Research Article
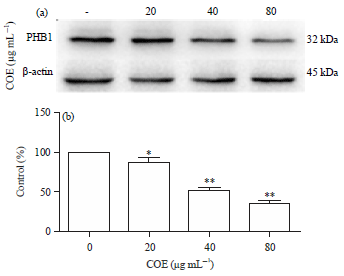
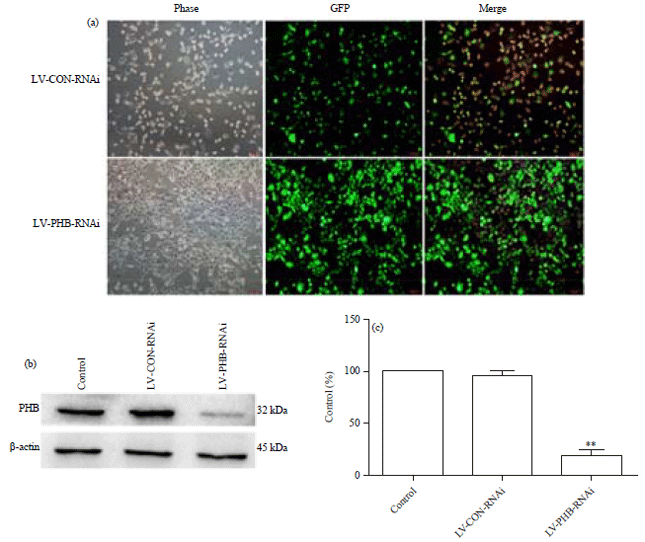
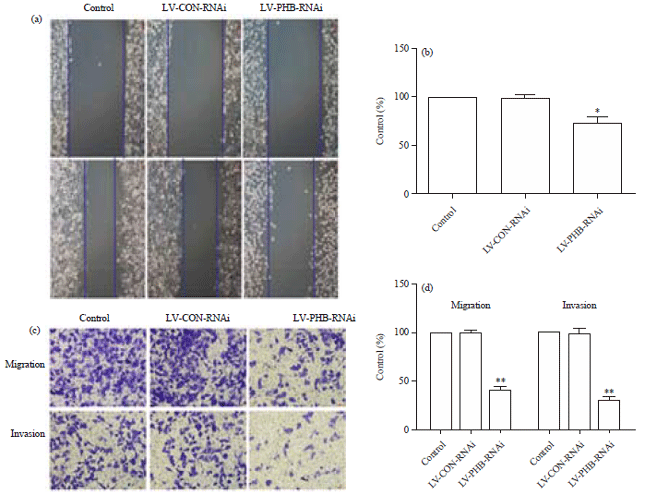
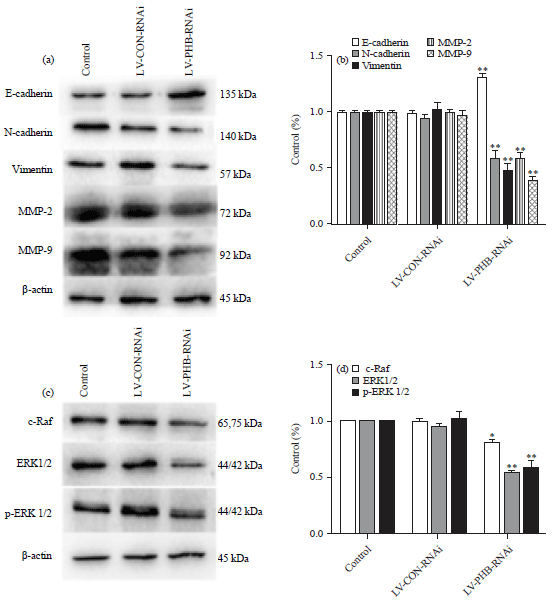
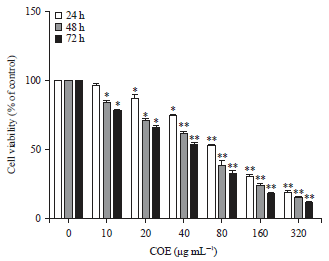
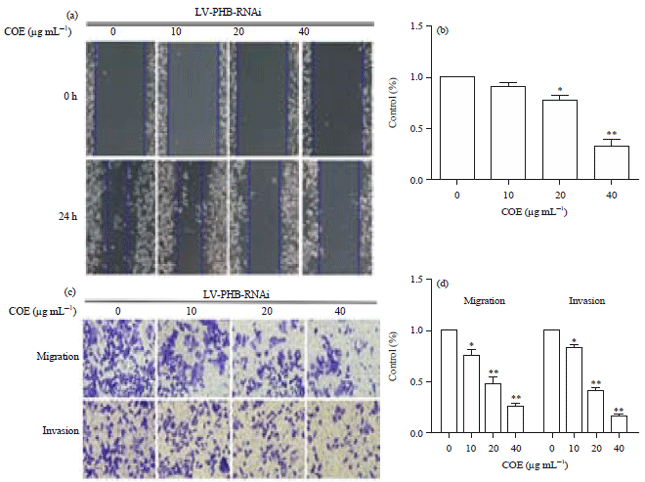
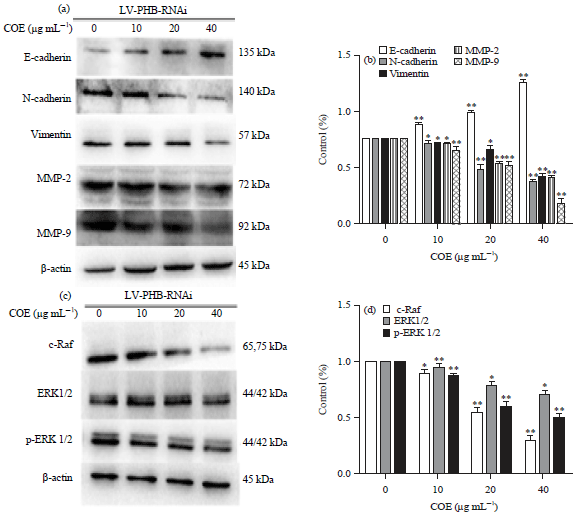
Celastrus Orbiculatus Extract Suppresses Migration and Invasion of Gastric Cancer by Inhibiting Prohibitin and c-Raf/ERK Signaling Pathway
Department of Gastroenterology, Affiliated Hospital of Yangzhou University, Yangzhou University, 225000, Yangzhou, China
Hai-bo Wang
Department of Gastroenterology, Affiliated Hospital of Yangzhou University, Yangzhou University, 225000, Yangzhou, China
Feng Jin
Department of Gastroenterology, Affiliated Hospital of Yangzhou University, Yangzhou University, 225000, Yangzhou, China
Li-de Tao
Yangzhou University-Yangzhou Cancer Research Institute, Yangzhou University, Yangzhou, 225009, Jiangsu, People�s Republic of China
Dan Li
Department of Gastroenterology, Affiliated Hospital of Yangzhou University, Yangzhou University, 225000, Yangzhou, China
Teng-yang Ni
Department of Gastroenterology, Affiliated Hospital of Yangzhou University, Yangzhou University, 225000, Yangzhou, China
Wen-yuan Li
Department of Gastroenterology, Affiliated Hospital of Yangzhou University, Yangzhou University, 225000, Yangzhou, China
Bo Pan
Yangzhou University-Yangzhou Cancer Research Institute, Yangzhou University, Yangzhou, 225009, Jiangsu, People�s Republic of China
Wei-ming Xiao
Department of Gastroenterology, Affiliated Hospital of Yangzhou University, Yangzhou University, 225000, Yangzhou, China
Yan-bing Ding
Department of Gastroenterology, Affiliated Hospital of Yangzhou University, Yangzhou University, 225000, Yangzhou, China
Masataka Sunagawa
Department of Physiology, School of Medicine, Showa University, 142 Tokyo, Japan
Yan-qing Liu
Department of Gastroenterology, Affiliated Hospital of Yangzhou University, Yangzhou University, 225000, Yangzhou, China
LiveDNA: 86.23350