ABSTRACT
Ever since the 1970s, the behavior of health care providers has been a research topic of serious concern to medical and economic scholars in the advanced countries. Because of the increased supply and demand for medical care, related expenditure has risen so rapidly that it has exceeded the economic growth rate and has increased to such an extent that it has affected the opportunities for the balanced development of other sectors. For this reason, in the medical market, how to make good use of limited medical resources, in order to seek the largest health standard for all of the country’s citizens, is currently one of the most important research directions in medical economics. In terms of the supply of medical care in the market, hospitals are in the most important position and also account for the most expenditure, that is, hospitals use the most medical resources in the medical market. According to Bureau of National Health Insurance statistics, hospitals have since 1995 when national health insurance began to be implemented on average accounted for 65% of total reported medical expenses. If such expenses are categorized according to the level of evaluation, medical expenses reported by medical centers and regional hospitals account for 70% of total reported expenditure in the hospital sector and physicians mostly control some 80% of this medical expenditure. For this reason, physicians have a major influence on medical expenditure in terms of how efficiently medical resources are used. Moreover, when seeking to measure the concept of relative efficiency in regard to medical care, most studies focus on an evaluation of the relative efficiency of hospitals. It is for this reason that this study intends to focus on the physicians and to examine the input-output relationships between the medical resources used by these physicians and the quantity of medical services provided by them, in order to analyze the productivity and efficiency of physicians. In addition, by applying the Malmquist productivity index, this study empirically evaluates how the quantities of each physician′s medical inputs and service outputs affect productivity and efficiency and uses panel data to analyze the sources of each physician’s productivity and efficiency changes over the years.
PDF Abstract XML References
How to cite this article
DOI: 10.3923/jms.2006.577.584
URL: https://scialert.net/abstract/?doi=jms.2006.577.584
INTRODUCTION
The implementation of national health insurance has had a huge influence on Taiwan’s overall health care environment. As for the general public, national health insurance has removed many of the economic obstacles that people face and has increased their access to medical services. In particular, for those who in the past were unable to be covered by health insurance as well as those with serious diseases and injuries, it is good news indeed. In regard to hospitals, the implementation of the health insurance system, which has resulted in a redistribution of medical resources, has had both positive and negative impacts on the hospitals’ operations. The positive impacts are that, in response to the implementation of national health insurance, the hospitals have, in order to survive, not only improved their quality, efficiency and the types of service and range of services offered, but have also once again examined their respective organizations’ internal operations as well as the relationships within each organization. The negative impacts are that, if the hospitals have been unable to respond to the changes in an effective manner, then their very existence has been threatened. Currently, the numbers of large hospitals and local clinics have significantly increased, while regional hospitals are facing a significant reduction in patient visits and are encountering operational difficulties.
Although the growth rate of total medical costs declined from 15 to 7.38% following the launching of the national health insurance program in Taiwan, the growth rate of outpatients reached 9.14% and the growth rate of inpatients amounted to 3.88%, with the national average of outpatient visits per person per year exceeding 14 visits. While the public’s habitually seeking medical advice has of course resulted in a huge waste of medical resources, the differences in the behavior of physicians in terms of providing treatment has also significantly affected the extent to which medical resources are used up. In providing care in relation to the same diseases, different ways of providing treatment will give rise to different levels of cost effectiveness.
Nunamaker (1983) first of all used Data Envelopment Analysis (DEA) to estimate the productivity of medical institutions. However, in the past, most related studies in the medical field focused on the hospital and very few focused on the physicians themselves. For instance, Chilingerian and Sherman (1990) and Chilingerian (1992) used panel data to examine changes in long-term productivity and efficiency for hospitals and clinics beginning with the late 1980s (Fare et al., 1989). If consideration is also given to analyzing the quality of medical care, this was only incorporated in studies from the mid-1990s onwards (Fare et al., 1995). For this reason, in this study we use the output-oriented Malmquist productivity index approach (Malmquist, 1953) to analyze changes in productivity and efficiency for physicians in both public and private medical centers and hospitals in Taiwan. In the process we arrive at the following four research objectives: (1) To use hospital input-output data to calculate the value of the output distance function and to construct Malmquist productivity indices for each hospital to facilitate comparisons between periods and to decompose these indices into their change components. (2) To consider including an indicator of medical quality among the physician’s output variables and to objectively evaluate its effect in terms of analyzing the Malmquist productivity indices for each physician and their change components. (3) To engage in sensitivity analysis, because the estimation of the Malmquist index is performed by means of a distance function, which in turn is established in the DEA analytical model. (Because the sensitivity of the DEA approach to different combinations of inputs and outputs is relatively high, we use many combinations of inputs and outputs to evaluate the sensitivity of the Malmquist index.) (4) To use both the Tobit and OLS regression analysis approach to discuss the factors affecting the changes in the efficiency and productivity change of physicians.
MATERIALS AND METHODS
The approaches used to evaluate efficiency have by and large been categorized according to two main kinds, namely, the non-frontier approach and the frontier approach. The former pays attention to the statistical method used and is based on the average concept of efficiency value without taking into consideration the economic meaning of efficiency, while the latter bases its efficiency on the concept of Pareto optimality and incorporates the frontier concept, so that, relatively speaking, it conforms more closely to the economic meaning of efficiency. The non-frontier approach has many applications in the realm of financial management and the steps involved in its use include first using factor analysis or principal component analysis to select some financial ratios that will serve as the research variables and then using these variables to construct a statistical model to perform the analysis. The statistical models generally used include the discriminate analytical model, the PROBIT model and the LOGIT models, which are mainly used in the selection process and which have statistical meaning. Moreover, when performing the statistical analysis, it is necessary to develop numerous hypotheses before proceeding, an approach that does not conform to the original meaning of efficiency as defined by Farrell. For this reason, in this study we adopt the frontier approach with its economic connotations to perform the analysis.
From an empirical point of view, there are two different kinds of approaches to evaluating efficiency using the frontier approach, these being the parametric approach and the nonparametric approach. In contrast to the parametric approach, the nonparametric approach does not set the functional form of the production frontier a priori and thus is not limited by the functional expression. Therefore, there is no need to have the many hypothetical conditions that arise due to the statistical approach adopted when estimating the function and measuring efficiency. Moreover, when dealing with the problems of having many inputs and outputs, the nonparametric approach is easier to use than the parametric approach and so in this study we adopt the nonparametric approach in our empirical analysis. Moreover, the approach used to measure the physician’s productivity change is the Malmquist productivity index that is currently commonly used in the management field. In summing up the above, this study will use DEA, Malmquist productivity index, Tobit and OLS regression analysis approach to measure the productivity of physicians and evaluate the factors that affect the changes in the efficiency and productivity change of physicians.
RESULTS AND DISCUSSION
This study uses the Current Statistics of Publicly- and Privately-Established Medical Institutions, the Statistics on the Quantity of Hospital Medical Services and the National Health Insurance Academic Research Database compiled by the Department of Health of the Executive Yuan in Taiwan to select the medical centers physicians and regional hospitals, physicians that serve as the sample used in our analysis of productivity change from 1999 to 2004. In considering the sensitivity of the Malmquist productivity index to the setting of the input and output variables, the input and output variables are set into the following three combinations to perform the sensitivity analysis in this study. In selecting the input and output variables, we mostly refer to Chilingerian (1992) In his study, Chilingerian (1992) examines the productivity of physicians within different departments in the same hospital, while this study is concerned with measuring the productivity of physicians in different medical institutions.
Model 1
Input variables: Diagnostic fee, medicine fee, length of prescription and length of hospital stay.
Output variables: Outpatient visits, emergency visits, number of patients discharged, average number of medical staff per bed.
Model 2
Input variables: Diagnostic fee, medicine fee, length of prescription and length of hospital stay.
Output variables: Outpatient visits, emergency visits, number of patients discharged.
Model 3
Input variables: Diagnostic fee, medicine fee, length of prescription and length of hospital stay.
Output variables: Outpatient visits, emergency visits, number of patients discharged, number of surgeries.
For each of these three combinations of inputs and outputs, all of the input variables remain unchanged. In terms of the output variables, the average number of medical staff per bed in Model 1 serves as the proxy variable for measuring output in regard to medical quality. This variable is left out of Model 2. This medical quality variable is also taken out of Model 3 and replaced with the number of surgeries. For the empirical analysis, the DEAP software is used to calculate the Malmquist productivity index and the STATISTICA software package is employed to generate the descriptive statistics for the indices and perform the regression analysis for the influential factors.
Table 1 to 3, respectively list the three different combinations of inputs and outputs for each of the types of long-term productivity and efficiency change indices over the full length of the sample period. According to the results derived for the Model 1 combination shown in Table 1, with regard to the productivity and efficiency indices, of the 40 hospitals’ physicians’ physicians, only two of them are found to exhibit long-term productivity growth, while the long-term productivity of the other 38 are seen to exhibit a decline. When the productivity change index is decomposed into efficiency and technical change indices, it is discovered that the type of technical change is similar to the type of productivity change, but that, among the 40 hospitals’ physicians, 10 exhibit an improvement in efficiency, 7 do not change and 23 exhibit a deterioration in efficiency. For this reason, although in the vast majority of cases the productivity of the hospitals’ physicians’ physicians is not enhanced, in close to half of the hospitals’ physicians’ physicians there is an improvement in efficiency or at least no sign of deterioration.
| Table 1: | Long-term change indices (Model 1) |
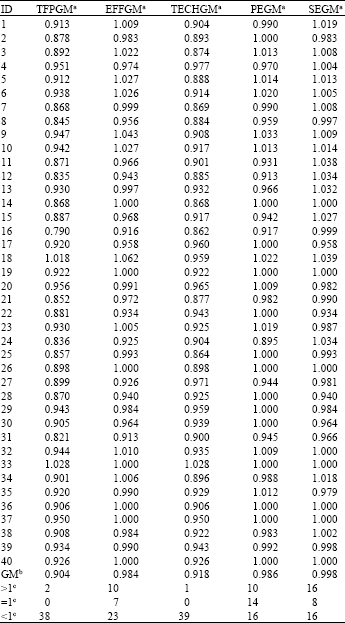 | |
| Notes: a and b represent geometric means. c represents increase, no change, or decrease, separately | |
If each hospital’s physicians efficiency change index is then decomposed into pure efficiency change and scale efficiency change indices, it is discovered that, among the 40 hospitals’ physicians’ physicians in the sample, in about 60% of the cases, the pure efficiency and scale efficiency change exhibit either an increasing trend or else remain constant.
Secondly, when the results for the Model 2 combination of variables shown in Table 2 are compared with the results in Table 1, if medical quality is not taken into consideration, then neither the productivity change index nor the technical change index vary significantly and the values for scale efficiency change are also extremely close. However, the efficiency and pure efficiency change indices improve significantly, which means that, when medical quality is taken into consideration, in terms of the evaluation of productivity change, there is no significant improvement.
| Table 2: | Long-term change indices (Model 2) |
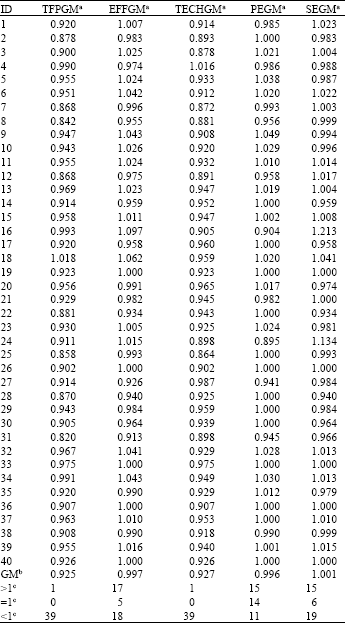 | |
| Notes: a and b represent geometric means. c represents increase, no change, or decrease, separately | |
When medical quality is included, however, there is a decline in efficiency. Furthermore, when the combination of variables in Table 3 is compared and the number of surgeries is included among the output variables, both productivity and technical change exhibit slight growth, while efficiency and the pure efficiency and scale efficiency change resulting from its decomposition each decline slightly.
Table 4 and 5 take the long-term productivity and efficiency change indices in Table 1 to 3 and based on the public and private ownership of the hospitals’ physicians’ physicians, respectively list the change indices and the change frequencies of the descriptive statistics.
| Table 3: | Long-term change indices (Model 3) |
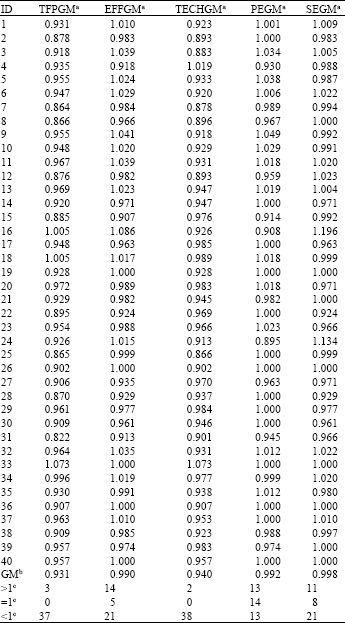 | |
| Notes: a and b represent geometric means. c represents increase, no change, or decrease, separately | |
As for the average values of the change indices in Table 4, when the medical quality in Model 1 is included, productivity change indices for public and private hospitals’ physicians’ physicians of 0.900 and 0.909, respectively, are obtained from the analysis, together with efficiency change indices of 0.993 are 0.979 and technical change indices of 0.906 and 0.929, respectively. When Model 2, which does not take medical quality into consideration, is combined with Model 3, the productivity, efficiency and technical change indices described above are, in terms of their average values, all significantly larger than the results obtained from combining Model 1, which does take medical quality into consideration, with Model 3. As for the long-term productivity and efficiency change frequencies in Table 5, their overall change in accordance with the various combinations of inputs and outputs is as described above and for this reason we do not further explain these results here.
Table 6 lists the factors that influence efficiency within a single period. Under the assumption of constant returns to scale, the efficiency of public hospitals’ physicians’ physicians and of hospitals’ physicians’ physicians with relatively high lengths of stay tends to be rather poor, while the efficiency of hospitals’ physicians’ physicians’ physicians with a high utilization rate of beds and high market concentration is relatively good. If medical quality is not included, then the more beds there are, the more efficient the hospital is, although the rate at which the efficiency increases progressively declines. However, if medical quality is included, then efficiency will progressively decline as the scale of operations in terms of the number of beds increases. Under the assumption of variable returns to scale, the influence that public hospitals’ physicians, the utilization rate of beds, the average length of stay in hospital and the degree of market concentration have on efficiency is found to be exactly the same as under the assumption of constant returns to scale discussed above. Only if the number of beds increases does the hospital become less efficient, although the decline in efficiency becomes progressively less pronounced as the number of beds increases. This finding is similar to the results for the number of hospital beds in Model 1 where medical quality is included under the assumption of constant returns to scale. In terms of the proxy variable for time, under constant returns to scale, the second year is more efficient than the first, but the sixth year appears to be relatively inefficient. A similar finding is also obtained using Model 1 based on the variable returns to scale assumption. From the results of Table 6, it can be seen that the efficiency of public hospitals’ physicians is significantly lower than that of private hospitals’ physicians, showing that hospital ownership is still the most important factor in deciding how medical resources are to be efficiently used. Secondly, hospitals’ physicians in which the utilization rate of beds is higher and in which the average length of stay is shorter tend to be more efficient. However, hospitals’ physicians in which the number of beds is higher are not easy to manage, which results in the hospitals’ physicians becoming less efficient. Nevertheless, the extent of the reduction in efficiency becomes smaller as the number of beds increases. Only the degree of market concentration has a positive influence on the hospital’s efficiency. This finding shows that it is inappropriate for the view that competition theory enhances efficiency to be applied to the medical market in Taiwan.
| Table 4: | Summary of long-term change indices |
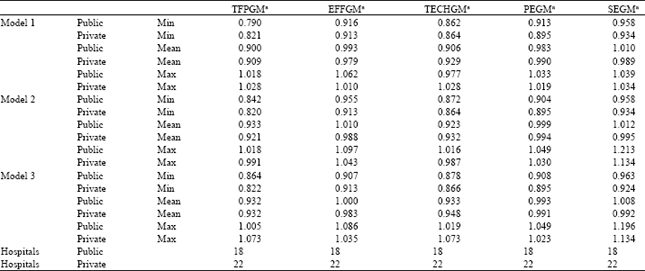 | |
| Note: a represents geometric mean | |
| Table 5: | Summary of long-term change frequencies |
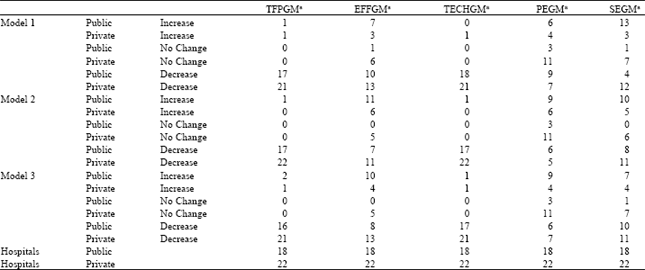 | |
| Note: a represents geometric mean | |
Table 7 lists the factors that influence productivity and efficiency change across time periods. With regard to productivity change, the utilization rate of beds is the important factor that determines productivity growth. When medical quality is included, the higher the degree of market concentration, then the more significant is the productivity growth. The productivity growth in the second and fifth periods is slower when compared with the first period. As for efficiency change, in the case of hospitals’ physicians with a high utilization rate of beds and shorter average lengths of stay, efficiency growth is more significant. The number of beds has a positive influence on the growth of efficiency, but the increase in efficiency progressively declines the more beds that there are. The growth of efficiency from the second period to the fifth period takes place more slowly than in the first period. Overall, the results of Table 7 indicate that public hospitals’ physicians have a positive but insignificant influence in terms of the growth of productivity and efficiency. The utilization rate of beds and the average length of stay in hospital are still the important factors determining productivity and efficiency change. The number of hospital beds and the degree of market concentration have a positive, but a not very significant, effect on the productivity and efficiency growth of the hospitals’ physicians. When compared with the first period, the second to the fifth periods each exhibit a declining tendency in terms of their influence on productivity and efficiency.
| Table 6: | Factors influencing productivity and efficiency change within periods |
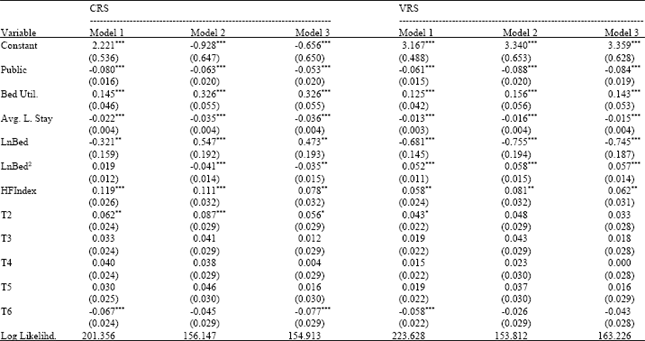 | |
| Notes: Standard errors in parentheses. ***, **, * represents 1, 5 and 10% level of significance, respectively | |
| Table 7: | Factors influencing productivity and efficiency change across periods |
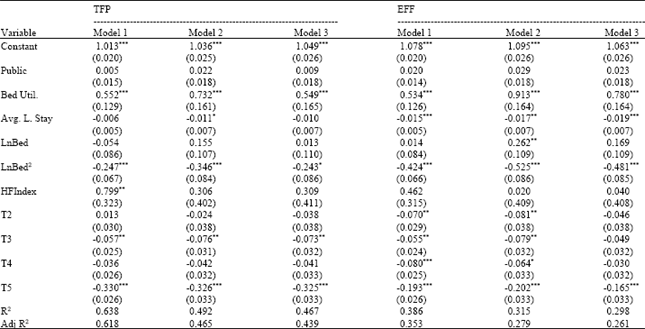 | |
| Notes: Standard errors in parentheses. ***, **, * represents 1, 5 and 10% level of significance, respectively | |
The coefficients of determination in Table 7 each have fairly good explanatory power in terms of productivity and efficiency changes. However, when compared with the results of Table 6, the extent of the influence of all of the explanatory variables in Table 7 is not as significant as in Table 6 in terms of the explanatory variables within a single time period.
CONCLUSIONS AND RECOMMENDATIONS
This study attempts to apply the Malmquist productivity index analytical approach to panel data that comprise the medical inputs and service volume outputs of Taiwan’s medical centers’ physicians and regional hospitals’ physicians. The purpose behind this is to examine the long-term productivity and efficiency changen in relation to physicians, evaluate the factors that influence productivity and efficiency change and consider whether or not medical quality should be included in order to analyze its effect on productivity and efficiency change. In terms of the research method adopted, the Malmquist productivity index approach involves solving a multi-input and multi-output distance function linear programming problem, in order to evaluate the trend in productivity change for each policy unit across different time periods. A mathematical model can also be used to decompose productivity change into the product of efficiency change and technical change, the former also being the product of pure efficiency change and scale efficiency change. Furthermore, in evaluating the productivity and efficiency of physicians, the literature (Fare et al., 1989) refers to the importance of including medical quality. Three kinds of indicators are commonly referred to in the literature for measuring medical quality (Lu and Hsie, 2000), namely, the structural or medical care input, the process of providing medical services and the results or effects of medical treatment. After taking into consideration the Department of Health data used in this study and excluding with incomplete data from the sample, it is discovered that only the number of doctors and nurses per bed measured by the structural or medical care inputs can serve as the proxy variable for medical quality among the output variables. It is thus predicted that the more medical personnel there are per bed, the more medical care the patients will receive and this will therefore increase the quality of the health care provided. Furthermore, whether or not medical quality is included, as well as whether or not more or less service-related output variables are taken into consideration is likely to affect the empirical results derived in this study in relation to productivity and efficiency change and so this study uses three groups of output variables to adjust the combination of inputs and outputs for performing the empirical evaluation and making comparisons. Because the emphasis in this study is on evaluating long-term productivity and efficiency change, when examining the factors that influence productivity and efficiency change, a panel data analysis model that includes a time proxy variable is constructed, in order to better understand the long-term development trends in productivity and efficiency change.
In terms of further research that could be conducted in the future, if outpatients and inpatients can be combined, it will be easier to find which levels within the hospital or which specialist personnel are not efficient. If we can go further to analyze the productivity of the output variables including education and research, any such research will contribute even more. If the input and output variables can be more accurately selected, the results of the study will be more reliable. Furthermore, if the content and scope of the study can be enlarged, the differences in terms of the variables used can be more fully understood.
ACKNOWLEDGEMENT
The author would like to thank the Department of Health of the Republic of China, Taiwan for financially supporting this research.








