Research Article
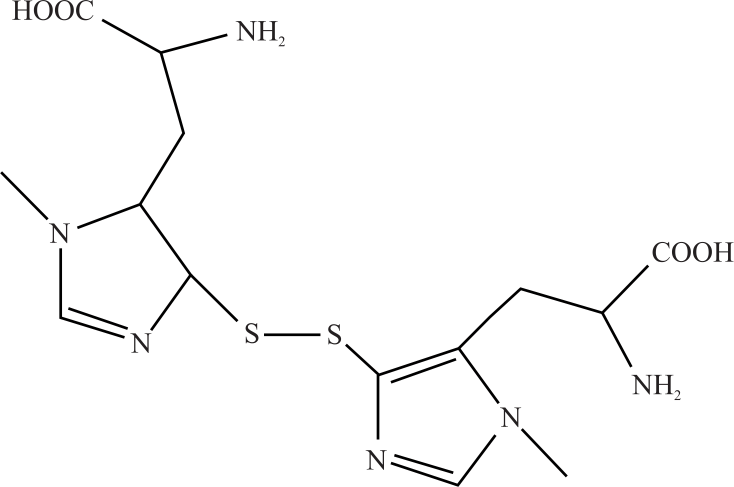
Ovothiol-A Ameliorates Renal Injury Induced by Bile Duct Ligation in Rats (Biological, Quantum-Chemical and Molecular Docking Study)
Department of Biotechnology, Faculty of Sciences, Cairo University, Giza 12613, Egypt
Mohamed Refaat Shehata
Department of Chemistry, Faculty of Sciences, Cairo University, Giza 12613, Egypt
Ayman Saber Mohamed
Department of Zoology, Faculty of Sciences, Cairo University, Giza 12613, Egypt
LiveDNA: 20.36184
May Mohamed Elbatran
Departments of Pharmacology and Toxicology, Faculty of Pharmacy, Cairo University, Giza 12613, Egypt