Short Communication
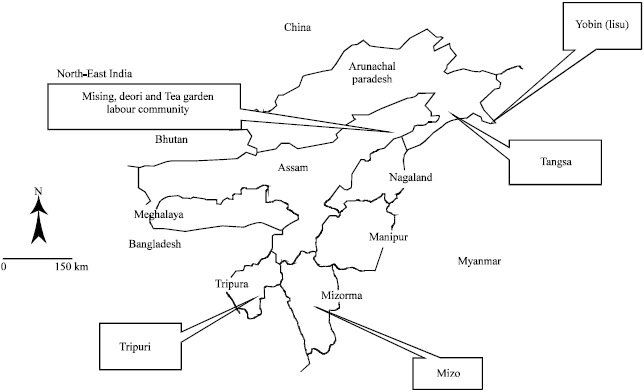
Prevalence of Haemoglobin Variants in Malaria Endemic Northeast India
Regional Medical Research Centre, North East Region, Indian Council of Medical Research, P.O. Box 105, Dibrugarh-786 001, Assam, India
J. Mahanta
Regional Medical Research Centre, North East Region, Indian Council of Medical Research, P.O. Box 105, Dibrugarh-786 001, Assam, India