Research Article
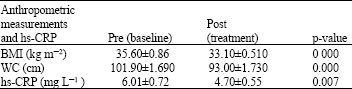
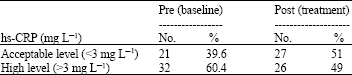
The Effect of Weight Reduction Diet on C-Reactive Protein Level in Obese-Adult Subjects
Deparment of Community Health Sciences, College of Applied Medical Sciences, King Saud University, Riyadh, Saudi Arabia
Rabba H. Al-Huthail
Deparment of Community Health Sciences, College of Applied Medical Sciences, King Saud University, Riyadh, Saudi Arabia
Mohamed A. Alsaif
Deparment of Community Health Sciences, College of Applied Medical Sciences, King Saud University, Riyadh, Saudi Arabia
Abdulaziz M. Al-Othman
Deparment of Community Health Sciences, College of Applied Medical Sciences, King Saud University, Riyadh, Saudi Arabia
May N. Al-Muammer
Deparment of Community Health Sciences, College of Applied Medical Sciences, King Saud University, Riyadh, Saudi Arabia
Saada M. Al-Orf
Deparment of Community Health Sciences, College of Applied Medical Sciences, King Saud University, Riyadh, Saudi Arabia
Abdallah A. Saeed
Deparment of Community Health Sciences, College of Applied Medical Sciences, King Saud University, Riyadh, Saudi Arabia
Badreldin A. Mohamed
Deparment of Community Health Sciences, College of Applied Medical Sciences, King Saud University, Riyadh, Saudi Arabia