Research Article
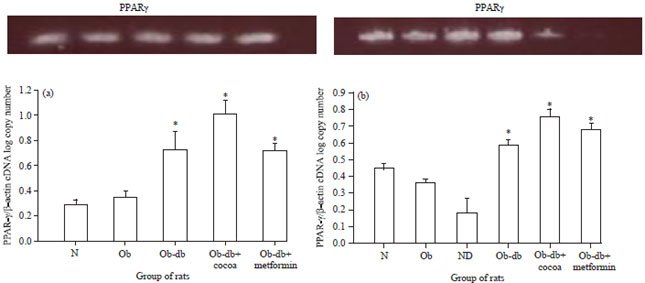
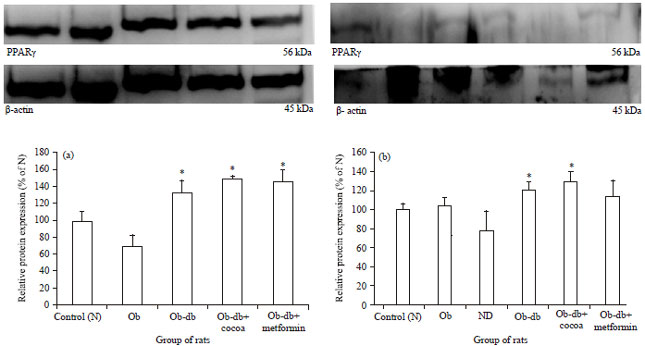
Cocoa Polyphenol-Rich Extract Enhances the Expression Levels of PPAR-γ in the Skeletal Muscle and Adipose Tissue of Obese-Diabetic Rats Fed a High-Fat Diet
Department of Nutrition and Dietetics, Faculty of Medicine and Health Sciences, Universiti Putra Malaysia, 43400 UPM Serdang, Selangor, Malaysia
Faisal Ali
Department of Nutrition and Dietetics, Faculty of Medicine and Health Sciences, Universiti Putra Malaysia, 43400 UPM Serdang, Selangor, Malaysia
Amin Ismail
Department of Nutrition and Dietetics, Faculty of Medicine and Health Sciences, Universiti Putra Malaysia, 43400 UPM Serdang, Selangor, Malaysia
Chong Pei Pei
Department of Biomedical Sciences, Faculty of Medicine and Health Sciences, Universiti Putra Malaysia, 43400 UPM Serdang, Selangor, Malaysia
Muhajir Hamid
Department of Microbiology, Faculty of Biotechnology and Bimolecular Sciences, Universiti Putra Malaysia, 43400 UPM Serdang, Selangor, Malaysia