Research Article
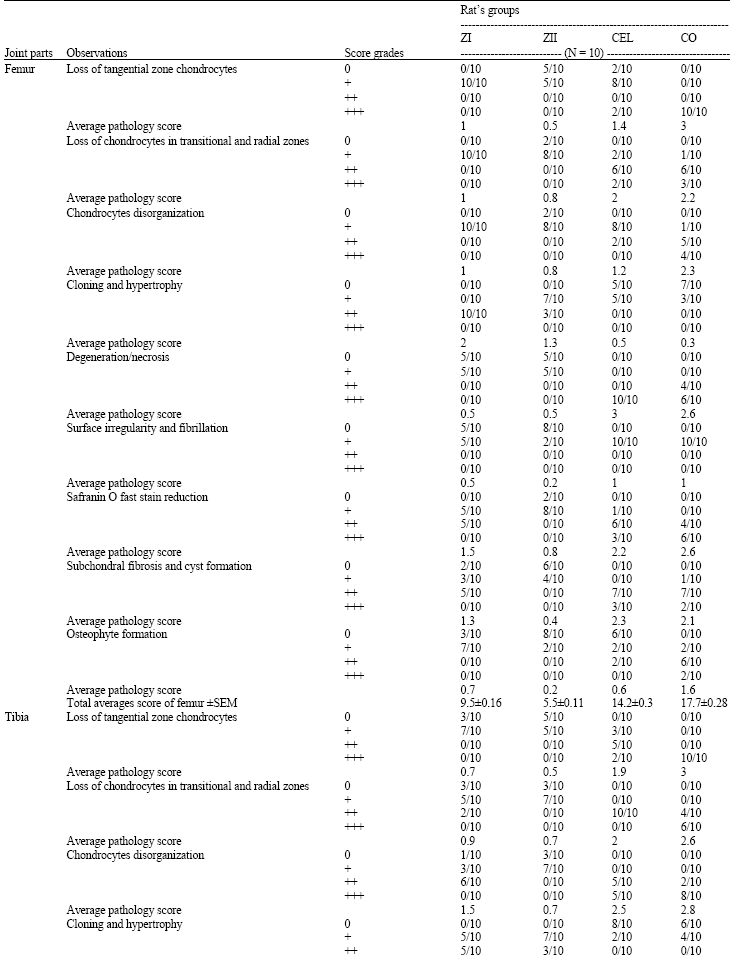
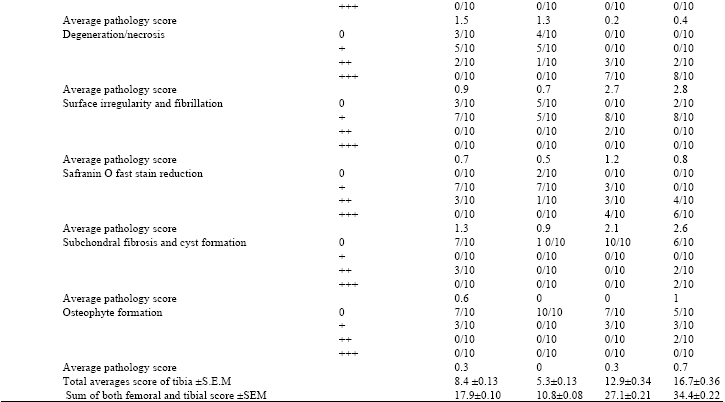
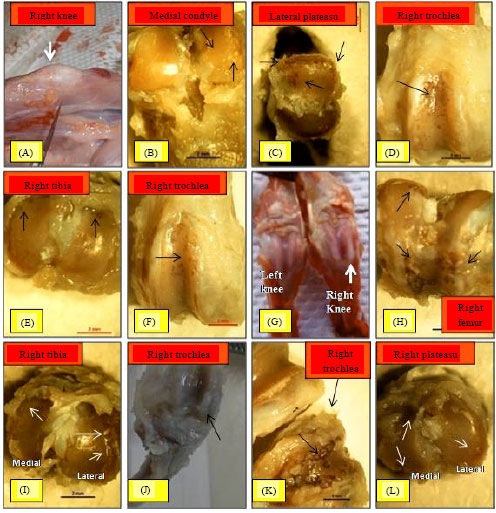
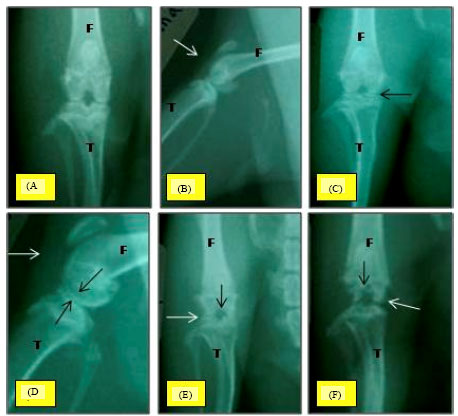
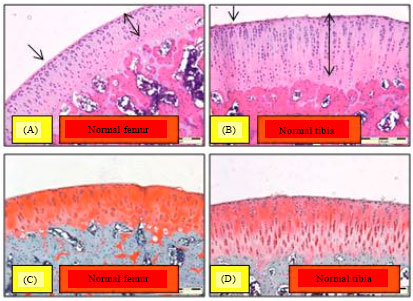
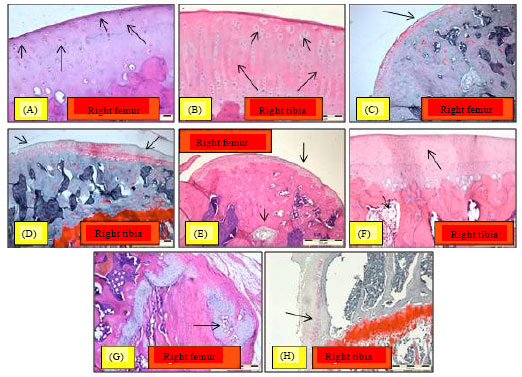
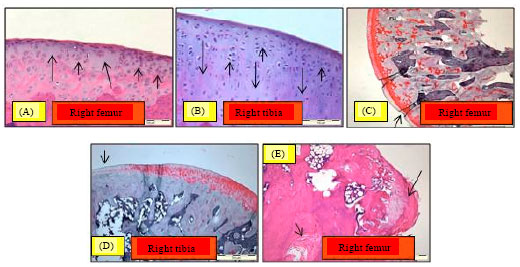
Chondroprotective Effect of Zerumbone on Monosodium Iodoacetate Induced Osteoarthritis in Rats
Department of Preclinical Sciences, Faculty of Veterinary Medicine, University Putra Malaysia, 43400, Serdang, Selangor, Malaysia
S. Ganabadi
Department of Preclinical Sciences, Faculty of Veterinary Medicine, University Putra Malaysia, 43400, Serdang, Selangor, Malaysia
S. Fakurazi
Department of Human Anatomy, Faculty of Medicine and Health Sciences, University Putra Malaysia, 43400, Serdang, Selangor, Malaysia
H. Yaakub
Department of Animal Science, Faculty of Agriculture, University Putra Malaysia, 43400, Serdang, Selangor, Malaysia
M. Lip
Analytical Laboratory and Quality Assurance Programmed Technical Services Centre, Mardi, P.O. Box 12301, Kuala Lumpure, General Post Office 50774, Malaysia