Research Article
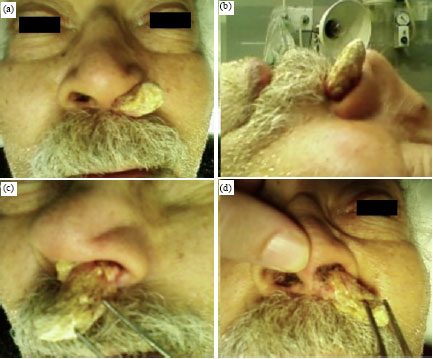
Nasal Vestibular Huge Keratoacanthoma: An Unusual Site
Otorhinolaryngology Research Centre, Department of Otolaryngology, Head and Neck Surgery, Tehran University of Medical Sciences, Amir-A’lam Hospital, Tehran, Iran
M. Khorsandi-Ashtiani
Otorhinolaryngology Research Centre, Department of Otolaryngology, Head and Neck Surgery, Tehran University of Medical Sciences, Amir-A’lam Hospital, Tehran, Iran
M. Rabbani-Anari
Otorhinolaryngology Research Centre, Department of Otolaryngology, Head and Neck Surgery, Tehran University of Medical Sciences, Amir-A’lam Hospital, Tehran, Iran
A. Bassam
Otorhinolaryngology Research Centre, Department of Otolaryngology, Head and Neck Surgery, Tehran University of Medical Sciences, Amir-A’lam Hospital, Tehran, Iran
A. Kouhi
Otorhinolaryngology Research Centre, Department of Otolaryngology, Head and Neck Surgery, Tehran University of Medical Sciences, Amir-A’lam Hospital, Tehran, Iran