences, King Faisal University, AlHassa between Sep 2017 and Dec 2017. This study has been approved by the Research Ethics Committee at King Faisal University, Saudi Arabia (KFU-REC/2017-01-04).
GI and GL of traditional Saudi foods: The GI values were based on glucose as the standard reference and taken from previous studies3,24,30,31. The GI and GL were calculated for the meals prepared from the individual foods by using recommended formula27,35.
Analytical technique of data analysis: The study used SPSS (SPSS for Windows, Version 21.0) for data analysis. All data were examined using two-tailed tests with a significance level of p<0.05 and were checked for normality using the Kolmogorov-Smirnov test (K-S test). Multivariate analysis of variance (MANOVA) was used to examine the effect of the consumption of TSFs on BMI and MBP. The bivariate Pearson correlation was applied to test the relationship between variables. Results were expressed as number (n), percentage and Mean±SD.
Subjects’ characteristics are shown in Table 1. The average age of participants was 20±1.24 years. The prevalence of obesity and overweight among students was 19 and 9%, respectively, according to the average BMI score. Abnormal blood pressure readings were noted in 3.5% of participants (Table 2). The association between BMI and MBP was observed (r = 0.23, p<0.001). The study had predicted that an increase in BMI by 1 unit would result in an increase in MBP by 0.44 mmHg (F = 27.92, p<0.001).
In terms of the consumption of traditional Saudi foods (TSFs), the results revealed that the average consumption of TSFs by students was low. However, Kabsa and Dates were always consumed at a high rate, while Qorssan and Mattaziz were consumed at a very low rate. The association between the average consumption of TSFs and the prevalence of obesity between students was not observed in this study r = -0.068, p = 0.13). However, there was a significant negative correlation between BMI and the consumption of some individual foods, namely, Basmati rice Kabsa, Hassawi rice Kabsa, Falafel (r = -0.12, p<0.01) and Chickpea (r = -0.13, p<0.01).
When multivariate tests were used, Pillai’s trace (F = 0.962, p = 0.47), Wilks’ lambda (F = 0.960, p = 0.47), Hotelling’s trace (F = 0.957, p = 0.47) and Roy’s largest root (F = 1.667, p = 0.173) showed that BMI and MBP were not affected by the average consumption of TSFs. However, BMI was negatively affected by the consumption of Kabsa as it was consumed at high rate.
The majority of students (67%) strongly believed that TSFs are very healthy and nutritious (Table 3). Moreover, the consumption of TSFs was significantly correlated with healthy and nutritious beliefs (r = 0.65, p<0.001).
The study also estimated the GI and GL of TSFs and found that TSFs had, on average, a low GI and a medium GL with values of 55 and 12, respectively.
| Table 1: | Descriptive characteristics of study participants |
 | |
| Results presented as Mean±SD (n = 480). BMI (calculated as weight (kg)/height2 (m)) | |
| Table 2: | Classification of body mass index and blood pressure for participants (n = 480) |
 | |
| Results expressed as percentage | |
The Falafel sandwich had the lowest estimated GI value, followed by Chickpea then Marqooq and Dates with Laban, with values of 33, 36 and 49, respectively. However, there was only one type of food, Saleeq, that had a high estimated GI value. In terms of GL value, the Falafel sandwich again achieved the lowest GL (3). In contrast, Foul had the highest GL with a value of 27 (Table 3).
This study aimed to examine the association between frequent consumption of traditional Saudi foods and BMI in Saudi females. It is well documented that being overweight puts individuals at an increased risk for a range of health problems such as heart disease, diabetes and hypertension as well as for emotional and psychological issues. The TSFs are rarely consumed by recent generations due to the diversity and availability of food from several sources, which has led to major shifts in dietary patterns. However, the majority of students believed that TSFs are healthy and have a high nutritive value. In fact, there were two of these foods (Kabsa and dates) that were frequently consumed at a high rate (91 and 85%, respectively).
Despite that, there was a weak correlation r = 0.2) between the average consumption of TSFs and the beliefs in their health and nutritious benefits, this correlation was highly significant (p<0.001). This finding may encourage people to increase their consumption of TSFs.
| Table 3: | Estimated glycaemic index (GI) and glycaemic load (GL) values of some traditional Saudi meals |
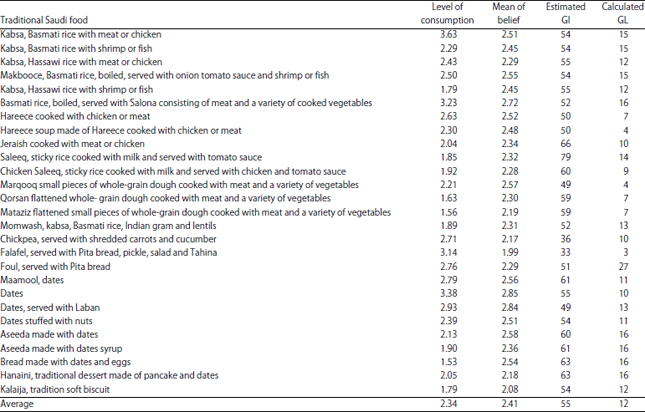 | |
| Author calculation, 2017 | |
This study also aimed to estimate the GI and GL of the most traditional Saudi food prepared from single foods. The estimated GI and GL of TSFs ranged between low to medium. It is evident that the GI concept applies well to mixed meals and the GI of different mixed meals can be predicted from the GI of single foods27,36. The lower estimated GI of traditional foods can be explained by the fact that their CHO may be slowly hydrolysed and, thus, absorbed at a slower rate in the small intestine. These features could help in reducing energy intake, promoting weight loss and consequently preventing weight gain18,37-39.
It is well known that the main source of CHOs in the Saudi diet comes mainly from rice30 and wheat flour29. This study found that the most commonly consumed Saudi food was Kabsa, which is the main dish that is served at lunch time and consists of rice, vegetables and meat30. However, the whole-grain wheat and flour-based dishes such as Mataziz and Qorssan were consumed less (36 and 38%, respectively). It is evident that the starch present in these foods within whole-grain structures can completely inhibit its swelling and dispersion, partially blocking the access of digestive enzymes3. This important feature of starchy Saudi foods could provide a major contribution to the improvement of Saudi diets in terms of lowering blood glucose and insulin responses and consequently promoting postprandial fat oxidation38. Additionally, the consumption of whole-grain foods definitely increases the intake of NSP. Dietary NSP, either soluble or insoluble, plays an important role in increasing satiety and delaying hunger for a long time and reducing energy intake during the remainder of the day40.
Additionally, the consumption of TSFs was inversely correlated with BMI and MBP. This could be explained by the fact that most traditional Saudi foods are unrefined foods and are served with vegetables and meat. It is obvious that frequent consumption of high NSP foods places a particular emphasis on the important and independent role of these foods in helping to prevent obesity as they satisfy appetite for longer and help to burn more body fat6-9.
In conclusion, the major practical implication from this study is to encourage the consumption of healthy Saudi traditional foods. This supports current public health recommendations encouraging the consumption of whole grains, fruits and vegetables as part of a balanced diet.
The study discovered a possible beneficial relationship between the consumption of traditional Saudi foods and body mass index, which could help in reducing the prevalence of obesity and overweight. This will help researchers examine the critical issues related to controlling weight gain that some researchers have tried to explore. Thus, a new theory concerning these traditional Saudi foods may be developed. Dietary advice should be given to encourage the consumption of traditional foods on a daily basis.
The limitation of the study is the limited number of estimated GI and GL values available for traditional Saudi foods due to the lack of information of the measured GI values of some TSFs. Further studies are needed to confirm the impact of long-term consumption of traditional Saudi foods on satiety and on the blood profiles of people with chronic diseases.
The author would like to thank the Deanship of Scientific Research, King Faisal University, Saudi Arabia, for supporting this study (Project No. 160165). Additionally, the author thanks all participants for their time and efforts in participating in this study.