ABSTRACT
Intracranial hypertension is initially an alarm signal for the increased ICP; later the increase in intracranial pressure is accompanied by symptoms and there is the ICH syndrome; later on the increase in ICP becomes a pathogenic mechanism in itself and intracranial hypertension appears as an acute disease. The pattern of ICH includes a three-phase evolution; the pressure-time fluctuation is the dynamic element in the progression and decompensation of intracranial hypertension. The evolution of ICH is made by exceeding the critical thresholds of the ICP equivalent to each stage and the decompensation corresponds to the acute critical pressure-time fluctuation. The main features that determine clinical course of intracranial hypertension are: the speed of ICP increase till and over the normal limit, the critical thresholds and the highest value of ICP, the period of pathologic value of ICP, the length of recurrence to normal value and the frequent occurrence of ICP increase. There are five main forms of ICP increase depending of the rapidity of ICP increase till normal limit and over. Intracranial hypertension is classified in four forms based on the etiopathogenesis: parenchymatous intracranial hypertension with an intrinsic cerebral cause, vascular intracranial hypertension, which has its etiology in disorders of the cerebral blood circulation, meningeal intracranial hypertension and idiopathic intracranial hypertension, the former pseudotumor cerebri; it is an incomplete ICH syndrome.
PDF Abstract XML References Citation
How to cite this article
DOI: 10.3923/jms.2004.52.58
URL: https://scialert.net/abstract/?doi=jms.2004.52.58
INTRODUCTION
The intracranial hypertension (ICH)-one of the most important syndromes in neurology and neurosurgery-is the increase of the intracranial pressure (ICP) which occurs as a result of the disturbance of the regulatory intracranial pressure mechanisms, caused by the changes in the volumes of the intracranial components: brain parenchyma, cerebrospinal fluid and cerebral blood volume and by exceeding the capacities of compensating the elevated ICP[1,2] Intracranial hypertension develops from the initial cerebral effect of increased intra-cranial pressure and becomes symptomatical; then it acquires its individuality, surpas-sing the initial disease. The intracranial hypertension syndrome corresponds to the stage at which the increases in intracranial pressure (ICP) can be compensated and the ICH disease is in its acute form, equivalent to a decompensated ICH syndrome.
The type of ICP increase seems to be characteristic for each disease of the brain and ICP monitoring shows some features[3-6]:
| ● | the speed of ICP increase till the normal value of 20 mm Hg and over this normal limit, therefore there are two segments of ICP increase: one of the increase till the normal limit of ICP and the second of ICP increase until the high pathologic values, |
| ● | the peak value of ICP increased, |
| ● | the period of pathologic values of ICP, |
| ● | the length of recurrence to normal value of ICP, |
| ● | the frequent occurrence of ICP increase. |
The speed of ICP increase until normal limit of 20 mm Hg can be rapid or slow and also the speed of the ICP increase over this normal limit can be rapid or slow[7].
There are some types of ICP increase conformity with the features above:
| ● | A very rapid increase of ICP till to 20 mm Hg and then over this value the ICP increase can be very rapid, until a high value of ICP. This type of ICP increase appears in acute situations as haematoma or traumatic brain edema, when a new volume develops quickly into the cranium. The infraclinic period and the period of ICH syndrome are short. The decompensation if ICH is rapid because of the high speed of new volume development and of the exceeding of the compensatory capacities.There is a big rapidity of ICP increase but the pathologic values of ICP are near the normal limit of ICP; the period of high values of ICP is short, because of the rapid decompensation (Fig. 1). |
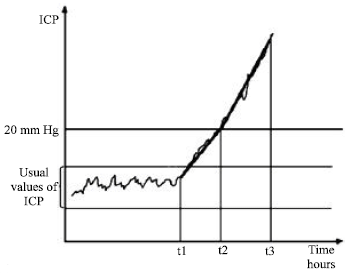 | |
| Fig. 1: | Types of acute ICP increase |
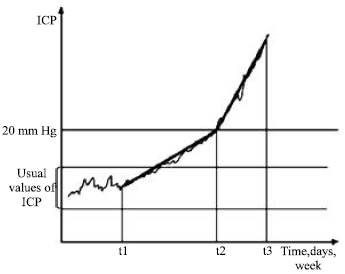 | |
| Fig. 2: | Types of ICP increase in brain tumor |
| ● | A slow increase of ICP till to 20 mm Hg and then over this value, the ICP increase is rapid too; this type of ICP increase appears in brain tumors, cerebral abceses etc. when a new volume develops slow into the cranium.The infraclinic period and the period of ICH syndrome are longer as in acute cases but the decompensation if ICH over the ICP of 20 mm Hg is also rapid because of the exceeding of the compensatory capacities. Also the pathologic values of ICP are near the normal limit of ICP and the period of high values of ICP is short, because of the rapid decompensation (Fig. 2). |
| ● | The rapidity of ICP increase till the normal limit of 20 mm Hg is medium as a rule, the high values of pathologic ICP are similar as in the above two types, but the period of high ICP values is longer as the previous forms of raised ICP. This ICP increase appears in ICH syndrome determined by hypertensive encephalopathies; as a rule there is a completye and prolonged ICH syndrome (Fig. 3). |
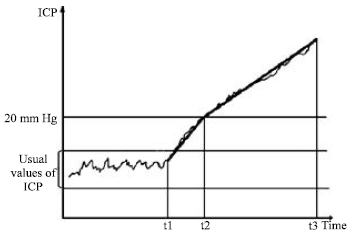 | |
| Fig. 3: | Types of ICP increase in hypertensive encephlopathy |
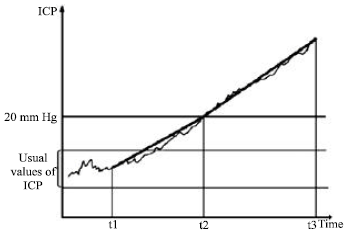 | |
| Fig. 4: | Types of ICP increase in diminishing of CSF absorbtion |
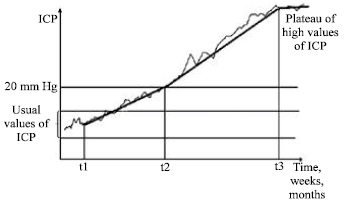 | |
| Fig. 5: | Types of ICP increase in idiopathic intracranial hypertension |
| ● | The increase of ICP is slow till normal limit and over 20 mm Hg the ICP increase is also slow. This pattern of ICP increase appears in the cases of diminition of cerebrospinal fluid absorbtion in acute meningitis, subarachnoid haemorrhage, carcinomatous meningitis, chronic meningitis-sarcoidosis; also in cases of the cerebral venous thrombosis and superior sagital sinus thrombosis, cerebral thromboflebitis, mastoiditis, usually in cerebral vascular disorders. The speed of ICP increase is less than the anterior type and there are resources of partial compensation and to maitain the cerebral blood flow. The period of pathologic values of ICP is extended and usually there is not a clinical decompensation; as a rule there is a completye and prolonged ICH syndrome (Fig. 4). |
| ● | The fifth form of raised ICP has a very slow speed of ICP increase. This gradual increase of ICP permits a good compensation and a quasi-normal cerebral blood flow; therefore the pathologic values of ICP can be very high, till 60-80 mm Hg, only with papillar edema and headache. There is a plateau of this high values of ICP. There is only an incomplete ICH syndrome but very prolonged and without decompensation (Fig. 5). |
Forms of intracranial hypertension: The intracranial hypertension can be systematized in four forms according to its etiology, to the pathogenic mechanisms and to the patterns of ICP increase.
Parenchymatous intracranial hypertension: This form appers in expansive intracranial processes (tumours, haematomas, cerebral abscesses etc.); in traumatic brain edema; general intoxication with neural toxins (exogenous or endogenous) etc.[8-11]. A primary known brain etiology causes the modification in the intracranial volume and then the brain edema appears, evolving towards an increase in intracranial pressure. The direct parenchymatous lesion occurs first as a result of intrinsic brain etiology and of the primary modifications of intracranial volume (expansive, compressive, hypoxic or traumatic brain edema). Frequently the brain edema is sectorial and often there are difference between the cerebrospinal compartments. There is a very rapid or a slow increase of ICP over 20 mm Hg, but the length of time of pathologic ICP is short because of the decompensation. The parenchymatous ICH can have a complete evolution up to the acute form with brain stem ischemia or brain herniation[6,7,9,12].
Vascular intracranial hypertension: The development of brain edema and the increase of ICP are determined by disorders of the cerebral blood volume (excluding the etiology of parenchymatous ICH). The brain edema occurs by “brain congestion” following the increase of the cerebral blood volume, caused by an important coming of blood volume or by a reduction or a stopping of the cerebral blood outflow.
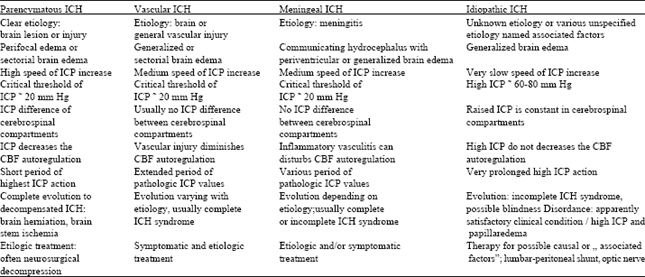
| Table 1: | Pathogenetical classification of intracranial hypertension |
 | |
There are also a reduction of the cerebro-spinal fluid (CSF) absorbtion in the lessening of the cerebral blood flow[13]. Vascular ICH occurs in vascular cerebral diseases: cerebral venous thrombosis and superior sagittal sinus thrombosis, mastoiditis with transverse or sigmoid sinus thrombosis (the “otic hydrocephalus” described by Simonds) and in extracerebral diseases: hypertensive encephalopathies as acute hypertensive encephalopathy in cases of malignant hypertension from any cause, in glomerulonephritis, eclampsia and in chronic hypertensive encephalopathy as Binswanger’s encephalopathy or in cerebral venous outflow reduction in congestive cardiac failure or intrathoracic mass lesions. The acute stoke is a cerebrovascular disease with different mechanisms but with two resultants on the brain: ischaemia (85%) or haemorrhage (15%). The site of primary lesion in ischaemic stroke can be an intra-or extracranial vascular disease. Brain edema and the increase of ICP occur through ultrafiltration after the increase of cerebral blood flow around infaction and/or there is a vasogenic brain edema. Usually there is a brain edema of the whole brain, but in some cases as in ischaemic stroke with ICH there is a sectorial brain edema. Obstruction of the beginning of venous circulation causes a vascular ICH alike meningeal ICH. Clinical acute presentations are due to elevated ICP in vascular ICH but many symptoms are different depending of the etiology[10,14,15].
Meningeal intracranial hypertension: Meningeal ICH includes the cases of diminition of cerebrospinal fluid absorbtion in acute meningitis, subarachnoid haemorrhage, carcinomatous meningitis, chronic meningitis-sarcoidosis.There are a thickening of the leptomeninges and an involvement of the arachnoid granulations and it occurs a lessening of the CSF absorbtion and an acute “communicating” hydrocephalus with acute ICH syndrome. Clinical features and pattern of ICP increase are alike in ICH syndrome resulting from obstruction of CSF flow (as in obstructive hydrocephalus)[1,16,17].
Idiopathic intracranial hypertension: The etiology could not be establish. It occurs in endocrine, metabolic and hematological diseases, hormonal treatments etc.[2,18,19]. The frequency of the ICH syndrome is the lowest with regard to the diseases to which it is correlated. The increase of ICP is gradual with a very slow speed and this permits a good compen-sation of the raised ICP. The increase of ICP is very important, till 60-80 mm Hg but the brain vascular autoregulation compensates the increase in ICP and maintains the cerebral blood flow. There was three major theories of the cause of idiopathic ICH (IdICH):
| ● | increased resistance to CSF absorption; |
| ● | increased CSF production and |
| ● | increased venous sinus pressure (some authors do not exclude IdICH occuring because of dural sinus thrombosis)[10,20-23] |
Other theory is presented further on[5,13]: The characteristics of IdICH and the anatomical and physiological data show that the mechanisms of elaboration of the interstitial fluid at blood-brain barrier (BBB) and of cerebrospinal fluid (CSF) at choroid plexus are very similarly. In IdICH many pathological conditions can induce the simultaneous hypersecretion of CSF and of the brain interstitial fluid and the high intracranial pressure (ICP) of CSF is equalized simultaneously of the pressure of the brain interstitial fluid.The cerebral blood flow is maintained quasinormal in IdICH, even increased, so that it occurs a fast absorption of CSF and of interstitial fluid and the brain injury is insignificantly despite the high ICP. Therefore idiopathic intracranial hypertension can occur through simultaneous hypersecretion of the cerebrospinal fluid and of the cerbral interstitial fluid followed by a rapid circulation and absorption of these fluids based on a fast cerebral blood flow. The brain edema is of the whole brain and there is not difference of the raised ICP between the cerebrospinal compartments. The period of the pathologic values of ICP is prolonged and the symptoms are reduced: headache, papilledema and visual loss, early or late.Therefore IdICH evolves only at an incomplete ICH sindrome[5,10,13].
The diagnosis of IdICH is a diagnosis of exclusion: increased ICP without parenchymatous etiology orvascular or meningeal causes. Idiopathic ICH is often to obese women, with large incidence in third decade; also there are some associated conditions: drugs (tetracycline, cimetidine etc.), oral contraceptive, Cushing’s disease, hypothyroidism, obese children etc[6].
Vascular ICH and Id ICH are the two parts of the former pseudotumor cerebri; the determination of the etiology of Id ICH will pass some types of IdICH to other ICH forms. Parenchymatous ICH evolves to the acute form through brain stem ischemia or brainherniation because of the difference of ICP between the three cerebrospinal compartments; vascular ICH and meningeal ICH evolve usually including the ICH syndrome and the essential ICH is only an incomplete ICH syndrome. The main features of this four forms of ICH (Table 1).
Dynamic model of the intracranial hypertension: A dynamic model of the ICH is based on the relation between ICP and the period of high-pressure action: the critical pressure-time fluctuation causes the autoregulation of the cerebral blood flow to decrease or determines the brain herniation. The decompensation is a state of instability and appears when the intrinsic ratio of pressure-time fluctuation is changed:the high ICP lasts longer than the corresponding normal ICP, or the ICP is higher than the one that normally lasts the same period of time.
The increase in intracranial pressure (ICP) is the initial cerebral effect of the changes between volume and intracranial pressure. After that the intracranial hypertension causes pathophysiological disorders that determine characteristic modifications of the endocranial structures and therefore the increase in ICP is accompanied by its specific clinical symptoms ICH as a initial sign of the causal disease becomes a syndrome and evolves simultaneously with the causal disease or can progress as an apparently independent disease. The increase of ICP up to 15 mmHg represents an alarm signal for a possible ICH but it does not cause by itself other pathophysiological mechanisms and is not accompanied by symptomatology[4,10,20]. Intracranial hypertension remains a sign as elevated ICP or evolves into a syndrome or just a disease depending on the mechanism that causes it. This evolution of ICH arises from the transformation of the initial increase of the ICP into a pathogenic mechanism and from the progression of the characteristic symptoms whose intensity can exceed the symptomatology of the initial diseases.The moment when the high ICP causes other self-evolving disturbances depends on the specific limits of the capacities to compensate the increase in ICP. ICH syndrome can progress differently depending of the initial etiology; the individual characteristics and fortuitous elements can accelerate or not its evolution; sometimes there is a direct transition from ICP as initial sign to acute ICH. The ICH syndrome corresponds to an increase in ICP of about 20 mm Hg and it is accompanied of symptoms; the new symptomatology is specific and intracranial hypertension becomes a disease with its own development. The ICH disease has high ICP values, of over 20 mm Hg and the decompensation is determined by cerebral ischemia (with brain stem ischemia) or brain herniation[13]. The values of ICP corresponding to the transition to the subsequent biomechanical stage and successive clinical condition are critical-thresholds of the ICP and are equivalent to an instability state.
The clinical stages of ICH are:
| ● | an infraclinic form: the ICP increased around and over the physiological values, |
| ● | an ICH syndrome: ICP of up to 20 mm Hg and cinical symptoms with slow development in a chronic form; it is the period of compensation of increased ICP in the diseases which evolve with ICH; |
| ● | an ICH disease: the acute form with ICP over 20 mm Hg, the symptoms of the preceding stage are increased until decompensation. |
These clinical stages are reversible by an effective treatment and this means a reversible process for the corresponding biomechanichal stages. The length of time of each stage appears inversely proportional to the value of ICP and high ICP accelerates the evolution of ICH to the acute form. Intracranial hypertension syndrome corresponds to the stage at which the increase in ICP is compensated, while the ICH disease is determined by the exceeding of the compensatory capacities for the increases in ICP; therefore the intracranial hypertension disease is the decompensated ICH syndrome.
Intracranial hypertension is initially an alarm signal for the increased ICP; later the increase in intracranial pressure is accompanied by symptoms that represent the ICH syndrome; later on the increase in ICP becomes a pathogenic mechanism in itself and intracranial hypertension appears as an acute disease with its individual evolution.
The main features that determine clinical course of intracranial hypertension are:
| ● | the speed of ICP increase till and over the normal limit, |
| ● | the critical thresholds and the highest value of ICP, |
| ● | the period of pathologic value of ICP, |
| ● | the length of recurrence to normal value and |
| ● | the frequent occurrence of ICP increase. |
There are five main forms of ICP increase depending of the rapidity of ICP increase till normal limit and over.
The dynamic pattern of ICH includes a three-phase evolution andit has a precise course defined by determined mechanisms, but unstable because the evolutionary complexity depends on each individual case. The pressure-time fluctuation is the dynamic element in the progression and decompensation of intracranial hypertension. The evolution of ICH is made by exceeding the critical thresholds of the ICP equivalent to each stage and the decompensation corresponds to the acute critical pressure-time fluctuation.
The compensation mechanisms can block the evolution of pressure-time fluctuation to the critical situation as long as the intrinsic proportionality ratio of ICP-period of action is maintained. Further on there is the possibility of a reversible process until the organic injury occurs. The intracranial hypertension syndrome corresponds to the stage at which the increases in ICP can be compensated, equivalent to the chronic form of ICH; while the ICH disease is the acute form and is a decompensated ICH syndrome.
The classification of ICH is based on the etiopathogenesis:
| ● | parenchymatous intracranial hypertension with an intrinsic cerebral cause; |
| ● | vascular intracranial hypertension has the etiology in disorders of cerebral blood circulation and advances usually until the ICH syndrome. |
| ● | meningeal intracranial hypertension and |
| ● | essential or idiopathic intracranial hypertension is the former pseudotumor cerebri and it is an incomplete ICH syndrome. |
The therapeutic objectives are preventing the ICP from exceeding 20 mm Hg and maintaining a normal cerebral blood flow. The emergency therapy is the same for the acute form and each of the four forms of ICH has a specific therapy, according to the pathogenic mechanism and if possible to the aetiology. The evolution of the parenchymatous ICH shows a disturbance in autoregulation of cerebral blood circulation that precipitates the decompensation of intracranial hypertension.









Simoen Reply
This study delves into the pattern of increased intracranial pressure (ICP) and the classification of intracranial hypertension (ICH). It discusses the evolution of ICH and the critical thresholds of ICP. The study also identifies the main features that determine the clinical course of ICH, such as the speed of ICP increase and the period of pathologic value of ICP. The classification of ICH is based on four forms of etiopathogenesis: parenchymatous, vascular, meningeal, and idiopathic. The study provides valuable insights into the progression and decompensation of ICH, which could aid in the development of effective treatments for this condition.
Editor
Dear Simeon,
We appreciate your thoughtful comments and are glad that you found the study to be informative.
We agree that the study provides valuable insights into the pattern of increased intracranial pressure and the classification of ICH. We hope that this information will be useful in the development of effective treatments for this condition.
Thank you again for your feedback, and we hope that you will find our future publications equally informative and valuable.