Research Article
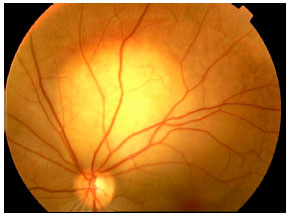
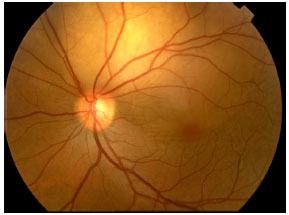
Choroidal Metastasis as First Manifestation Following Breast Conserving Surgery for Breast Cancer: Case Report
Department of Surgery, Zonguldak Karaehnas University, The School of Medicine
Atilla Alpay
Department of Oplitalinology, Zongwdak Karaelinas University, The School of Medicnie, Kozlu-Zongwdak, Turkey
Ali U ur Emre
Department of Surgery, Zonguldak Karaehnas University, The School of Medicine
Oge Ta cilar
Department of Surgery, Zonguldak Karaehnas University, The School of Medicine
Blent Hamdi Ucan
Department of Surgery, Zonguldak Karaehnas University, The School of Medicine
Hakan Balbaloglu
Department of Surgery, Zonguldak Karaehnas University, The School of Medicine
Sami Dibeklioglu
Department of Surgery, Zonguldak Karaehnas University, The School of Medicine
Mustafa Comert
Department of Surgery, Zonguldak Karaehnas University, The School of Medicine