Research Article
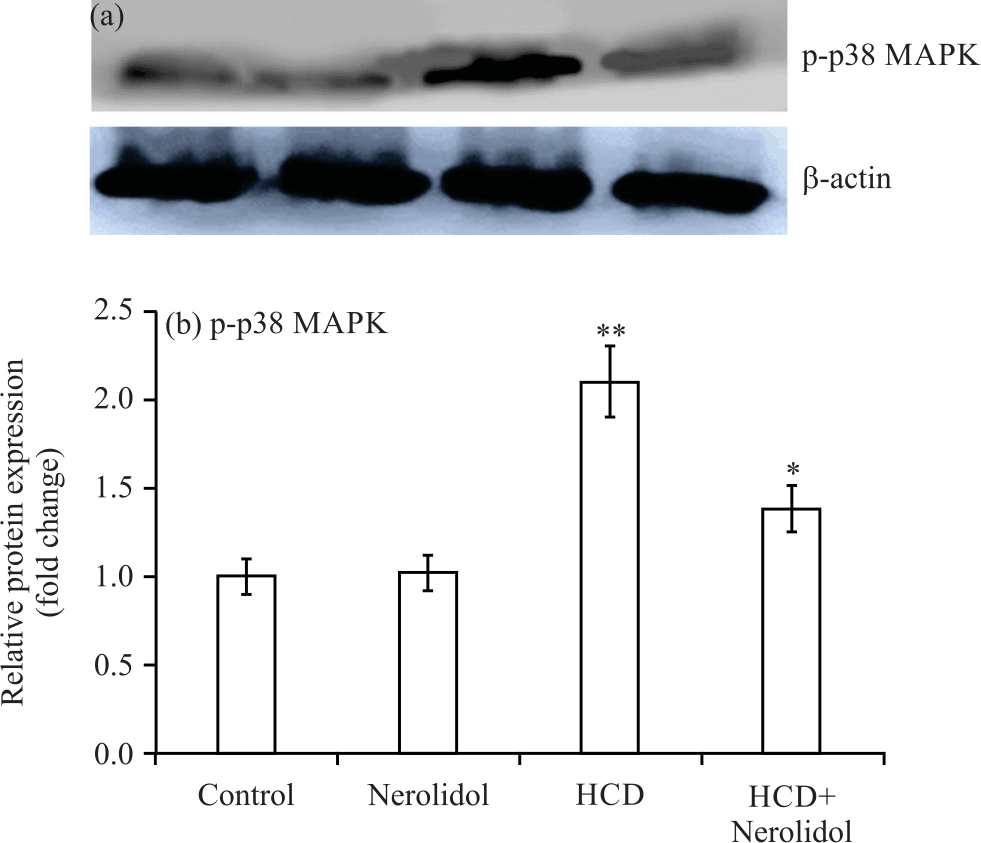
Influence of Nerolidol on High-cholesterol Diet-Induced Atherosclerosis in Rats via Antioxidant and p38 MAPK Signaling Pathway
Physical Examination Center, Electrocardiogram Room, 904 Hospital of PLA Joint Logistics Support Force, Wuxi, Jiangsu 214000, China
Lina Sun
Department of Cardiology, Qingdao Chengyang People’s Hospital, Qingdao, Shandong 266109, China
Baoning Zuo
Department of Cardiology, Second People’s Hospital of Qingyang, Qingyang, Gansu 745000, China
LiveDNA: 86.37355