Research Article
Encopresis: From a Surgical View in Comparison to Psychiatric Management
Department of Surgery, Faculty of Medicine, Al-Azher University, New Damietta, Egypt
M. Balbola
Department of Surgery, Faculty of Medicine, Al-Azher University, New Damietta, Egypt
M. Shahin
Department of Surgery, Faculty of Medicine, Al-Azher University, New Damietta, Egypt
N. Salm
Department of Surgery, Faculty of Medicine, Al-Azher University, New Damietta, Egypt
G. Khafagy
Department of Pediatric, Kafer El-sheikh LRC, Egypt
Us. Gheida
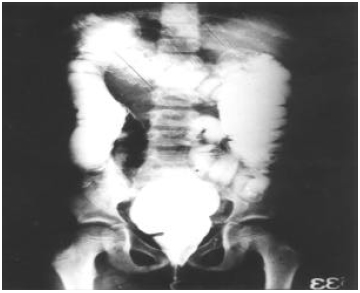
Department of Radiology, Faculty of Medicine, Tanta University, Egypt
Sh. El-Maadawy
Department of Psychiatry, Ministry of Health Hospitals, Egypt