Research Article
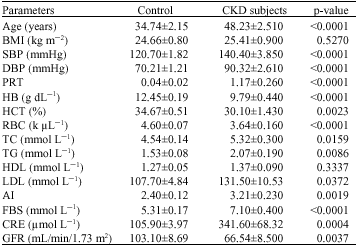
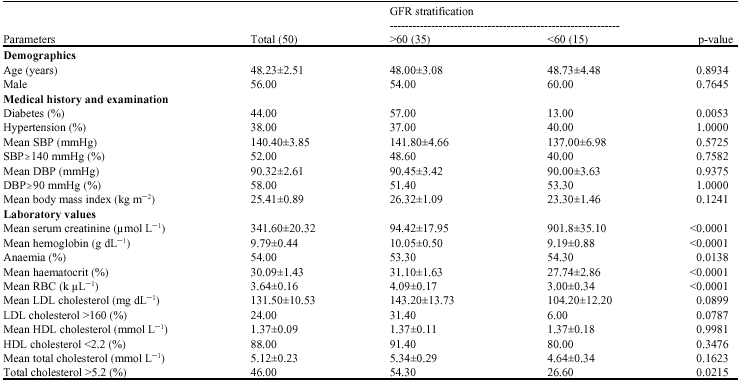
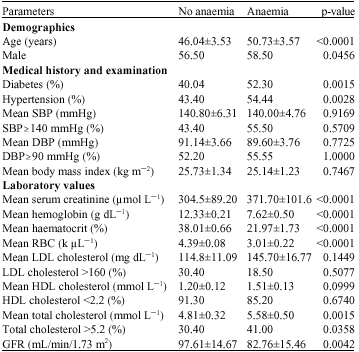
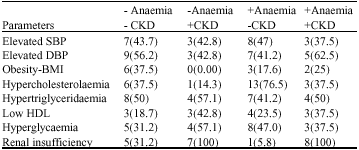
Anaemia as a Risk Factor for Cardiovascular Disease in Patients with Chronic Kidney Disease
Department of Molecular Medicine,Kwame Nkrumah University of Science and Technology, Kumasi, Ghana
William K.B.A. Owiredu
Department of Molecular Medicine,Kwame Nkrumah University of Science and Technology, Kumasi, Ghana
Edwin F. Laing
Department of Molecular Medicine, Kwame Nkrumah University of Science and Technology, Kumasi, Ghana
Nafiu Amidu
Department of Molecular Medicine,Kwame Nkrumah University of Science and Technology, Kumasi, Ghana
Benjamin A. Eghan Jnr.
Department of Medicine, School of Medical Sciences, College of Health Sciences, Kwame Nkrumah University of Science and Technology, Kumasi, Ghana
Linda Ahenkorah
Department of Molecular Medicine,Kwame Nkrumah University of Science and Technology, Kumasi, Ghana