Research Article
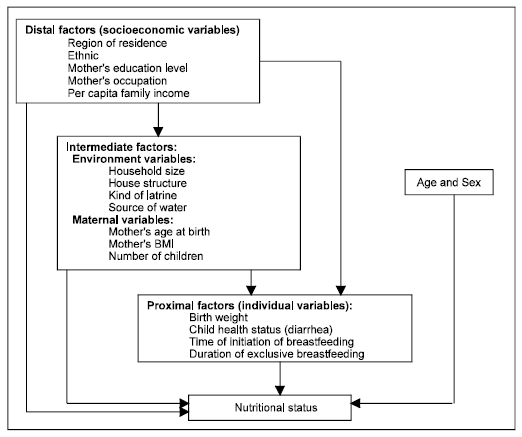
Nutritional Status and Determinants of Malnutrition in Children under Three Years of Age in Nghean, Vietnam
Vinh University, 182-LeDuan, Vinh, Nghean, Vietnam
Nguyen Ngoc Hoa
Nghean General Hospital, 138-Nguyen Phong Sac, Vinh, Nghean, Vietnam