Research Article
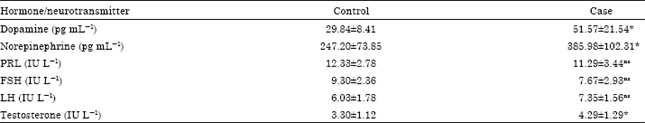
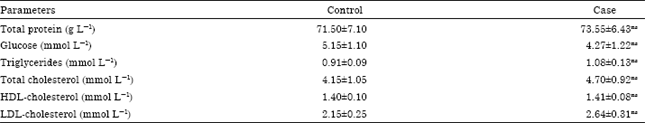
Neuroendocrinological, Metabolic and Toxicological Effects of Chronic Cannabis Use among Male in Lagos
Department of Biochemistry, College of Medicine, University of Lagos, P.M.B. 12003, Lagos, Nigeria
H.S.A. Olasore
Department of Biochemistry, College of Medicine, University of Lagos, P.M.B. 12003, Lagos, Nigeria
E.O. Nanaghan
Department of Biochemistry, College of Medicine, University of Lagos, P.M.B. 12003, Lagos, Nigeria
I.O. Turner
Department of Biochemistry, College of Medicine, University of Lagos, P.M.B. 12003, Lagos, Nigeria
A.A. Owoyale
Department of Biochemistry, College of Medicine, University of Lagos, P.M.B. 12003, Lagos, Nigeria
O.A. Magbagbeola
Department of Biochemistry, College of Medicine, University of Lagos, P.M.B. 12003, Lagos, Nigeria