Review Article
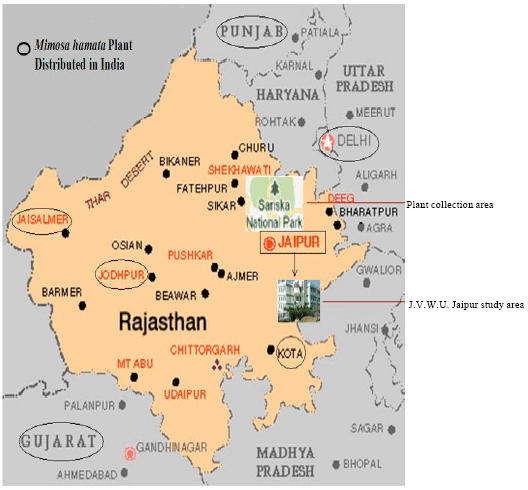
Pharmacological Evaluation of an Ethnomedicinal and Endangered Desert Plant: Mimosa hamata
School of Sciences, Suresh Gyan Vihar University, Jagatpura, Jaipur-302017, (Raj.), India
Richa Saxena
School of Sciences, Suresh Gyan Vihar University, Jagatpura, Jaipur-302017, (Raj.), India
Subhash Chandra
School of Sciences, Suresh Gyan Vihar University, Jagatpura, Jaipur-302017, (Raj.), India
Shilpa Bhargava
School of Sciences, Suresh Gyan Vihar University, Jagatpura, Jaipur-302017, (Raj.), India
S.C. Joshi
Department of Zoology, University of Rajasthan, Jaipur-302004, India