ABSTRACT
Neutrophil Gelatinase-Associated Lipocalin (NGAL) is a sensitive marker of acute kidney injury. It is considered as a novel biomarker for progressive inflammatory process in patients with coronary artery disease. The aim of this study was to evaluate the prognostic significance of NGAL in predicting the in-hospital complications in patients with STEMI treated with fibrinolytic therapy. A total of 52 patients with STEMI treated with fibrinolytic therapy (reteplase) were investigated. Patients with high NGAL (group I) showed significantly higher mortality compared to those with low NGAL (group 2) p = 0.013. By logistic regression shock and pulmonary edema were very strongly correlated with increased NGAL level with a ratio of 0.842, 0.608 and p = 0.0001, respectively. In conclusions, cardiovascular death and in-hospital complications were significantly higher in patients with high NGAL than those with low NGAL. Plasma NGAL is a significant predictor of mortality and in hospital complications in patients with STEMI.
PDF Abstract XML References Citation
How to cite this article
URL: https://scialert.net/abstract/?doi=rjc.2013.10.18
INTRODUCTION
Inflammation and polymorph nuclear neutrophils are considered important in the pathogenesis of acute myocardial infarction (Sahinarslan et al., 2011). Neutrophil activation has been reported in unstable angina and acute myocardial infarction but not in patients with stable angina (Ott et al., 1996; Jaremo et al., 2000; Buffon et al., 2002; Patel et al., 2004; Naruko et al., 2002; Madjid et al., 2004; Sarndahl et al., 2007). This activation seems to precede myocardial injury in patients with AMI (Goldmann et al., 2009).
Neutrophil Gelatinase-Associated Lipocalin (NGAL) is secreted from neutrophils and may increase the proteolytic activity within the atherosclerotic plaque (Sahinarslan et al., 2011). NGAL is a specific matrix metalloproteinase-9 (MMP-9) binder, preventing it from degradation and, thus, maintaining its activity. The MMP-9 is an endopeptidase capable of degrading the extracellular matrix and thought to be associated with atherosclerosis and plaque rupture (Galis et al., 1994; Kai et al., 1998). The formation of a complex with NGAL and matrix metalloproteinase-9 ( MMP-9) is crucial for atherosclerotic plaque erosion and thrombus formation as MMP-9 enhance the action of NGAL (Hemdahl et al., 2006). Therefore, MMP-9 is considered an important mediator of vascular remodeling and plaque instability. Furthermore, high levels of serum MMP-9 are independently associated with adverse cardiovascular outcomes (Blankenberg et al., 2003).
Several novel biomarkers are reported to be associated with an increased risk for mortality in STEMI patients such as N-terminal pro-brain natriuretic peptide (NT-proBNP), glucose, C-reactive protein, creatinine or estimated glomerular filtration rate and cardiac troponin T (cTnT) (Khan et al., 2008; Kosiborod et al., 2005; Ortolani et al., 2008; Anavekar et al., 2004; Aviles et al., 2002). These biomarkers reflect left ventricular dysfunction, glucose metabolism, inflammation status, renal function and myocardial cell damage, respectively.
Neutrophil Gelatinase-Associated Lipocalin (NGAL) is a 25 kDa glycoprotein found in many tissues. Also, many studies proved it as a novel biomarker for early diagnosis of acute kidney injury and its level might reflect the degree of inflammatory process in patients with coronary artery disease (Kafkas et al., 2012). However, the data is inadequate about the prognostic value of NGAL in patients with acute MI. Therefore, the aim of this study was to evaluate the prognostic role of NGAL in patient with STEMI treated with thrombolytic therapy.
MATERIALS AND METHODS
Patients with STEMI, who received fibrinolytic therapy, were admitted to King Saud Medical City from January to April 2013 and included in the study.
Upon presentation in emergency room, patients were subjected to initial clinical assessment that included clinical history, physical examination, 12-lead ECG, continuous ECG monitoring and standard blood tests (including white blood cell, polymorph-nuclear neutrophil counts and cardiac troponin-I (cTnI), Creatinine Kinase (CK) and (CK-MB subtype). All patients received thrombolytic therapy with reteplase a fibrinolytic drug that is similar to recombinant human tissue plasminogen activator alteplase) but the modifications give reteplase a longer half-life of 13-16 min.
However, 8 patients were excluded. The exclusion criteria were end stage renal disease, neoplasia liver disease, renal cardiac or liver transplantation and infection. Because all these can affect serum-NGAL levels.
The estimation of NGAL levels was done by the Alere Triage® NGAL Test. It is a rapid fluorescence immunoassay using the Alere Triage® Meters for rapid, quantitative determination of NGAL in Ethylene Diamine Tetra-acetic Acid (EDTA) anticoagulated whole blood (Fig. 1). The test procedure involved the addition of several drops of EDTA to anticoagulated whole blood or plasma specimen to the sample port on the Test Device. The Test Device was inserted in the Alere Triage® Meter. The Meter was programmed for analysis after the specimen reaction with the reagents within the Test Device.
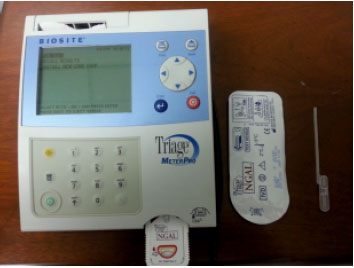 | |
| Fig. 1: | BIOSITE meter and NGAL test device for measuring NGAL level |
The analysis is based on the amount of fluorescence that Meter detects within a measurement zone on the Test Device. The detection of low intensity of fluorescence indicates higher NGAL concentration in the specimen. The result is displayed on the Meter screen in approximately 15-20 min from the addition of specimen. The non-parametric reference range upper limit (95th percentile) is less than 60 Ng mL-1.
Statistical analysis: Categorical data were analyzed in percentage, frequencies (proportion) and Mean±SD (standard Deviation) was used for non-categorical values. According to NGAL levels, the patients were divided into two groups. i.e., group 1 with high NGAl levels and group 2 with low NGAL levels. The comparison between two groups was done using the chi-square test for categorical variables. The comparisons of means were made using the two independent samples student’s t- test to compare the non categorical values of both groups of patients. The correlations between NGAL and the different in-hospital complications were assessed with the Pearson and Spearman’s test of correlation coefficients. Linear logistic regression analysis was done to assess the relationship of increased level of NGAL with the independent variables at 95% confidence interval and p-value were computed from the logistic model. In all analyses, p<0.05 was considered statistically significant. All the statistical data analyses were performed using Statistical Software SPSS Version 20.
RESULTS
Out of 44 patients, 15 patients showed high NGAL level (group 1) and 29 patients had low NGAL (group 2). Data in Table 1 showed the baseline characteristics between the two groups of patients as age was significantly higher in high NGAL as compared to low NGAL group (p = 0.092).
| Table 1: | Baseline characteristics and demographic data of both groups |
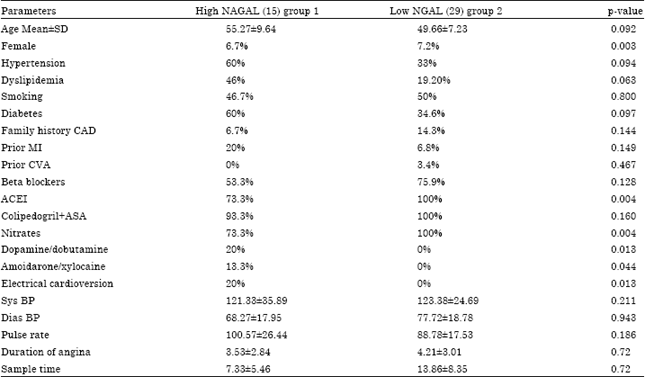 | |
| Chi-square test, SD: Standard deviation, CAD: Coronary artery disease, CVA: Cerebrovascular accident, ACEI: Angiotensin converting enzyme inhibitor | |
The female gender was more common in group 2 (0.003). Also, diabetes mellitus and hypertension were more in group I as compared to low NGAL group (p = 0.094, 0.097, respectively).
High NGAL group were more likely to be treated with inotropes, antiarrhythemic, amoidarone (p = 0.04, 0.01) and received electrical cardioversion (p = 0.013). Group 2 were more likely to be treated with nitrates and ACEI (p-0.004). Duration of angina and sample time were similar in both groups. There were no significant differences in smoking, dyslipidemia, pulse rate, blood pressure and the use of beta blockers or antiplatelets.
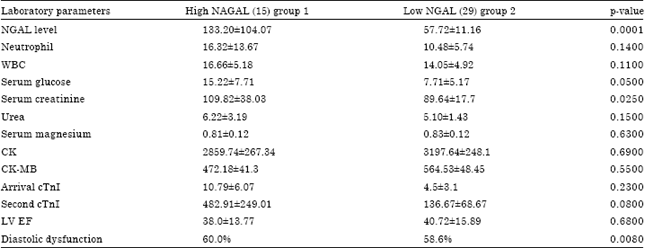
The NGAL level was significantly higher in group 1 than 2 (p = 0.0001). Serum creatinine level was slightly higher in patients with high NGAL as compared to those with low NGAL (109.82±38.03 vs. 89.64±17.7 p = 0.025), Serum glucose levels were significantly higher in patients with high NGAL level (group 1) than group 2 (15.22±7.71 vs. 7.71±5.17 p = 0.05). Other laboratory data such as CK, CK-MB and arrival cTnI were similar between the two groups (Table 2).
In-hospital complications: Patients with high NGAL (group 1) showed significantly higher incidence of in-hospital complications as compared to group 2 (low NGAL) as shown in Table 3.
| Table 2: | Laboratory data for both groups of patients high and low NGAL |
 | |
| Table 3: | In-hospital complications for both groups of patients |
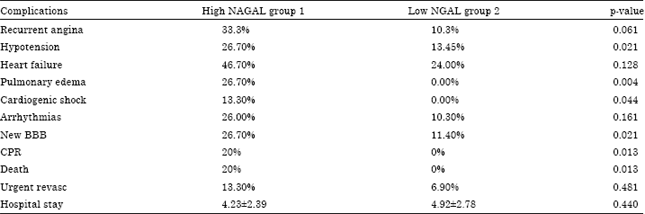 | |
Recurrent angina was frequent in Group I as compared to group 2 (33.3 vs. 10.3% p = 0.061). The hypotension and cardiogenic shock were common in group 1 (26.7 vs. 13.45% p = 0.02 and 13.3 vs. 0% p = 0.044).
However, 4 (26.7%) patients in group 1 developed acute pulmonary edema versus none of patients in group 2 (low NGAL p = 0.004). Also, four patients in group 1 showed new right bundle branch block in the ECG as compared to five in group 2 (26.7 vs. 11.4% p = 0.02) during hospitalization. Furthermore, none of the patients from group 2 (low NGAL level) died as compared to three (20%) patients in group 1 (p = 0.013) while two of them arrested in the first 2 h in the emergency room and the third one died after 72 h.
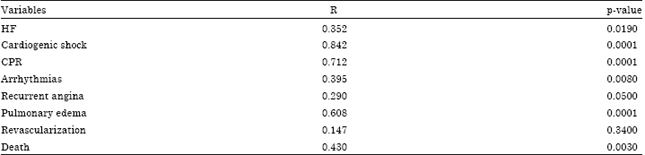
The correlation coefficients for the association between serum NGAL and in-hospital complications are listed in Table 4. All showed significantly strong positive correlation with NGAL level. The cardiogenic shock, Cardio-Pulmonary Resuscitation (CPR) and pulmonary edema showed a very strong correlation (r) with a value of 0.842, 0.712, 0.608 at p = 0.0001, respectively). Heart failure and arrhythmias showed moderately strong correlation with NGAL levels (r-values = 0.352, 0.395 at p = 0.019 and 0.008, respectively). Revascularization did not show any significant correlation with NGAL level (p = 0.34).
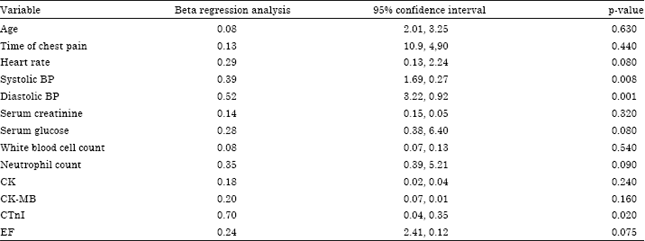
Logistic regression analysis are shown in Table 5. Heart rate, systolic, diastolic blood pressure, neutrophil count, serum glucose and cTnI levels were the significant predictors of increased NGAL level (Fig. 2) at 95% confidence interval CI is (0.13-2.24 p = 0.08) for heart rate.
| Table 4: | Correlation between NGAL levels and in-hospital complications |
 | |
| Table 5: | Logistic regression analysis for the predictors of high NGAL |
 | |
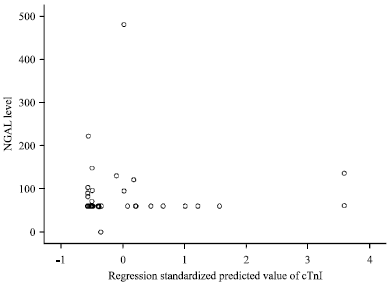 | |
| Fig. 2: | Regression analysis with significant association between NGAL and cardiac TnI |
Ninety five percent CI are (1.69-0.27 p = 0.008, 3.22-0.92 p = 0.001) for systolic and diastolic blood pressures, respectively. Ejection fraction was significant predictor of increased NGAL level 95% CI (2.41-0.12 p = 0.075).
DISCUSSION
Previously, the biomarker Neutrophil Gelatinase-Associated Lipocalin (NGAL) were established as a sensitive marker of both the clinical and subclinical acute kidney injury. However, its prognostic role in predicting adverse events in patients with STEMI treated with fibrinolytic therapy is not fully studied.
In this study, NGAL levels were significantly higher in patients with in-hospital complications. But the levels of NGAL were normal in patients with STEMI who did not develop complications. These findings suggest an active pathophysiological role for NGAL in the development of acute coronary events and its usefulness as prognostic biomarker in patients with STEMI. The NGAL increased significantly in patients with myocardial infarction as compared to patients with stable coronary artery disease and healthy subjects. Also, Kafkas et al. (2012) demonstrated that serum levels of NGAL were higher in patients with acute coronary syndrome than those with stable angina. However, the prognostic value of NGAL has not been studied in patients with myocardial infarction (Lindberg et al., 2012). Similarly, Malek (2012) reported that increased level of NGAL was detected in patients with acute myocardial infarction, heart failure or stroke. There is inadequate information about the prognostic significance of NGAL in patients after MI or HF. Also no data was found about their comparison or interaction with natriuretic peptides exists (Malek, 2012).
Some studies reported that patients with heart failure (Damman et al., 2008; Poniatowski et al., 2009), coronary artery disease (Choi et al., 2008; Zografos et al., 2009) and stroke (Elneihoum et al., 1996; Anwaar et al., 1998) had increased levels of urine, serum, or plasma NGAL. In another study, Zografos et al. (2009) found that serum NGAL levels were significantly higher in the presence of coronary artery disease and well correlated with the severity of the disease. Daniels et al. (2012) found that both the NGAL and NT-pro BNP levels were associated with cardiovascular death, all-cause mortality and the combined cardiovascular outcome independent of one another. Other investigators reported that NGAL is hyper-expressed in the myocardium following myocardial infarction (Hemdahl et al., 2006; Yndestad et al., 2009). The combination of NGAL with the MMP-9 and its ability to enhance the proteolysis activity of MMP-9 may suggest the role of NGAL as an active mediator of acute coronary syndromes and their complications (Yan et al., 2001).
Lindberg et al. (2012) in a study of 584 patients with STEMI found that patients with high NGAL had increased risk of all-cause mortality and Major Adverse Cardiovascular Events (MACE) as compared with patients having low NGAL levels. They also concluded that high plasma NGAL independently predicts all-cause mortality and MACE in ST-segment elevation myocardial infarction patients treated with primary percutaneous coronary intervention. Their findings are in agreement with the present study findings, because in this study patients with high NGAL showed more cardiovascular complications and in-hospital death than those with low NGAL level. It was also noted that high NGAL level is a strong predictor for in-hospital adverse events and mortality as well as strongly correlates with death, acute pulmonary edema, cardiogenic shock and recurrent angina parallel to this study results. Akcay et al. (2012) in a study of one hundred six consecutive patients with STEMI found that in-hospital and 1-year major adverse cardiovascular event rates were significantly higher in the high-NGAL group as compared to the low NGAL group. These data might prove the prognostic value of NGAL in patients with STEMI. It might also prove that NGAL can be a useful tool in clinical practice to stratify patients with STEMI. Also it will help to identify those who will develop in-hospital complications and adverse events which might benefit from early intervention. Therefore, It is important to recognize that the timing of biomarker measurement has important impact on the ability of NGAL to predict the cardiovascular complications in patients with STEMI.
CONCLUSION
Cardiovascular death and in-hospital complications were significantly higher in patients with high levels of NGAL than those with low levels of NGAL. Therefore, NGAL is a novel biomarker, easy and rapid to measure and might prove to be a useful tool for predicting cardiovascular complications in patients with acute myocardial infarction. It might help in the management and risk stratification in patients with STEMI. The study findings showed a potential for an expanded study with multicenter collaborations and long term follow-up with several measures of NGAL levels needed to identify the proper timing of measuring NGAL in order to improve its prognostic value in patients with STEMI.
REFERENCES
- Akcay, A.B., M.F. Ozlu, N. Sen, S. Cay and O.H. Ozturk et al., 2012. Prognostic significance of neutrophil gelatinase-associated lipocalin in ST-segment elevation myocardial infarction. J. Invset. Med., 60: 508-513.
CrossRefPubMedDirect Link - Anavekar, N.S., J.J.V. McMurray, E.J. Velazquez, S.D. Solomon and L. Kober et al., 2004. Relation between renal dysfunction and cardiovascular outcomes after myocardial infarction. N. Engl. J. Med., 351: 1285-1295.
CrossRefPubMedDirect Link - Anwaar, I., A. Gottsater, K. Ohlsson, I. Mattiasson and F. Lindgarde, 1998. Increasing levels of leukocyte-derived inflammatory mediators in plasma and cAMP in platelets during follow-up after acute cerebral ischemia. Cerebrovasc. Dis., 8: 310-317.
CrossRef - Aviles, R.J., A.T. Askari, B. Lindahl, L. Wallentin and G. Jia et al., 2002. Troponin T levels in patients with acute coronary syndromes, with or without renal dysfunction. N. Engl. J. Med., 346: 2047-2052.
CrossRef - Blankenberg, S., H.J. Rupprecht, O. Poirier, C. Bickel and M. Smieja et al., 2003. Plasma concentrations and genetic variation of matrix metalloproteinase 9 and prognosis of patients with cardiovascular disease. Circulation, 107: 1579-1585.
PubMedDirect Link - Buffon, A., L.M. Biasucci, G. Liuzzo, G. D'Onofrio, F. Crea and A. Maseri, 2002. Widespread coronary inflammation in unstable angina. N. Engl. J. Med., 347: 5-12.
CrossRef - Choi, K.M., J.S. Lee, E.J. Kim, S.H. Baik and H.S. Seo et al., 2008. Implication of lipocalin-2 and visfatin levels in patients with coronary heart disease. Eur. J. Endocrinol., 158: 203-207.
CrossRefDirect Link - Zografos, T., A. Haliassos, S. Korovesis, E. Giazitzoglou, E. Voridis and D. Katritsis, 2009. Association of neutrophil gelatinase-associated lipocalin with the severity of coronary artery disease. Am. J. Cardiol., 104: 917-920.
CrossRef - Damman, K., D.J. van Veldhuisen, G. Navis, A.A. Voors and H.L. Hillegea, 2008. Urinary Neutrophil Gelatinase Associated Lipocalin (NGAL), a marker of tubular damage, is increased in patients with chronic heart failure. Eur. J. Heart Fail., 10: 997-1000.
CrossRef - Daniels, L.B., E. Barrett-Connor, P. Clopton, G.A. Laughlin, J.H. Ix and A.S. Maisel, 2012. Plasma neutrophil gelatinase-associated lipocalin is independently associated with cardiovascular disease and mortality in community-dwelling older adults: The rancho bernardo study. J. Am. Coll. Cardiol., 59: 1101-1109.
CrossRef - Elneihoum, A.M., P. Falke, L. Axelsson, E. Lundberg, F. Lindgarde and K. Ohlsson, 1996. Leukocyte activation detected by increased plasma levels of inflammatory mediators in patients with ischemic cerebrovascular diseases. Stroke, 27: 1734-1738.
Direct Link - Galis, Z.S., G.K. Sukhova, M.W. Lark and P. Libby, 1994. Increased expression of matrix metalloproteinases and matrix degrading activity in vulnerable regions of human atherosclerotic plaques. J. Clin. Invest., 94: 2493-2503.
CrossRef - Goldmann, B.U., V. Rudolph, T.K. Rudolph, A.K. Holle, M. Hillebrandt, T. Meinertz and S. Baldus, 2009. Neutrophil activation precedes myocardial injury in patients with acute myocardial infarction. Free Radical Biol. Med., 47: 79-83.
CrossRef - Malek, F., 2012. The importance of NGAL and cystatin C biomarkers in cardiovascular diseases-editorial. Vnitr Lek., 58: 261-262 [In Czech].
PubMedDirect Link - Hemdahl, A.L., A. Gabrielsen, C. Zhu, P. Eriksson and U. Hedin et al., 2006. Expression of neutrophil gelatinase-associated lipocalin in atherosclerosis and myocardial infarction. Arterioscler. Thromb. Vascular Biol., 26: 136-142.
CrossRef - Jaremo, P., G. Hansson and O. Nilsson, 2000. Elevated inflammatory parameters are associated with lower platelet density in acute myocardial infarctions with ST-elevation. Thrombosis Res., 100: 471-478.
Direct Link - Kafkas, N., C. Demponeras, F. Zoubouloglou, L. Spanou, D. Babalis and K. Makris, 2012. Serum levels of gelatinase associated lipocalin as indicator of the inflammatory status in coronary artery disease. Int. J. Inflammation, Vol. 2012.
CrossRef - Kai, H., H. Ikeda, H. Yasukawa, M. Kai and Y. Seki et al., 1998. Peripheral blood levels of matrix metalloproteases-2 and -9 are elevated in patients with acute coronary syndromes. J. Am. Coll. Cardiol., 32: 368-372.
Direct Link - Khan, S.Q., P. Quinn, J.E. Davies and L.L. Ng, 2008. N-terminal pro-B-type natriuretic peptide is better than TIMI risk score at predicting death after acute myocardial infarction. Heart, 94: 40-43.
CrossRef - Kosiborod, M., S.S. Rathore, S.E. Inzucchi, F.A. Masoudi, Y. Wang, E.P. Havranek and H.M. Krumholz, 2005. Admission glucose and mortality in elderly patients hospitalized with acute myocardial infarction: Implications for patients with and without recognized diabetes. Circulation, 111: 3078-3086.
CrossRef - Lindberg, S., S.H. Pedersen, R. Mogelvang, J.S. Jensen, A. Flyvbjerg, S. Galatius and N.E. Magnusson, 2012. Prognostic utility of neutrophil gelatinase-associated lipocalin in predicting mortality and cardiovascular events in patients with ST-segment elevation myocardial infarction treated with primary percutaneous coronary intervention. J. Am. Coll. Cardiol., 60: 339-345.
CrossRefPubMed - Madjid, M., I. Awan, J.T. Willerson and S.W. Casscells, 2004. Leukocyte count andcoronary heart disease: Implications for risk assessment. J. Am. Coll. Cardiol., 44: 1945-1956.
CrossRefPubMedDirect Link - Naruko, T., M. Ueda, K. Haze, A.C. van der Wal and C.M. van der Loos et al., 2002. Neutrophil infiltration of culprit lesions in acute coronary syndromes. Circulation, 106: 2894-2900.
CrossRefPubMedDirect Link - Sahinarslan, A., S.A. Kocaman, D. Bas, A. Akyel, U. Ercin, O. Zengin and T. Timurkaynak, 2011. Plasma neutrophil gelatinase-associated lipocalin levels in acute myocardial infarction and stable coronary artery disease. Coronary Artery Dis., 22: 333-338.
PubMed - Sarndahl, E., I. Bergstrom, V.P. Brodin, J. Nijm, H.L. Setterud and L. Jonasson, 2007. Neutrophil activation status in stable coronary artery disease. PLoS ONE, Vol. 2, No. 10.
CrossRefDirect Link - Yan, L., N. Borregaard, L. Kjeldsen and M.A. Moses, 2001. The high molecular weight urinary matrix metalloproteinase (MMP) activity is a complex of gelatinase B/MMP-9 and neutrophil gelatinase-associated lipocalin (NGAL): modulation of MMP-9 activity by ngal. J. Biol. Chem., 276: 37258-37265.
CrossRef - Yndestad, A., L. Landro, T. Ueland, C.P. Dahl and T.H. Flo et al., 2009. Increased systemic and myocardial expression of neutrophil gelatinase-associated lipocalin in clinical and experimental heart failure. Eur. Heart J., 30: 1229-1236.
CrossRefDirect Link








