Research Article
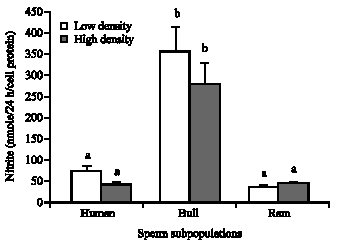
In vitro Production of Nitrite by Low and High Density Sperm Subpopulations of Human, Bull and Ram
Department of Basic Sciences, College of Veterinary Medicine, Islamic Azad University, Karaj Branch, Karaj, Iran
Hossein Hassanpour
Department of Basic Sciences, College of Veterinary Medicine, Sharekord University, Sharekord, Iran