Research Article
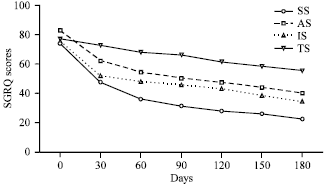
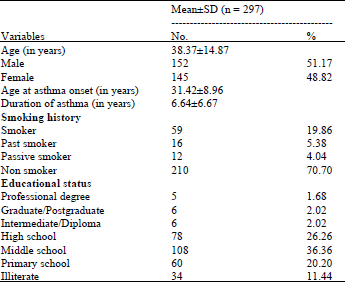
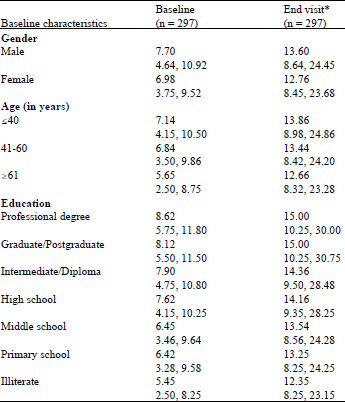
Impact of Pharmacist Provided Patient Education on Knowledge, Attitude, Practice and Quality of Life in Asthma Patients in a South Indian Hospital
Department of Pharmacy Practice, SRM College of Pharmacy,
A. D. Nageswari
Department of Pulmonary Medicine, SRM Medical College, Hospital and Research Centre,
K. Ilango
Interdisciplinary School of Indian System of Medicine (ISISM), SRM University, Kattankulathur, 603 203, Kanchipuram (DT), Tamil Nadu, India