Research Article
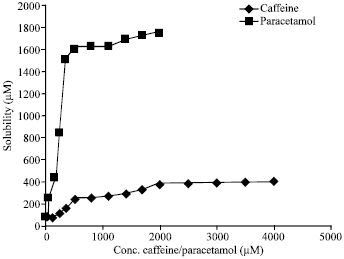
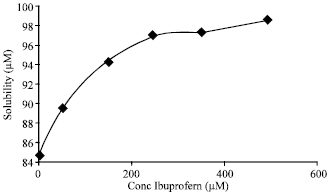
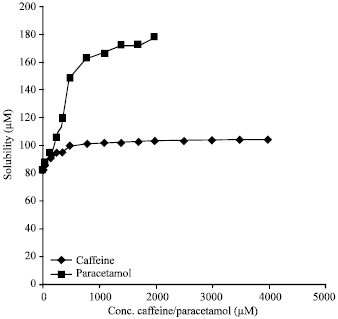
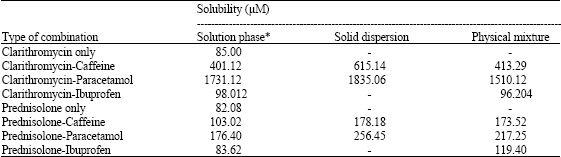
Solubility and Stability Enhancement of Poorly-Soluble Drugs Clarithromycin and Prednisolone by Combination with Other Drugs
Department of Chemistry, Panjab University, Cbandigarh-160014, India
Purshotam Sharma
Department of Chemistry, Panjab University, Cbandigarh-160014, India