ABSTRACT
The survey-study was conducted in equids rich 64 districts of 14 states of India to fetch the information on antimicrobial drug use and problems associated with antimicrobial chemotherapy in equids so that future research and extension activities can be planned. The study was a format based survey of equine practitioners (532) in different equids rich districts of 14 states of India. The format information analyzed in Exel® worksheat revealed that more than 40% vets used one or more of the 75 antimicrobials in their 75% patients. Use of ampicillin, ampicillin+cloxacillin, amoxycillin+cloxacillin, gentamicin and strepto-penicillin were ranked one through five by equine practitioners. Intramuscular route remained the preferred one for antimicrobial administration. About 80% vets used antimicrobial formulations meant for human use in equine practice. Penicillins and tetracyclines were the most common antibiotics with adverse actions. Almost 50% practitioners prescribed supportive therapy in their 50% patients. The most common supportive medicines used included antihistaminics followed by liver tonics, vitamins, cortisone, probiotics and mineral supplements. The commonest criterion for prescribing antimicrobials was the clinical diagnosis and least valued was the treatment history. More than 80% vets expressed the need of antibiotic sensitivity testing at least in selected cases. The study concludes that antimicrobials, including those intended for human use, are commonly prescribed in equine practice. Most of the equine practitioners used antimicrobials almost indiscriminately in equids because facilities for antimicrobial sensitivity assay are rarely available.
PDF Abstract XML References Citation
How to cite this article
URL: https://scialert.net/abstract/?doi=rjvs.2010.165.178
INTRODUCTION
In most of the equids rearing countries including developed countries it is a general complaint that antibiotics are used indiscriminately and many a time without any real need (Oglesby, 2009). Several attempts have been made to restrict to minimum antibiotic use in equids (Britt and Byars, 1997; Oglesby, 2009) however, not only veterinarians but owners often forget recommendations and tend to over use all newer antimicrobials which may cause antibiotic associated problems not only of equids but probably of human too and also plays important role in generation of antimicrobial resistant microbes in environment. Looking at the problem, US congressional committee held a hearing in 2009 on a bill to propose severe restrictions on the use of antibiotics in animals (Rosenthal, 2009). Although, all are concerned with use of antimicrobials in animals including equids, hardly few studies have been undertaken to understand the question of prescription of antimicrobials by veterinary practitioners.
Emergence of Multiple Drug Resistance (MDR) is often reported to be associated with indiscriminate use of antimicrobials in veterinary and medical practice (WHO, 1997). In India, several highly drug resistant and multiple drug resistant strains of zoonotic importance have been reported in last few years from animals (Singh et al., 2007, 2009; Singh, 2009a, b). However, little is understood about the antimicrobial drug use in animals in India. This study was undertaken with the aim to understand why, when, to whom, what antibiotics and what supporting prescriptions are administered by veterinarians to equids in India.
In different parts of world many surveys involving practicing veterinarians have been conducted to design the research strategies and even to solve other professional problems. Some of the important surveys were conducted to know the prevalence of medical problems of adult horses in Colarado (Traub-Dargatz et al., 1991), prevalence of chronic obstructive diseases (COPD) in horses of Lousiana (Seahorn et al., 2006) and existence of equine borreliosis (Lyme disease) in Germany (Gall and Pfister, 2006), prevalence of stomatitis and other diseases in India (Letchworth et al., 1999; Singh et al., 2010). Besides, surveys are conducted to find out the ailments of horses needing maximum research (AAEP, 2004).
However, only a few surveys were conducted to know the use of specific medicines in veterinary practice viz., diclofenec in Tanzania (WOAH, 2008), efficacy of polysulphated glycosamine-O-glycan in treatment of degenerative joint diseases of equids (Caron et al., 1996), the best options for control of equine colic (Mair and White, 2008) and helminthes infestation in Ireland (O'Meara and Mulcahy, 2002) and South Africa (Matthee et al., 2002). Although, laboratory based surveys have been undertaken to assess the prevalence of glanders, equine infectious anemia (EIA), equine influenza (EIV), equine herpes viruses (EHV-1, 4), trypanosomiasis (surra), salmonellosis, brucellosis and babesiosis in India (Malhotra et al., 1978; Uppal and Yadav, 1987; Singh et al., 1993, 2001, 2007; Gupta et al., 1996; Virmani et al., 2008), no survey of equine practitioners was about the use of antimicrobial drugs and associated problems in equids. Therefore, the present study was undertaken on equine practitioners spread all over India with major objective to know the pattern and rationale of antimicrobial drug uses in equids in India.
MATERIALS AND METHODS
Survey Proforma
The survey study was formulated in year 2006 at NRC Equines, Hissar and continued till October 2008. It was designed to have 14 questions (Table 1) with the aim to get information about type of practice; area of practice, clientele, antimicrobial drugs used and associated problems of equids in India. Proforma were sent to each selected district’s chief veterinary officer or secretary of veterinary association at district level. A total of 64 districts, each having >3000 equids (as per 17th Livestock Census, 2003; http://www.dms.nic.in/ami/livestocktotal.aspx) were selected in 14 states (Andhra Pradesh, Delhi, Gujarat, Haryana, Himachal Pradesh, Jharkhand, Karnataka, Maharashtra, Manipur, Punjab, Rajasthan, Uttrakhand, Uttar Pradesh and West Bengal). Proformas were also sent to 30 private stud farms and four government equine breeding/stud farms.
In Haryana, Uttar Pradesh, Punjab and Rajasthan proforma were given to each of the incharges of Veterinary training centers (for veterinary refresher courses) for getting information from veterinarians coming for training. A total of 2000 proformas were sent to veterinarians either through post or in person.
| Table 1: | Questionnaire sent to veterinarians in different states working in various organizations in India |
 | |
Statistical Analysis
Information contained in survey proforma was put into Microsoft ExcelR spread sheet for analyzing the information through χ2 goodness-of-fit and Z-tests.
RESULTS
A total of 532 (26.6%) questionnaires were received back from equine practitioners from 14 states of India namely; Andhra Pradesh (1), Delhi (4), Gujarat (7), Haryana (277), Himachal Pradesh (20), Jharkhand (3), Karnataka (1), Maharashtra (5), Manipur (1), Punjab (61), Rajasthan (20), Uttrakhand (3), Uttar Pradesh (UP, 126) and West Bengal (3). Response was better from vets practicing in Haryana (55.4%), Uttar Pradesh (42%) and Punjab (20.3%) while poor from those in Karnataka (2.5%) and West Bengal (3%) states. The details of responses from veterinary practitioners pertaining to number of total animals treated and number of equine patients treated per year; types of their clients, frequency of use of antimicrobial drugs (AMDs), number of AMDs in list of their preferential use and routes of antimicrobial drug administration have been shown in Table 2. Information regarding use of AMDs intended for human use in equids, AMDs harming equids, number of antibiotics reported to harm, number of medicines used as supportive treatment to counter the bad effect of AMD therapy, need of supportive therapy, criteria used for writing AMDS in prescription availability of probiotics in market and requirement of antimicrobial drug sensitivity testing are presented in Table 3.
| Table 2: | Analysis of response of equine practitioners in different parts of India working in different organizations regarding use of antimicrobials and associated problems |
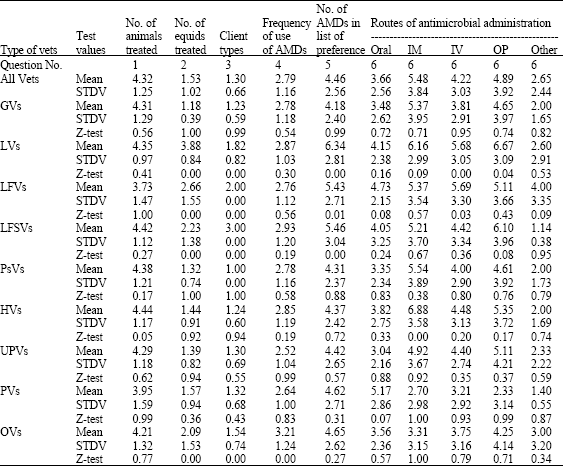 | |
| AMDs: Antimicrobial drug formulations; GVs: Vets treating <100 equines per year; LVs: Vets treating large number of equines (>100/year); LFVs: Vets working on organized farms; LFSVs: Vets treating equids of both, peasants and at organized farms; PsVs: Vets treating animals of peasants (small farmers) only, HVs: Haryana state vets; UPVs: Uttar Pradesh state vets; PVs: Punjab state vets; OVs: Vets in other sates; Mean: Average of the respondents; STDV: Standard deviation of the respondents; Z-test, Z test values using mean and standard deviations of all the 532 respondents as reference, figures against it indicate level of significance, lower the figure higher the significant difference, 0.01 means difference at level of 1% significance | |
Number of Total Animals Treated
Each year a vet, on an average, treats more than one thousand animals. However, in Punjab significantly lower (z, 0.05) and in Haryana significantly (z, 0.05) higher (number of animals were treated by each vet (Table 2).
No. of Equids Treated
Of the total animals treated by each vet only a fraction (~5%) was of equids including horses, mules and donkeys (Table 2). On the basis of number of equids treated practitioners were classified into two groups, viz., general vets (GVs, 463), treating up to 100 equids per year and large vets (LVs, 68), treating more than 100 equids per year.
Types of Clients
On the basis of clientele equine practitioners were grouped as clinicians working on equine stud farms (LFVs, 44), treating patients both at farm and of general public i.e., peasants (LFSVs, 57) and vets treating equids at state veterinary hospitals, i.e., peasants’ vets (PsVs, 422).
| Table 3: | Analysis of response of equine practitioners in different parts of India working in different organizations regarding use of antimicrobials and associated problems |
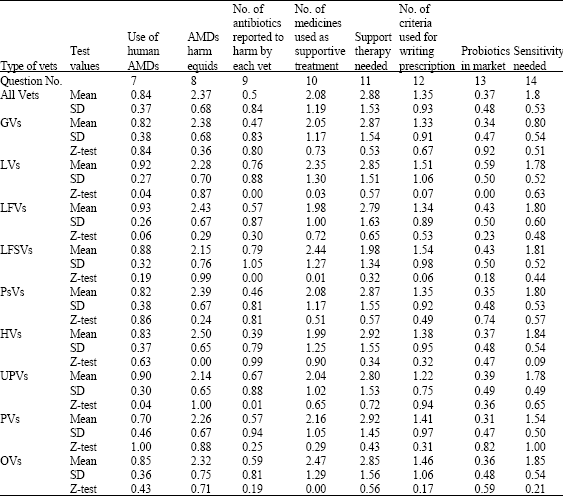 | |
| AMDs: Antimicrobial drug formulations; GVs: Vets treating <100 equines per year; LVs: Vets treating large number of equines (>100/year); LFVs: Vets working on organized farms; LFSVs: Vets treating equids of both, peasants and at organized farms; PsVs: Vets treating animals of peasants (small farmers) only, HVs: Haryana state vets; UPVs: Uttar Pradesh state vets; PVs: Punjab state vets; OVs: vets in other sates; Mean: Average of the respondents; SD: Standard deviation; Z-test, Z test values using mean and standard deviations of all the 532 respondents as reference, figures against it indicate level of significance, lower the figure higher the significant difference, 0.01 means difference at level of 1% significance | |
Prescription of Antibiotics/Antimicrobials
A total of 94.5% vets responded to the question concerning to frequency of use of antimicrobials in equids (Table 2). More than 40% vets used antimicrobials in >75% patients. However, vets in states other than Haryana, Punjab and UP ~23% used antimicrobials in 75% patients (Table 2). Inter class comparison revealed that use of antimicrobials was significantly more common (χ2 0.05) by LVs. More number of GVs (~13%) used antimicrobials in all cases they treat. In UP, Punjab and Haryana >70% vets used antimicrobials in >50% patients (2) but in other states antibiotic use was significantly high (z, 0.00).
Antimicrobials used
On an average 4.49±2.53 antimicrobials were in preferred list of each vet (Table 2) but significantly (z, 0.01) more numbers were in preference list of LVs, LFVs and LFSVs (5.43±2.71 to 6.34±2.81). None of the 75 antimicrobial/antimicrobial combinations was preferred by vets of all types of practice in different localities (Table 4). A total of 21 antimicrobials or their combinations were identified as the commonly prescribed (Table 5) ones, i.e., used by at least 10% of vets of one or other class (Table 6).
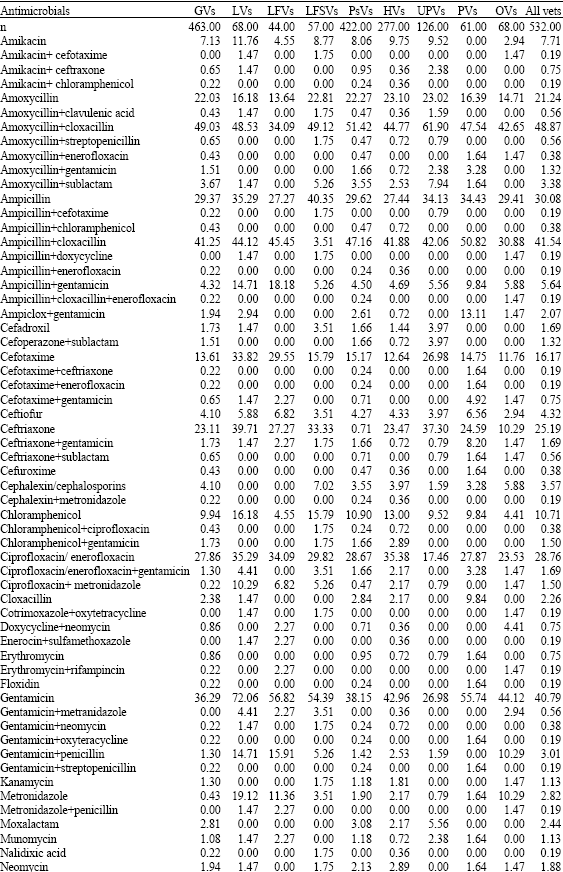
| Table 4: | Common antimicrobials used to treat diseases/ ailments of equids reported to be common in India by different classes of vets |
 | |
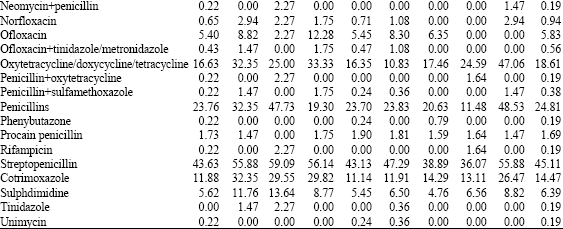 | |
| Gvs: Vets treating <100 equines per year; LVs: Vets treating large number of equines (>100/year); LFVs: Vets working on organized farms; LFSVs: Vets treating equids of both, peasants and at organized farms; PsVs: Vets treating animals of peasants (small farmers) only, HVs: Haryana state Vets; UPVs: Uttar Pradesh state Vets; Pvs: Punjab stateVets; OVs: Vets in other sates | |
| Table 5: | Most commonly used antimicrobial formulations in equids in India by different classes of vets |
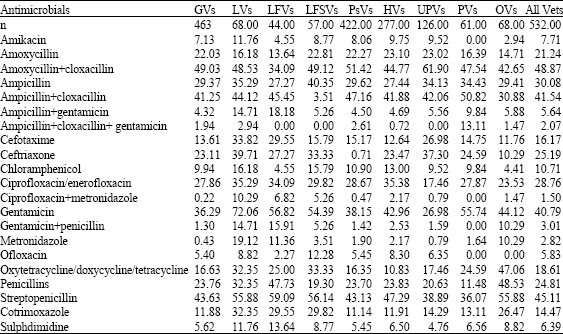 | |
| GVs: Vets treating <100 equines per year; LVs: Vets treating large number of equines (>100/year); LFVs: Vets working on organized farms; LFSVs: Vets treating equids of both, peasants and at organized farms; PsVs: Vets treating animals of peasants (small farmers) only, HVs: Haryana state Vets; UPVs: Uttar Pradesh state Vets; Pvs: Punjab stateVets; OVs: Vets in other sates | |
Of these five most common were amoxycillin+ cloxacillin (48.9%), streptopenicillin (45.1%), ampicillin+ cloxacillin (41.5%), gentamicin (40.8%) and ampicillin (30.1%). However, LFVs and LFSVs ranked use of ampicillin and ampicillin+cloxacillin at a lower preference than other vets (Table 5). Although, there was difference in the preference of individual antimicrobial, overall correlation was good (r≥0.8) among different classes of vets with reference to use of different antimicrobials.
| Table 6: | Common antimicrobials harming equids as appreciated by different classes of vets in India |
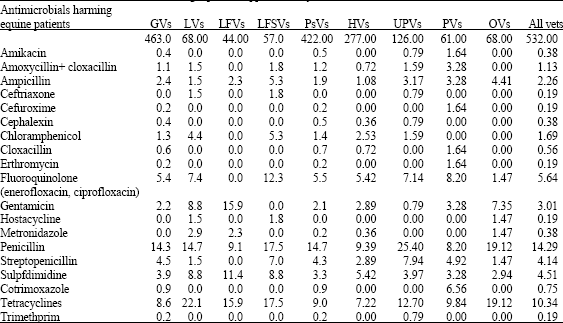 | |
| Gvs: Vets Ttreating only <100 equines per year; LVs: Vets treating large number of equines (>100/year); LFVs: Vets working on large farms; LFSVs: Vets treating equids of both, peasants and large farmers; PsVs: Vets treating animals of peasants (small farmers) only, HVs: Haryana state Vets; UPVs, Uttar Pradesh state Vets; Pvs: Punjab stateVets; OVs: Vets in other sates | |
Routes of Antimicrobial Drug Administration
On an average more than one route was followed by each respondent (1.63±0.94) for antibiotic drug use without any significant difference among vets of different regions and type of equine practice. Intramuscular (IM) route was the most preferred one (Table 2) for antimicrobial administrations in equids among all vets but use of other routes varied in different areas and by various types of practitioners. Many different routes were used by LFVs, LVs and LFSVs. The IM route was preferred by less vets (~22%) in other states than oral route (>30%). In Uttar Pradesh, ~29% vets used oral+parentral (OP) combination. Significantly (χ2 <0.1) more LVs used oral (~38%) and intravenous (~60%) administration of antimicrobials than GVs. Route preference differed significantly among different types of vets particularly towards adoption of intravenous, IM and OP routes (Table 2).
Antimicrobial for Human can be used in Equids
A total of 95.1% practitioners answered the question regarding use of human antimicrobial drug formulations (AMDs) in equids and ~80% vets accepted their use in equine practice (Table 3). Significantly high number of Punjab Vets (PVs) said no to human antimicrobials (~28%) however, acceptability was the maximum in UP equine clinicians (86.5%).
Antimicrobials Harm Equids
Significantly (χ2 0.1) more LFVS and vets of other states (OVs) than UP, Haryana and Punjab mentioned that antimicrobials often harm to equids. More than 50% LFVs and PsVs stated that antibiotics do not harm or rarely harm equids (Table 3).
Common Antimicrobials which Harm Equids
A total of 19 antimicrobials were reported to be associated with adverse effects in equids (Table 6). All vets recognized that penicillins and tetracyclines were the two main harmful antibiotics but for other antibiotics observations varied significantly (χ2 <0.07).
| Table 7: | Percentage of veterinarians using different medicines for supportive therapy in equids and criteria followed for prescribing antimicrobials to their equine patients |
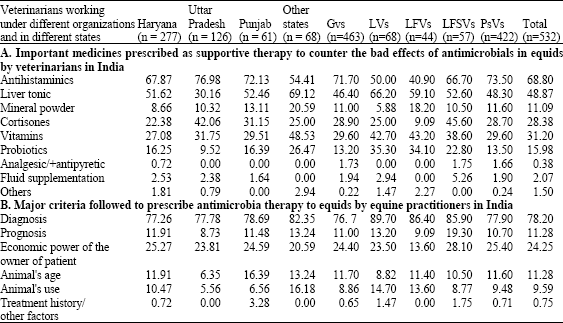 | |
| Gvs: Vets treating <100 equines per year; LVs: Vets treating large number of equines (>100/year); LFVs: Vets working on organized farms; LFSVs: Vets treating equids of both, peasants and at organized farms; PsVs: Vets treating animals of peasants (small farmers) only | |
More LVs and LFVs blamed sulphadimidine and gentamicin, more LVs, LFVs, LFSVs, OVs, UPVs, PVs opined for adverse effects of tetracyclines while many LFVS considered fluoroquinolones more harmful. Only PVs observed harmful effects of cotrimoxazole and cefuroxime in equine patients while adverse effect of hostacycline was reported by OVs only.
Supportive Therapies used to Counter Bad Effects of Antimicrobials
On an average 2.09±1.18 medicines (Table 3) were used to counter adverse effects of antimicrobials by all the respondents. However, significantly more (z, 0.03) medicines were prescribed in supportive therapy by LVs (2.35±1.30) and LFSVs (2.44±1.27, z, 0.01). Antihistaminics were the commonest support followed by liver tonics, vitamins, cortisone, probiotics and mineral supplements (Table 7). Intravenous fluid, analgesics and antipyretics, chelated arginine and sodium bicarbonates were among other rare choices. However, use of different supportive therapies varied significantly among different classes of vets viz., use of antihisaminics was significantly less common (χ2 <0.05) by LVs and LFVs but more common by PsVs and GVs. Liver tonics were used commonly (χ2 <0.02) by all (in >50% patients) but UPVs. Use of mineral powder was significantly high (χ2 <0.06) by OVs (>20%). Cortisones were more commonly (χ2 <0.01) used by UPVs (by >42%) and LFSVs (by >45%) but rarely by LFVs (by 9.1%). Use of vitamins was significantly more (χ2 <0.04) common by OVs, PVs, HVs (>48%) than UPVs (~31%). Probiotics were more commonly (χ2 <0.01) prescribed by OVs (>26%), LVs (>35%) and LFVs (>34%) than PsVs (~13%).
Supportive Therapy is Required
With reference to need of supportive treatment (Table 3) in equine patients, more than 20% vets were in favour of giving it to all patients, however only 7% LFVS were with this opinion. More than 40% vets prescribe supportive treatment in >75% cases while >50% for >50% equids they treated.
Criteria for Prescribing Antimicrobials
The question was answered by 91.7% respondents (Table 3) and many of them used more than one criterion for prescribing antibiotics (1.36±0.92). Clinical diagnosis was the non-disputed most common single criterion (>78%) among all the vets and treatment history was the least valued one (Table 7). There was hardly any significant difference regarding criteria for prescribing antibiotics (Table 2) and supportive treatment (Table 7) among vets of different states. However, LVs (1.51±1.06; z, 0.08) and LFSVs (1.54±0.98; z, 0.07) considered more number of reasons for prescribing antimicrobials (Table 3).
Availability of Probiotics in Market
Of the 86.6% respondents majority of vets stated non-availability of probiotics in market (Table 2). However, more LVs find probiotics available (![]() 0.59) than PsVs (
0.59) than PsVs (![]() 0.35) in local markets.
0.35) in local markets.
Antimicrobial Sensitivity Testing is Required
More than 80% vets felt the need of antibiotic sensitivity testing at least in selected cases. More than 40% vets in Punjab felt antibiotic sensitivity testing essential in all cases. However, significant number of HVs said that it is not required for equids (Table 3).
DISCUSSION
Except a few surveys on use of a selected medication for specific purpose (Caron et al., 1996; Matthee et al., 2002; O'Meara and Mulcahy, 2002; Mair and White, 2008; WOAH, 2008) there is dearth of information on in-field-use of different antimicrobials in veterinary practice and still less information is available from equine practice. Only little is known about the problems and notions of the equine practitioners who graduated long back and working almost in isolation since long, thus this study reveals many of the significant facts about the use of antimicrobials in equine veterinary practitioners in India.
Overall response of veterinarians to survey proforma (26.6%) was quite satisfactory in concurrence to earlier surveys (O'Meara and Mulcahy, 2002; WOAH, 2008). A better response of vets to survey in Haryana and Uttar Pradesh (UP) was probably due to personal visits and interaction of the investigator with veterinarians at veterinary training centers.
It appeared that either only a small fraction of equids needed veterinary care or a small fraction of sick animals was brought to veterinary hospitals. In general, majority of owners of equids in India are often very poor and always hand to mouth (Singh et al., 2007) and it is their normal assumption that treatment of equids in veterinary hospitals is dearer than conventional house hold remedies.
Although, majority of the vets treated more than a thousand animals each year in different parts of India irrespective of their kind of practice, in Punjab, comparatively less number of animals were treated by vet. It might be either due to comparatively more vets to serve the defined population or just might be because of healthier climate in the state.
It was evident that large numbers of veterinarians go for prescribing antimicrobials to their equine patients. The major reason behind use of antibiotics in high frequency might be due to demand of a sure shot treatment by the owners to avoid the frequent visits and also the need of clinicians to prove him/her the best.
Use of antimicrobials in equids appeared to be too common for most of the clinicians irrespective of state or type of practice and most of the clinicians apply multiple criteria for prescribing an antimicrobial drug to equids (1.36±0.92) but they rarely give any importance to previous treatment/ prescription. It might be either due to the fact that most of the equids brought to veterinary hospital have history of medication with ethnic herbal medicines or treated by non-qualified people (Singh et al., 2007). However, it may not be true for all the cases particularly may not be true for the veterinarians working on organized farms. It is not understood from the study, why clinicians ignore past treatment prescription before using antimicrobials, why they believe that the drug prescribed by them will work while the same drug prescribed by earlier practitioner shall fail.
A large number (75) of antimicrobials were found to be prescribed by equine veterinary practitioners and many of the antimicrobials were those which are often restricted for use in equine practice. On the basis of pharmacological studies and earlier clinical uses (Hirsh and Jang, 1987; Sweeney and Boy, 1993; Hirsh, 1999) tetracyclines, chloramphenicol, fluoroquinolones, cefotaxime, ceftriaxone and gentamicin (in foals) are contraindicated in equids because they may lead to various complications like colic (Sweeney and Boy, 1993; Baverud et al., 1998). However, many of these contraband antimicrobials were in the list of most preferred antimicrobials, specifically of the equine practitioners treating large number of equids or working on stud farms. The reasons behind the trend of using contraindicated antimicrobials though not clear might be ignorance or perceived benefits of the drugs. However, it is difficult to reason exactly, unless the systematic work is carried out, that either some of the health problems in equids are associated or not with preferential use of specific contraband antimicrobials in different regions of India. It is obvious and interesting that those contraindicated antibiotics (tetracyclines, gentamicin and fluoroquinolones) which are reported to cause more problems in equids were used to the maximum extent by the reporting group of the practitioners (LVs, LFVs and LFSVs).
The PsVs rarely used ceftriaxone while it was one of the preferred medicines by 33-40% of other vets; the reason might be its high cost per dose as PsVs often go for cheaper broad spectrum antimicrobials considering economy of their clients (Singh et al., 2007).
More use of penicillin, streptopenicillin, rifampicin, rifampin+erythromycin, penicillin+ neomycine and nalidixic acid by LFVs might be because of their association with problems of breeding, foal pneumonia and diarrhoea. However, why they (LFVs) used chloramphenicol+ciprofloxacin, oxytetracycline+penicillin at high preference can not be explained.
A battery of medicines was used by clinicians to counter the adverse effect of antimicrobial therapy. Use of cortisone, vitamins and antihistaminics might be justified for countering the adverse effect of reactogenic antibiotics and similarly the use of probiotics to correct the disturbed microflora as a consequence of antimicrobial therapy (Sweeney and Boy, 1993; Parraga et al., 1997; Hogenauer et al., 1998; Kania and Kania, 2003; Cote and Buchman, 2006; Gougoulias et al., 2007). However, use of mineral powder by OVs, mostly working on organized farms, in significantly high (χ2 <0.06) frequency (>20%) needs further studies to know how the minerals might modulate the harmful effect of antimicrobials.
It is now established fact that antimicrobial therapy modulates the normal microflora of patients often leading to serious after-effects as colic and diarrhoea in equids (Sweeney and Boy, 1993; Baverud et al., 1998; Hogenauer et al., 1998; Kania and Kania, 2003) thus the use of supportive therapy in high frequency by most of the vets appeared to be desirable. Role of probiotics is well established in management of problems created by disturbed normal microflora after antimicrobial therapy (Cote and Buchman, 2006; Gougoulias et al., 2007) but availability of proper probiotics preparations for equine use probably limited its inclusion in prescription of equine practitioners in India at regular basis.
Role of antibiotic sensitivity assays before prescribing a course of antimicrobial therapy was felt long back but even in developed countries in equines, most of the problems associated with infections necessitate the prescription of antibiotic drug before the results from laboratory are available (Hirsh and Jang, 1987), but it can always be used in selected cases as felt by most of the equine practitioners in India.
The study provided a valuable new information regarding use of antimicrobial drugs in equids and associated problems. The finding can be used for future planning on formulation and marketing of AMDs and supportive medicines for equine practice in India and other countries with similar equine husbandry practices.
ACKNOWLEDGMENTS
Author is thankful to all the vets who responded in the study and to all those officials of different states who helped in distribution and recollection of the questionnaires. Author specially acknowledges Dr. BR Gulati, Dr. SK Khurana (of NRC Equines Hissar), Dr. RK Sindhu (HVTI, Hissar), Dr. A K Kushwah (DO, Rampur), Dr. Bhudeo Singh (VO, Chandpur), Dr. HS Yadav (VO, Lucknow) and Dr. RP Yadav (VO, Aligarh) for their help in collection of proforma from various districts of different states.
REFERENCES
- Britt, B. and T.D. Byars, 1997. Hagyard-davidson-McGee. Proc. Annu. Convent. AAEP, 43: 170-177.
Direct Link - Gall, Y. and K. Pfister, 2006. Survey on the subject of equine Lyme borreliosis. Proceedings of the 8th International Potsdam Symposium on Tick-borne Diseases (IPS-VIII), May 22, Munich, Germany, pp: 274-279.
Direct Link - Gougoulias, C., K.M. Tuohy and G.R. Gibson, 2007. Dietary-based gut flora modulation against Clostridium difficile onset. Food Sci. Technol. Bull. Functional Foods, 4: 31-41.
Direct Link - Hirsh, D.C. and S.S. Jang, 1987. Antimicrobic susceptibility of bacterial pathogens from horses. Vet. Clin. North Am. Equine Pract., 3: 181-190.
PubMedDirect Link - Hogenauer, C., H.F. Hammer, G.J. Krejs and E.C. Reisinger, 1998. Mechanisms and management of antibiotic-associated diarrhea. Clinl. Infect. Dis., 27: 702-710.
Direct Link - Kania, B.F. and K. Kania, 2003. Pharmacological and toxicological aspects of combination of beta-lactam and aminoglycoside antibiotic, prednisolone and procaine hydrochloride on the example of Vetramycin. Pol. J. Vet. Sci., 6: 279-296.
PubMedDirect Link - Mair, T.S. and N.A. White, 2008. The creation of an international audit and database of equine colic surgery: survey of attitudes of surgeons. Equine Vet. J., 40: 400-404.
CrossRef - Matthee, S., F.H. Dreyer, W.A. Hoffmann and F.E. van Niekerk, 2002. An introductory survey of helminth control practices in South Africa and anthelmintic resistance on Thoroughbred stud farms in the Western Cape Province. J. South African Vet. Assoc., 73: 195-200.
PubMed - O'Meara, B. and G. Mulcahy, 2002. A survey of helminth control practices in equine establishments in Ireland. Vet. Parasitol., 109: 101-110.
CrossRef - Parraga, M.E., S.J. Spier, M. Thurmond and D. Hirsh, 1997. A clinical trial of probiotic administration for prevention of Salmonella shedding in the postoperative period in horses with colic. Vet. Int. Med., 11: 36-41.
PubMedDirect Link - Singh, B.K., M.P. Yadav and S.C. Tiwari, 2001. Neutralizing and complement-fixing monoclonal antibodies as an aid to the diagnosis of equine herpesvirus-1 infection. Vet. Res. Commun., 25: 675-686.
PubMed - Singh, B.K., R. Sinclair, A.K. Gupta, P.K. Uppal, M.P. Yadav and J.A. Mumford, 1993. Production of monoclonal antibodies against equine influenza A/Equi-2 (H3N8) Indian isolate. Indian J. Exp. Biol., 31: 774-775.
PubMed - Singh, B.R., J. Jyoti, M. Chandra, N. Babu and G. Sharma, 2009. Drug resistance pattern in Salmonella isolates of equine origin in India. J. Infect. Dev. Countries, 3: 141-147.
Direct Link - Singh, B.R., 2009. Prevalence of vancomycin resistance and multiple drug resistance in enterococci in equids in North India. J. Infect. Dev. Countries, 3: 498-503.
Direct Link - Singh, B.R., M. Chauhan, R.K. Sindhu, B.R. Gulati and S.K. Khurana et al., 2010. Diseases prevalent in equids in India: A survey of veterinary practitioners. Asian J. Anim. Vet. Adv., 5: 143-153.
CrossRefDirect Link - Sweeney, C.R. and M.G. Boy, 1993. Antimicrobial Drug use in Horses. In: Antimicrobial Therapy in Veterinary Medicin, Prescott, F.J. and J.D. Baggot (Eds.). Iowa State University Press, Ames, pp: 410.
CrossRef - Uppal, P.K. and M.P. Yadav, 1987. Outbreak of equine influenza in India. Vet. Record., 121: 569-570.
Direct Link - Virmani, N., B.K. Singh, B.R. Gulati and S. Kumar, 2008. Equine influenza outbreak in India. Vet. Record., 163: 607-608.
Direct Link








