Research Article
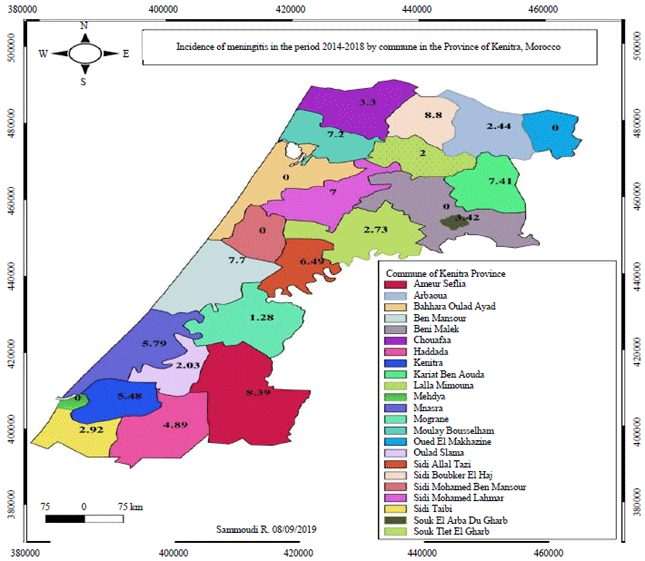
Epidemiological, Cytochemical and Bacteriological Profile of Meningitis among Adults and Children in North West of Morocco
Department of Health Facilities Networks Provincial Epidemiology Unit, Kenitra Health Delegation, Morocco
Mohamed EL Hioui
Unit for Clinic and Cognitive Neuroscience and Health, Laboratory of Biology and Health, Department of Biology, Faculty of Sciences, Ibn Tofail University, Kenitra, Morocco
LiveDNA: 212.3151
Samira Jayche
Unit for Clinic and Cognitive Neuroscience and Health, Laboratory of Biology and Health, Department of Biology, Faculty of Sciences, Ibn Tofail University, Kenitra, Morocco
Lacheheb Mohammed
Department of Health Facilities Networks Provincial Epidemiology Unit, Kenitra Health Delegation, Morocco
Alaoui Asmaa
Department of Health Facilities Networks Provincial Epidemiology Unit, Kenitra Health Delegation, Morocco
Abdesslam Lhou
Department of Health Facilities Networks Provincial Epidemiology Unit, Kenitra Health Delegation, Morocco
Badreddine dahou
Department of Health Facilities Networks Provincial Epidemiology Unit, Kenitra Health Delegation, Morocco
Ahmed Omar Touhami Ahami
Unit for Clinic and Cognitive Neuroscience and Health, Laboratory of Biology and Health, Department of Biology, Faculty of Sciences, Ibn Tofail University, Kenitra, Morocco
LiveDNA: 212.28621