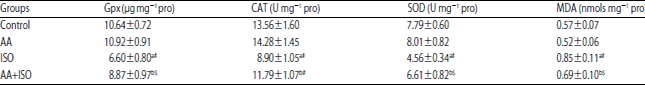Research Article
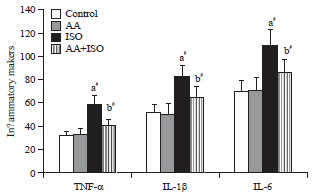
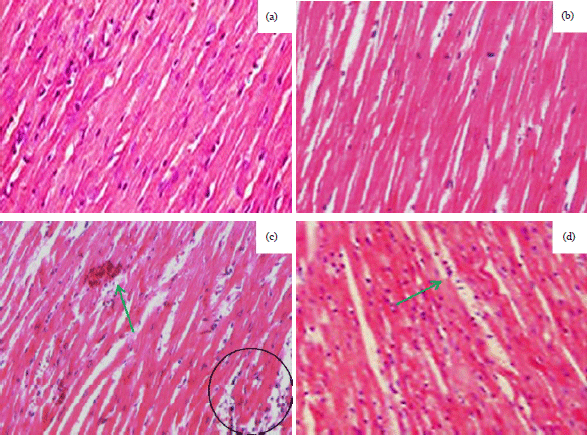
Asiatic Acid Enhances Antioxidant and Anti-inflammatory Activity to Suppress Isoproterenol Induced Cardiotoxicity
Department of Cardiovascular Medicine, The First Hospital of Nantong, Nantong 226000, China
Liang Chen
Department of Cardiovascular Medicine, The First Hospital of Nantong, Nantong 226000, China
Huihe Lu
Department of Cardiovascular Medicine, The First Hospital of Nantong, Nantong 226000, China
LiveDNA: 86.24162