Research Article
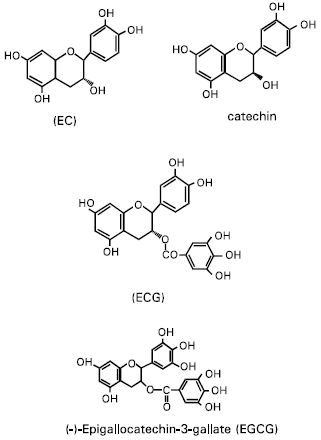
Effect of Tea Polyphenols on Masugi Nephritis of Rabbit
College of Life Science, Zhejiang University, Hangzhou-310029, China
Chen Ji-shuang
College of Life Science, Zhejiang University, Hangzhou-310029, China
Yang Xian-qiang
Department of Tea Science, Zhejiang University, Hangzhou-310029, China