Research Article
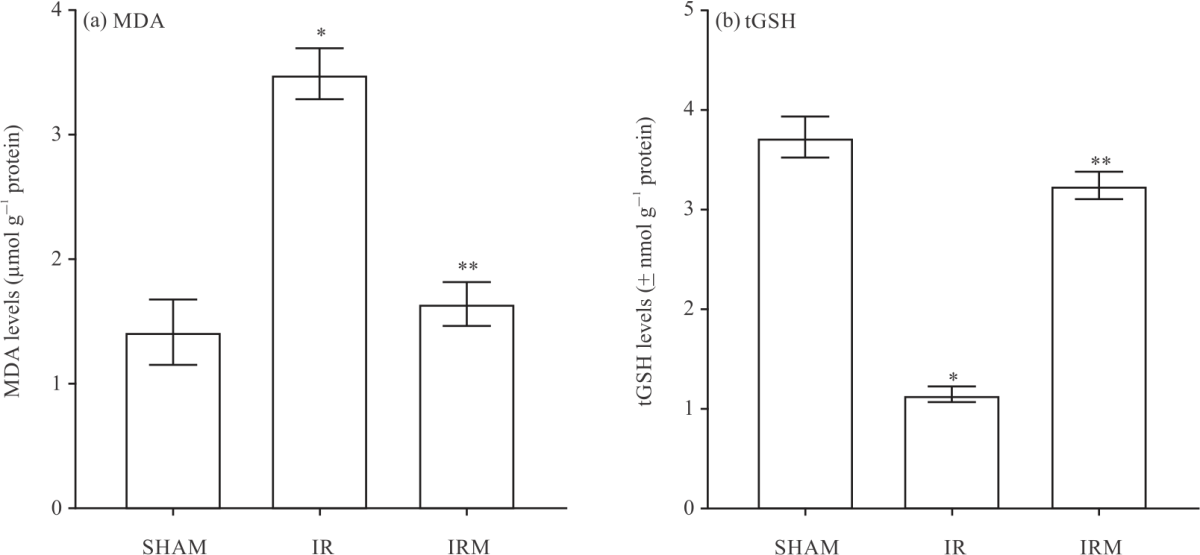
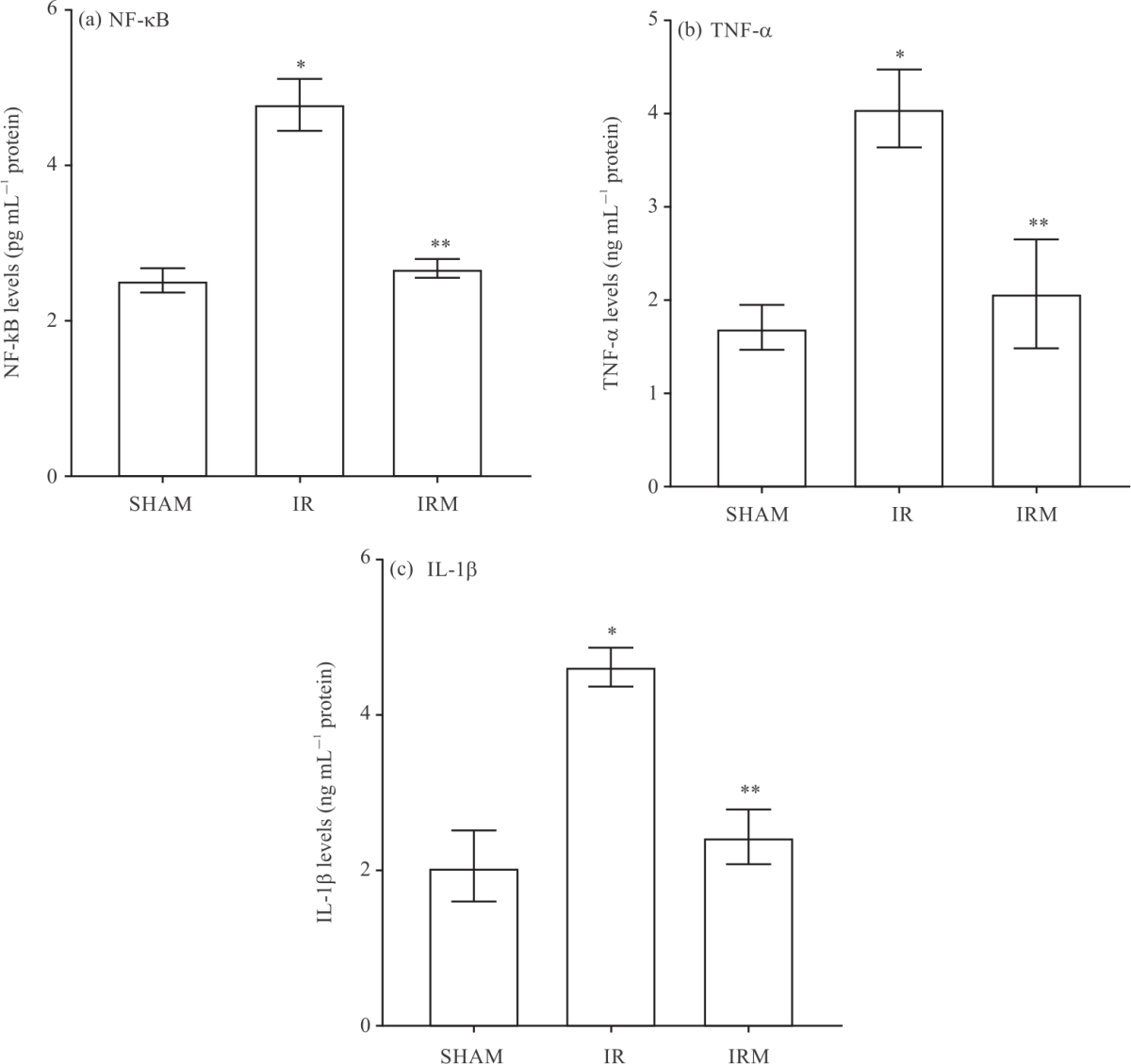
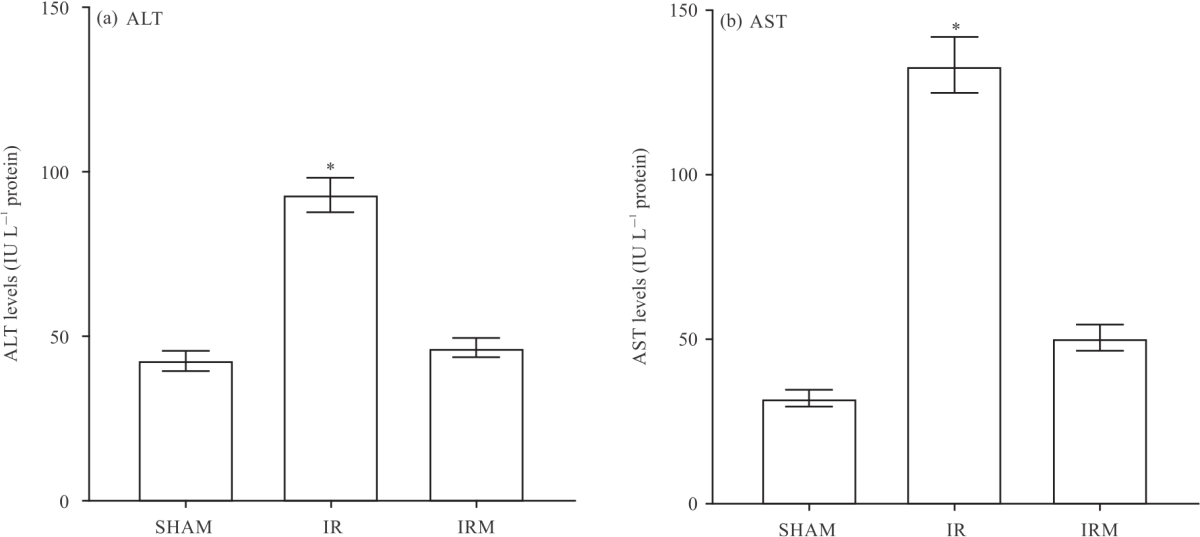
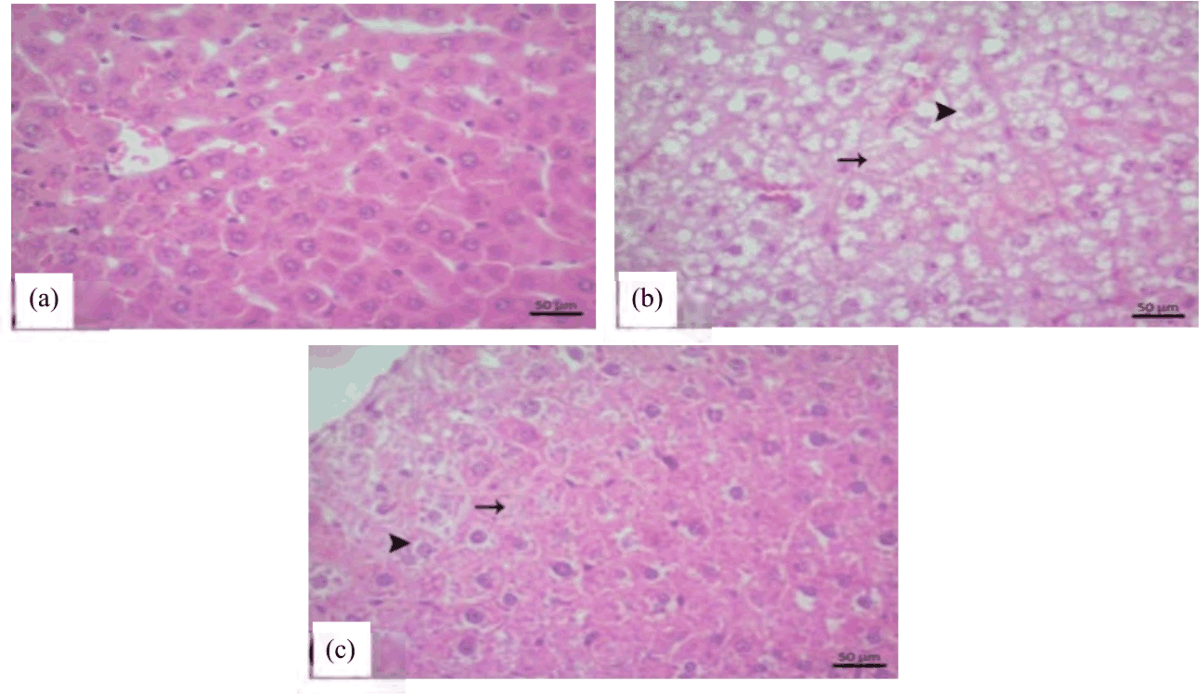
Effects of Mirtazapine on Liver Ischemia-Reperfusion Injury in Rats
Department of General Surgery, University of Health Sciences, Prof. Dr. Cemil Tascioglu City Hospital, Istanbul, Turkey
Ismayil Yilmaz
Department of General Surgery, University of Health Sciences, Prof. Dr. Cemil Tascioglu City Hospital, Istanbul, Turkey
Fatih Ozcicek
Department of Internal Medicine, Erzincan Binali Yildirim University, School of Medicine, Erzincan, Turkey
Seval Bulut
Department of Pharmacology, Erzincan Binali Yildirim University, School of Medicine, Erzincan, Turkey
Arif Onur Eden
Department of Emergency Medicine, Erzincan Binali Yildirim University, School of Medicine, Erzincan, Turkey
Cebrail Gursul
Department of Physiology, Erzincan Binali Yildirim University, School of Medicine, Erzincan, Turkey
Ali Sefa Mendil
Department of Pathology, Faculty of Veterinary, Erciyes University, Kayseri, Turkey
Mehmet Kuzucu
Department of Biology, Faculty of Arts and Sciences, Erzincan Binali Yildirim University, School of Medicine, Erzincan, Turkey
Durdu Altuner
Department of Pharmacology, Erzincan Binali Yildirim University, School of Medicine, Erzincan, Turkey
Halis Suleyman
Department of Pharmacology, Erzincan Binali Yildirim University, School of Medicine, Erzincan, Turkey
LiveDNA: 90.23571