Research Article
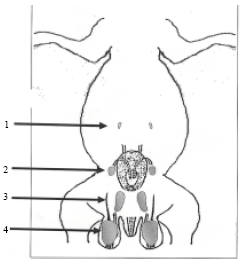
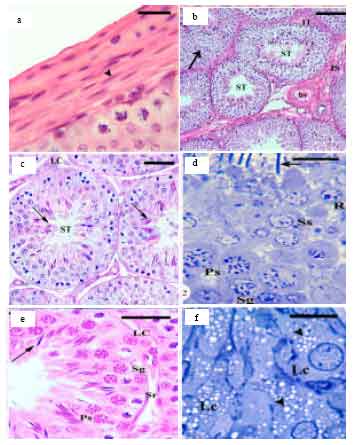
Histological and Histomorphometric Changes of the Rabbit Testis During Postnatal Development
Department of Histology, Faculty of Veterinary Medicine, South Valley University, Qena, Egypt
Mahmoud M. Abd-Elhamied
Department of Histology, Faculty of Veterinary Medicine, South Valley University, Qena, Egypt
Gamal K.M. Ali
Department of Anatomy and Histology, Assiut University, Assiut, Egypt