Research Article
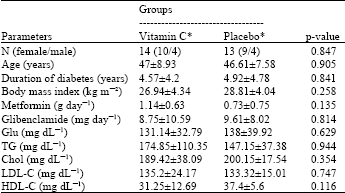
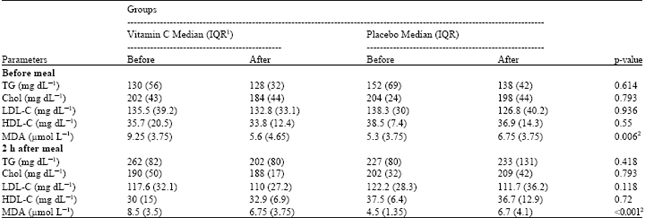
Effect of Vitamin C Supplementation on Postprandial Oxidative Stress and Lipid Profile in Type 2 Diabetic Patients
Department of Nutrition, School of Health and Nutrition, Shiraz University of Medical Sciences, Shiraz, Iran
Najmeh Hejazi
Department of Nutrition, School of Health and Nutrition, Shiraz University of Medical Sciences, Shiraz, Iran
Mohammad-Hossein Dabbaghmanesh
Department of Edocrine and Metabolism Research Center, Shiraz University of Medical Sciences, Shiraz, Iran
Hamid-Reza Tabatabaei
Department of Epidemiology, School of Health and Nutrition, Shiraz University of Medical Sciences, Shiraz, Iran
Afsane Ahmadi
Department of Nutrition, School of Health and Nutrition, Shiraz University of Medical Sciences, Shiraz, Iran
Hasti Ansar
Department of Nutrition, School of Health and Nutrition, Shiraz University of Medical Sciences, Shiraz, Iran