Research Article
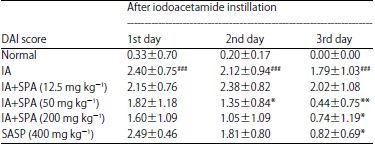
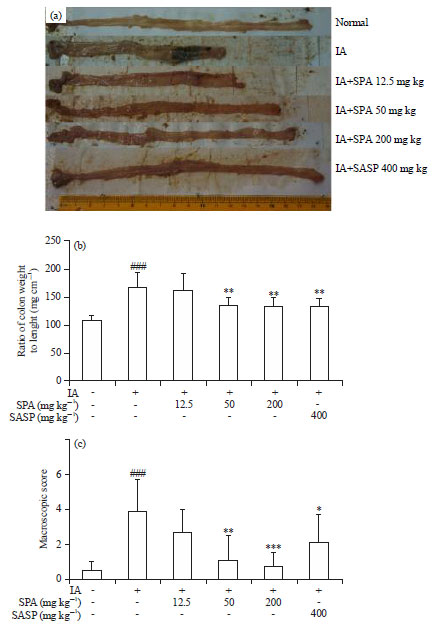
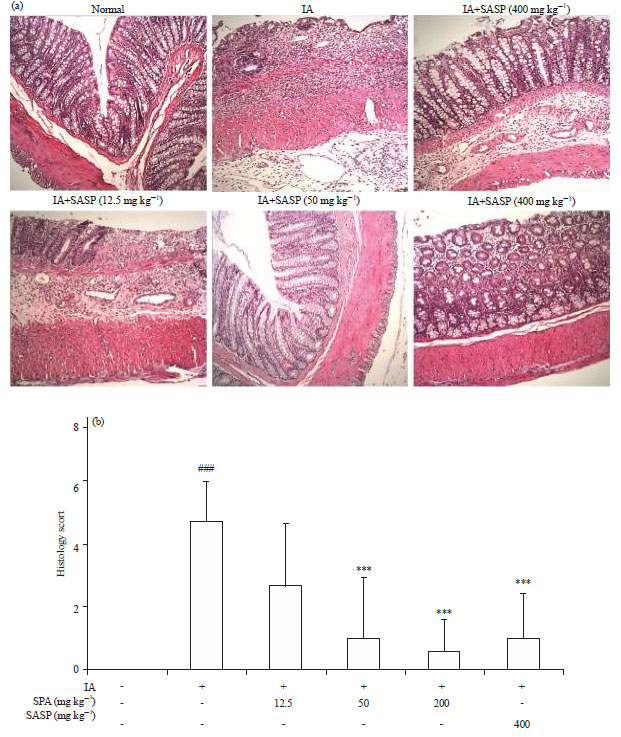
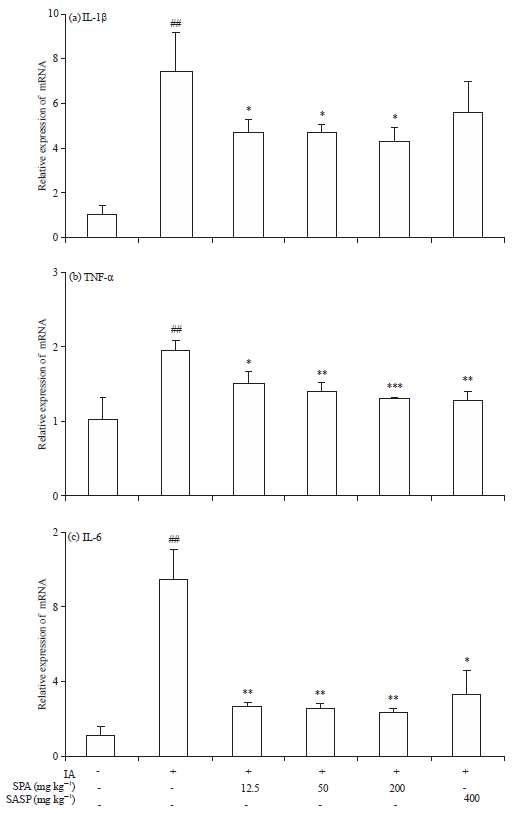
Siegesbeckia pubescens Attenuates Iodoacetamide-induced Colitis in Rats
Institute of Materia Medica, Zhejiang Academy of Medical Sciences, 310013 Hangzhou, China
Tian-li Teng
Institute of Materia Medica, Zhejiang Academy of Medical Sciences, 310013 Hangzhou, China Department of Pharmacy, The First Affiliated Hospital, College of Medicine, Zhejiang University, 310003 Hangzhou, China
Qin Li
Institute of Materia Medica, Zhejiang Academy of Medical Sciences, 310013 Hangzhou, China
Shi-fang Xu
Institute of Materia Medica, Zhejiang Academy of Medical Sciences, 310013 Hangzhou, China
Qun Chen
Ningbo College of Health Sciences, 315100 Ningbo, China
Xiao-yu Li
Institute of Materia Medica, Zhejiang Academy of Medical Sciences, 310013 Hangzhou, China
Yi-ping Ye
Institute of Materia Medica, Zhejiang Academy of Medical Sciences, 310013 Hangzhou, China