Review Article
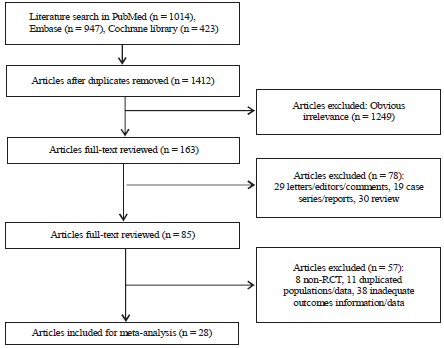
Bayesian Meta-Analysis: The Effect of Statins on the Treatment of Hypercholesterolemia
Department of Cardiology, Jinan Central Hospital Affiliated to Shandong University, 250013 Jinan, Shandong Province, China
Qing Zhu
Shandong Blood Center, 250013 Jinan, Shandong Province, China
Liqi Wang
Department of Cardiology, Jinan Central Hospital Affiliated to Shandong University, 250013 Jinan, Shandong Province, China
LiveDNA: 86.16380