ABSTRACT
South East Asia Region (SEAR) is one of the most populous world regions and also bears a disproportionate burden of mortality compared to other world regions. The purpose of this article was to analyze the situation of maternal, neonatal and perinatal health in SEAR to inform public health practitioners, program managers and policy makers about the situation in this world region. A secondary review of policy and programmatic documents published by ministries of health in SEAR countries, WHO, other UN agencies and peer reviewed journal articles in the area of maternal, child, neonatal and perinatal health published in the last five years was conducted. This article discusses the current situation of maternal, perinatal and neonatal health in SEAR countries, highlights some of the key challenges and provides recommendations to countries on the way forward for improving perinatal and maternal health. Key issues are discussed under the broad themes of improving maternal and perinatal health information systems, improving quality of care and human resource management. The article concludes that Health Systems Strengthening, Scaling up of Skilled Human Resource, Investing in information systems and improving the quality of maternal and neonatal care services are essential for future progress in countries but these are long term processes which need sustained commitment and ownership at all levels.
PDF Abstract XML References Citation
How to cite this article
DOI: 10.3923/aje.2012.1.14
URL: https://scialert.net/abstract/?doi=aje.2012.1.14
INTRODUCTION
There has been considerable attention on the high burden of maternal, perinatal and neonatal deaths in recent times. Important high-level global commitments, such as Millennium Development Goal 4 and 5 call for reduction in under-five mortality rate and improvement of maternal health respectively between 1990 and 2015 (Campbell and Graham, 2006). The WHO South-East Asia Region (SEAR) comprises of 11 Member countries and 1.7 billion inhabitants and accounts for one-fourth of the world’s population. According to the latest estimates by WHO, an estimated 38.5 million live births, 2.4 million perinatal deaths and 1.3 million stillbirths occur in the Region annually (WHO, 2007a). Five countries namely India, Bangladesh, Indonesia, Nepal and Myanmar contribute to almost 98% of the maternal deaths in the Region (WHO, 2004).
The purpose of this paper is to inform public health practitioners, program managers and policy makers about the situation and challenges of maternal, neonatal and perinatal mortality in SEAR. It also provides policy and programmatic recommendations to countries in order to further intensify concerted efforts to tackle the burden of maternal, neonatal and perinatal deaths. The source of data are mostly drawn from WHO (2004) and WHS (2009). Programmatic and policy documents published by ministries of health in SEAR countries, WHO, other UN agencies and peer reviewed journal articles in the area of maternal, child, neonatal and perinatal health published in the last five years were also reviewed.
Definitions
| • | Maternal deaths are referred to deaths of women while pregnant or within 42 days of the termination of pregnancy. These can be due to direct or indirect causes. It is measured by Maternal Mortality Ratio (MMR): number of maternal deaths per 100, 000 live births. |
| • | Neonatal mortality rate represents deaths occurring within the first four weeks after birth per 1000 live births. Based on the timings of death, neonatal deaths are further sub-classified into early and late neonatal deaths. Early deaths refer to deaths in the first week and late deaths refer to deaths after the first week (WHO, 1993). |
| • | “A stillbirth refers to a dead born fetus which can either occur before the onset of labor (ante-partum death) or during labor (intra-partum death) and is expressed per 1000 of total births” (WHO, 2004) |
| • | Perinatal mortality includes deaths after 22 weeks of gestation up to deaths within the first week of life expressed per 1000 of total births (WHO, 1993). Therefore, it includes ante-partum and intra-partum stillbirths. |
| • | A Skilled Birth attendant is an accredited health professional who has been trained to proficiency in managing normal pregnancies, providing essential neonatal and postnatal care and who can identify, manage and refer complicated pregnancies (WHO, ICM and FIGO, 2004). |
MATERNAL, NEONATAL MORTALITY AND STILLBIRTH IN SEAR
Maternal mortality: South east Asian countries show great diversity in terms of key maternal and neonatal health indicators. India, Bangladesh, Indonesia, Nepal and Myanmar contribute to almost 98% of the maternal deaths in the Region (Fig. 1).Timor-Leste and Myanmar also have high rates of maternal deaths with MMR of 380 per 100000 live births. Thailand (110) and Sri Lanka (58) and more recently, Maldives (120), have made impressive declines in maternal mortality ratios over the years and are the better performing countries of the region.
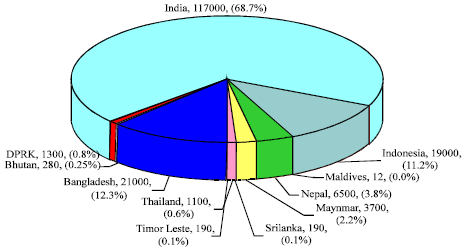 | |
| Fig. 1: | Burden of maternal mortality in SEAR (WHO, UNICEF, UNFPA and The World Bank 2007) |
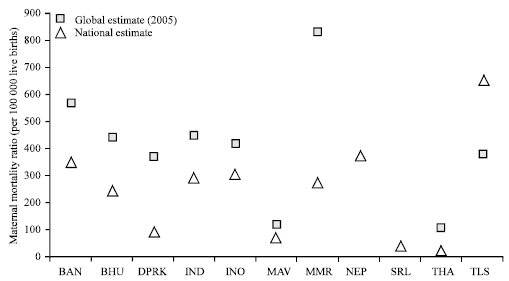 | |
| Fig. 2: | Global and national estimates comparing maternal mortality ratio per 100 000 live births in SEAR countries. BAN: Bangladesh, BHU: Bhutan, DPRK: Democratic, THA: Thailand, TLS: Timor Leste, IND: India, INO: Indonesia, MAV: Maldives, MMR: Mayanmar, NEP: Nepal, SRL: Srilanka |
Causes of maternal mortality: Maternal deaths are due to direct and indirect causes with up to 80% of maternal deaths globally occurring due to direct obstetric complications, such as haemorrhage, infection, eclampsia, obstructed labour and unsafe abortion. All of these obstetric complications are well known and can be managed effectively (Royston and Armstrong, 1989). Indirect causes include those that result from pre-existing conditions or diseases that are developed during pregnancy, which were not due to direct obstetric causes, but were aggravated by physiologic effects of pregnancy. These indirect causes include conditions such as malaria, anemia, HIV and contribute to 20% of all maternal deaths globally. Maternal nutritional status and inadequate calorie intake during pregnancy are also important determinants for maternal and perinatal outcomes (Mobasheri and Golalipour, 2007; Khoushabi and Saraswathi, 2010; Borazjani et al., 2011).
In addition to these causes of maternal deaths, there are many other important determinants of maternal health or underlying causes, such as socio-cultural, economic and political factors. Among the underlying causes are low status of women in society, poor nutritional status of women, poor knowledge about hygiene during childbirth, literacy, decision making ability, access to gender sensitive facilities, lack of time and division of labor for women are all important determinants of maternal health.
Measurement of maternal mortality: Measuring maternal mortality ratio is complex and problematic, especially in developing countries due to weak health information and vital registration systems (Simkhada et al., 2009). Furthermore, methods that capture maternal mortality are time consuming, expensive and difficult to implement. Usually, program managers rely either on projections of Maternal Mortality which are published routinely by the Maternal Mortality Working Group (comprising of UN agencies: WHO, UNICEF, UNFPA, UNDP, academic groups and partners) or on population based surveys or censuses that happen every ten years. Figure 2 highlights the differing maternal mortality ratios obtained from different sources obtained using different methodologies unadjusted using primary data and adjusted or predicted estimates for SEAR countries. These discrepancies are quite large and merit further detailed analysis and research but are beyond the scope of this technical paper.
Given these difficulties associated with measurement of maternal mortality ratio, WHO recommends that countries use process indicators, such as the percentage of deliveries assisted by skilled attendants. There are clear clinical justifications for the presence of a skilled attendant at delivery, as this may reduce both the incidence of life threatening complications arising during childbirth, e.g., post-partum hemorrhage, sepsis and eclampsia. It is also essential for the survival of the newborn that may need immediate resuscitation to survive. Evidence also shows reduced maternal mortality ratios with skilled attendance at birth (WHO, 2005; De Brouwere et al., 1998).
The caesarean section (C-section) rate- proportion of deliveries carried out by C-section from all deliveries (not only those occur in health facilities)-is also often used as an indicator for understanding maternal health service in a country. The rationale for using the C-section rate is based on the premise that in the absence of C-section, many women with serious obstetric complications (obstructed labour, eclampsia, or intractable haemorrhage) will die during childbirth if such service is not available. However, there is potential for over-estimation as many times caesarean sections are overused or used for inappropriate indications especially in private-for-profit institutions in developing countries. Also, many times, the C-section rate is calculated using inappropriate denominator, i.e., number of deliveries in hospitals, while the proportion of deliveries in health facilities is very low as these settings.
Maternal health services: Based on the global evidence base, SEAR countries have also been making investments to increase the availability, access, quality and coverage of safe obstetric and newborn care. As countries make substantive efforts to achieve MDGs 4 and 5 there has been an increasing proportion of deliveries attended by skilled health workers. Although, there is still a long way to go before ensuring skilled attendance at all deliveries, the progress is promising; albeit a little slow. Figure 3 shows the trends in the proportion of births attended by skilled health personnel in SEA countries between 1990 and 2005 and also the projection for 2015. Bangladesh and Nepal have made slow progress over the years in increasing the coverage of skilled health personnel at the time of birth from 5% in 1990 to 13% in 2005 (Bangladesh) and 7% in 1990 to 18.7% in 2005 (Nepal). These countries will most likely not achieve the targets for skilled birth attendance at 2015. However, three countries in the region namely Thailand, Sri Lanka and DPRK have achieved universal coverage of skilled attendants at the time of birth, while Maldives is likely to achieve the same in the next few years. However, it is also encouraging to note that midwifery training programs are in place in almost the rest of SEA countries through competency based in-service and pre-service curriculum.
Figure 4 shows the proportion of births attended by skilled health personnel in five countries in SEAR between 2002 and 2006 vis-à-vis place of residence, wealth and education of the mother. Major differences can be seen within and between countries in terms of the percentage of births attended by skilled health personnel across these different categories. In the Region, Thailand has the least inequities; whereas Nepal, Bangladesh, India and Indonesia have widespread inequities in the percent of births attended by skilled health personnel vis-à-vis place of residence, wealth and education of the mother.
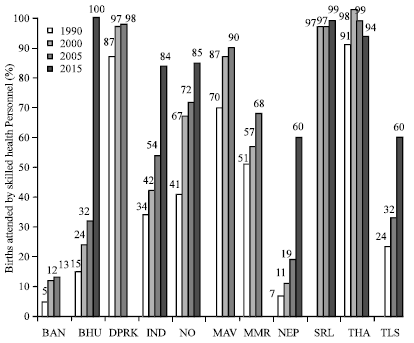 | |
| Fig. 3: | Trends in the proportion of births attended by skilled health personnel, 1990-2005 and projection for 2015 (WHO, 2007a) |
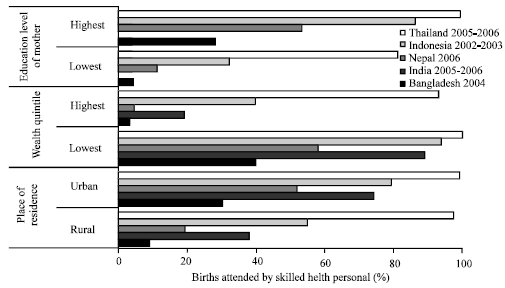 | |
| Fig. 4: | Comparison of births attended by skilled health personnel in five countries between 2002 and 2006 with relation to education of the mother, wealth quintile and place of residence (WHO, 2009) |
Neonatal mortality: Neonates have the highest risk of death among all children. It is estimated that almost 99% of the world’s neonatal deaths occur in low-income and middle-income countries, primarily in South Asia and Sub-Saharan Africa (WHO, 2007a). In the SEA region-India, Nepal Bangladesh, Myanmar and Indonesia contribute to 99% of the total neonatal deaths. Out of these, India has a 76.6% contribution to the regional burden of neonatal deaths. Figure 5 shows the number of neonatal and early neonatal deaths in SEA countries and the proportion of deaths in individual countries in 2004.
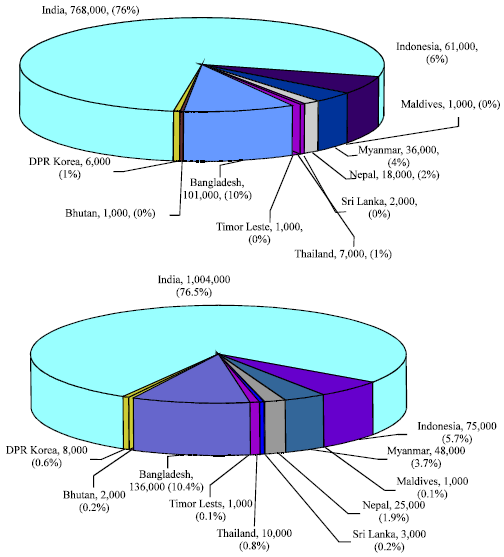 | |
| Fig. 5: | Number of early neonatal deaths and proportion of neonatal deaths in SEAR countries (WHO, 2007a, 2009) |
There were approximately 1.31 million neonatal deaths in SEA countries, out of which 1.002 million (76.48%) occurred during the first seven days; the early neonatal period.
Many SEA countries have made substantial progress in reducing under-5 and infant mortality rates through the success of many programmatic efforts, such as: Immunization, IMCI, CDD, ARI and Nutrition. However, reduction of neonatal mortality, which is intrinsically linked to maternal health, remains a critical bottleneck in many countries. Reduction in neonatal mortality is of paramount importance if countries are to achieve the millennium development goals for child survival.
Causes and determinants of neonatal mortality: The major causes of neonatal deaths are infections, prematurity, low birth weight and birth asphyxia. The most important among these are infectious causes as illustrated in Fig. 6. Similar to maternal mortality, numerous socio-cultural, economic and other factors also come into play (Uddin and Hossain, 2010), all of which contribute significantly to the high rates of neonatal deaths in SEAR. Evidence shows that most neonatal deaths can be prevented if women have access to basic health care services during pregnancy, childbirth and the postnatal period.
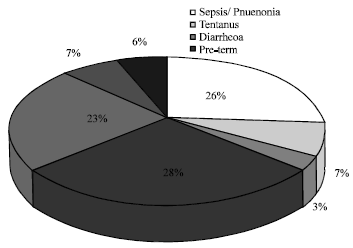 | |
| Fig. 6: | Causes of neonatal deaths (Lawn et al., 2005) |
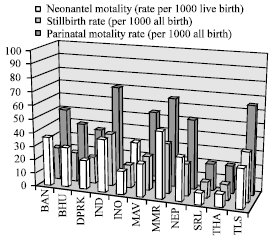 | |
| Fig. 7: | Perinatal and neonatal mortality in SEAR (WHO, 2007a, 2009) |
These include skilled midwifery care during childbirth, timely and appropriate treatment of newborn infections, proper attention to hygiene, warmth, immediate breastfeeding and immunizations to protect expectant mothers and newborns against tetanus (Tinker et al., 2009). These interventions are simple, feasible, cost effective and have substantially demonstrated reduction of neonatal mortality rates in various settings, including in South Asia.
Ministries of health in SEA countries along with supportive developmental partners are making great strides to improve the quality of MNH services to reduce the high burden of neonatal deaths. Some countries are also implementing innovative community-based models essential newborn care provision and early recognition and treatment of sick neonates through the training of community-based health workers and volunteers. This holds great promise for countries which have low levels of institutional deliveries and where most babies die without ever coming in contact with the formal health care system.
Stillbirth: Although, stillbirths are a dreadful outcome of pregnancy, appropriate protocols for identification and recording of stillbirths are not a part of national health management information systems of SEAR countries. We know that stillbirths are either equal to or more likely to exceed the number of neonatal deaths (Macfarlane and Mugford, 2000). Figure 7 demonstrates the variations in perinatal and neonatal mortality and stillbirths in SEAR countries.
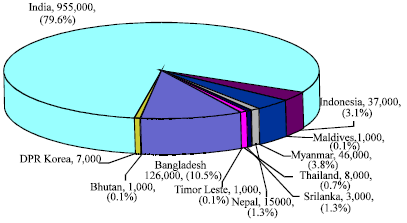 | |
| Fig. 8: | Burden of stillbirths in the South-East Asia Region (WHO, 2007a, b, 2009) |
According to WHO estimates, the stillbirth rate for South-East Asia for the year 2000 was 33 per 1000 live births. Further, out of the estimated total 1.3 million stillbirths, 36% were estimated to be intra-partumstillbirths (WHO, 2007a). This is a substantial proportion of all perinatal deaths in the Region and can largely be prevented through good obstetric care. We know that earlier the timing of death of the baby, the higher are the chances for under reporting. It is also well acknowledged that stillbirths generally tend to be more under reported than live births (Greb et al., 1987; Harter et al., 1986).
Causes and determinants of stillbirth: Early neonatal deaths and stillbirths usually have obstetric causes and are largely preventable if good quality obstetric care is made available at the right time (Zadkarami, 2008). The rates of intrapartum stillbirths are a sensitive measure of the quality of intrapartum care (Lawn et al., 2009). Where women receive good care during childbirth, intrapartum deaths represent less than 10% of stillbirths due to severe unexpected complications (WHO, 2007a). Figure 8 demonstrates the situation of stillbirths in SEAR countries where 79.6% of the total burden of stillbirths is in India.
Measurement of stillbirths and intrapartum deaths: There are many challenges which limit the accurate measurement and recording of stillbirths routinely. Most countries in the Region, such as Bangladesh, India, Nepal and Timor-Leste have low rates of institutional deliveries; hence capturing stillbirths only from the hospital-based data would not reflect the real situation, as most babies are actually born outside health facilities. Eliciting pregnancy and birth history during population-based surveys also run the risk of being incomplete and tend to suffer from recall biases, especially related to the exact timing of death (Harter et al., 1986). The chances of under reporting of stillbirths are also higher when deaths are early on in the pregnancy. Generally, stillbirths tend to be more under reported than babies who were born alive but later died (Macfarlane and Mugford, 2000; Greb et al., 1987). As long as countries do not prioritize perinatal health issues and design monitoring systems that capture both antepartum and intrapartum stillbirths, the reporting of stillbirths will remain weak. Capturing the timing of death of the unborn babies will help us formulate effective interventions to address the high rates of stillbirth and early neonatal mortality (WHO, 2007a).
DISCUSSION
This section will discuss the key issues, challenges and provide recommendations to countries for improving maternal, neonatal and perinatal mortality in South Asia. Discussion has been focused to four key themes, all of which are in the purview of health system strengthening for improving maternal, perinatal and health.
Strengthening monitoring information systems for maternal and perinatal health: Although the levels of maternal, neonatal mortality and stillbirths are acknowledged to be strong indicators of health and socio-economic status of countries, robust good quality data on these is lacking in SEA countries. Information about maternal and neonatal mortality and stillbirth are mostly obtained by estimation through statistical modeling methods or from household-based population surveys with cluster sampling methodologies in order to produce nationally representative samples. Problems in measurement include (1) weak vital registration, (2) misclassification (3) difficulties in capturing timing of deaths and (4) under reporting of deaths esp. for stillbirths and early neonatal deaths (Harter et al., 1986). The exact numbers of mothers and newborns who die around the time of delivery and the postpartum period are therefore difficult to ascertain and usually rely on estimates and projections. There needs to be further research done to critically examine the discrepancies that exist between global estimates and national estimates. It is increasingly being acknowledged that there is a need to move beyond estimates and projections of mortality related data.
Strategic investments need to be made so that every mother and newborn whether alive or stillborn is accounted for within the system. Plans to strengthen birth registration and vital registrations systems must be operational at the national level. Countries should work towards developing robust systems of surveillance that captures morbidity and mortality related events in a timely and comprehensive fashion. This information is essential for critically assessing program performance, perform adjustments and support program implementation. Dissemination of data widely is necessary for ensuring accountability and for advocacy. There should be a continuous cycle of planning, implementation, monitoring and evaluation and information use. Program managers must also bear in mind the usage of data that is generated from the monitoring and evaluation system. Information collected must be used to provide institutional feedback and serve as a quality assurance mechanism. Health information should also be made available to the broader public, civil society and community level influentials so that all multiple sectors are engaged in maternal and perinatal health issues and ensure that the health system is responsive to the needs to the people and is held accountable for results. Efforts to streamline information generated from all maternal and perinatal health programs must be done so that the national Health Monitoring Information System (HMIS) captures all these information and is strengthened. Parallel systems of data collection and use must be discouraged. A robust monitoring and evaluation system also offers many possibilities for integration with other programs and systems that also capture pregnancy related information.
Health systems strengthening for maternal and perinatal health: The last few years have seen a renewed commitment towards revitalization of primary health care and strengthening of health systems. Health system strengthening is defined as improving the six health system building blocks, which include: (1) service delivery; (2) health workforce; (3) information; (4) medical, products, vaccines and technologies; (5) financing; (6) leadership and governance and managing their interaction in ways that achieve more equitable and sustained improvements of health services and outcomes (WHO, 2007b).This move towards health system strengthening and revitalization of primary health care comes at the right time as SEA countries work towards achieving the targets of the MDGs.
As described previously, there are many challenges in reducing maternal and perinatal deaths in the Region. Bangladesh, Nepal and Timor-Leste all have less than 20% skilled attendance at birth. To tackle these challenges, many countries in SEAR have formulated evidence-based, strategic policies and programs that are innovative, focus on implementation at scale and follow established best practices and models for reducing maternal and neonatal deaths in resource constrained settings. The programs and packages include recommended interventions from the Lancet series on newborn survival (2005), maternal survival (2006) and on reproductive health (2006), which, if implemented at scale, has the potential to substantially reduce both neonatal and maternal deaths. Some of these interventions include (1) Comprehensive family planning; (2) Safe abortion services; (3) Antenatal care; (4) Skilled attendance at birth and emergency obstetric and neonatal care; (5) Postnatal care for the newborn and the mothers. Planners and policy makers must prioritize interventions and implement the most feasible and cost effective ones. All of this must be done under the broad umbrella of health systems strengthening and revitalizing primary health care efforts.
There has also been a gradual shift towards an integrated service delivery platform for maternal and neonatal health as compared to the previous vertical approaches which targeted specific diseases or stages in the lifecycle. Programs now focus on providing care throughout the lifecycle continuum (from pre-pregnancy, pregnancy, childbirth and infancy), placing emphasis on strengthening effective linkages with the health care system and the household to hospital continuum.
There are numerous examples to illustrate the significant positive developments in SEAR countries over the past decade. The National Rural Health Mission reflects the Government of India’s commitment to reduce maternal and neonatal deaths and achieve MDG 4 and 5. The JananiSurakshaYojana (India), Safe Delivery Incentive Program- AamaSurakshaKaryakram (Nepal) and Demand Side Financing by providing maternal health voucher for the poor women in Bangladesh are all great examples of the innovative work being done in the Region to remove demand side barriers to care seeking and employ models which use conditional cash transfers to pregnant women for increasing institutional births and incentives to health workers for providing skilled attendance at birth (Lim et al., 2010; ICDDR-B, 2008).
Improving quality of services: Countries need to work towards developing an effective skilled attendance system, which includes care from a skilled provider, a policy environment that promotes skilled, client-centered care, a functioning system for stabilization and referral, the availability of essential equipment and supplies and community demand for high quality services for mothers and children. To help strengthen the components of skilled attendance system, countries can use available tools in order to achieve the desired performance at service delivery sites and within communities. Provision of high quality services are fundamental to ensure that services are utilized by people (Ferdous and Zafrul Azam, 2009). As countries increase coverage rates of skilled attendance, Quality of obstetric care needs to be ensured so that skilled care at the point of contact actually has an impact on the population (Shahraki et al., 2007).
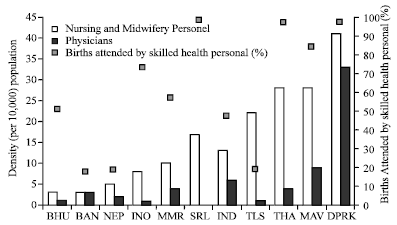 | |
| Fig. 9: | SBA coverage rates in countries and density of health workers (WHO, 2007b) |
Quality improvement can be done through defining operational standards, assessing clinical and community performance, identifying targeted, cost-effective interventions to improve birth preparedness and complication readiness and service quality in maternal and newborn care, monitor and evaluate performance. Institutionalizing maternal and perinatal death audits are also a good starting point for a quality improvement process. Competency-based pre-service and in-service trainings for health workers, supportive supervision mechanisms, effective workforce management, development of infrastructure and financing mechanisms will all contribute in improving the quality of care.
Ensuring availability of human resources: The provision of essential interventions during pregnancy, childbirth and in the immediate post-partum period by adequately skilled health personnel is a recognized strategy for the reduction of maternal and perinatal deaths. Based on the convincing evidence of mortality reduction as a result of skilled health worker attendance at birth, countries around the world have been making significant investments to scale up skilled care during childbirth (Graham et al., 2001). At the global level, the World Health Report 2005 and 2006 and other important documents have also highlighted the importance of investing and developing motivated, supportive health workers in achieving national and global targets and commitments. The deliberations at the special session of the UN General Assembly in 1999, which was held as a follow up to the International Conference on Population and Development (ICPD), also recommended that globally 80, 85 and 90% of all births should be assisted by skilled attendants by 2005, 2010 and 2015 respectively (United Nations, 1999). At the regional level, efforts are also underway to facilitate and strengthen national databases on human resources for maternal and newborn health and also develop national plans to address gaps and ensure adequate resources and effective implementation.
Similar to high mortality settings elsewhere, four countries in SEAR, namely Bangladesh, India, Nepal and Timor-Leste have also had to struggle with the availability of adequate number of skilled health personnels (WHO, 2007b). Figure 9 demonstrates higher rates of skilled attendance at birth in countries, such as DPR Korea, Maldives, Thailand and Sri Lanka, all of which have a high density of nursing and midwifery personnel per 10,000 population.
There are many challenges for increasing the coverage of skilled attendance during childbirth and in the immediate postpartum period in SEAR. Human Resource Information Systems are lacking in most developing countries (Farahbakhsh et al., 2007). Systems with accurate information regarding the numbers, categories, classifications and placements of skilled health workers is lacking in most SEAR countries. Standards regarding nursing and midwifery health care workforce, their training curricula, roles and responsibilities, positions, regulatory authorities and guidelines vary in different countries.
In addition, there is an inadequate production capacity, lack of appropriate knowledge and skills, limited public health orientation, planning and managerial challenges, non-existent or non-operationalized national plans for skilled health workforce. This skilled human resource deficit is one of the greatest challenges for scaling up essential health care service in the Region. Estimates indicate that SEAR is experiencing a shortage of between 650,000 and 1,500,000 doctors, nurses and midwives. The most affected countries being Bangladesh, Nepal, Bhutan, and Indonesia which have less than one doctor nurse and midwife eac h per 1000 population (WHO-SEARO, 2006). A closer examination reveals many underlying factors contributing to this deficit. Some of these include difficulties in attracting, retaining and deploying the public health workforce due to poor working conditions, low salary scales, hardships, migration of skilled health workforce, lack of proper incentives or appropriate career ladder, preference for urban and developed areas, political appointments and transfers, misdistribution and ad-hoc transfer of staff. Compounding these factors is the fact that there is a preference for the production of specialist doctors and nurses rather than a dynamic public health workforce.
The way forward for countries is by developing realistic and effective national plans that can be implemented. Strategies need to be formulated according to the unique situation of skilled health workforce and needs of individual countries. They must take into account the full spectrum of health workers both in public and private sectors/NGOs. National planners must design comprehensive strategies that are holistic in their approach and consider short-term, medium-term and long-term approaches towards increasing skilled attendance. Short-term strategies may include providing training and support to the existing cadre of health care workers, development of an effective human resource information system to improve personnel management and planning, retaining and attracting health workers within the public health system by providing incentives for future career growth, etc. Mid-term strategies include scaling up skilled human resources for health, especially at the primary care level where most births and deaths occur.
Task shifting offers great promise for the interim period in order to scale up the coverage of essential health care service and in expanding coverage and increasing access to emergency obstetric services. However, it is important to note that these approaches only work as a part of the overall strategy of revitalizing primary health care and strengthening human resources for health. Shifting tasks from one cadre to another will not work if there are (1) deficient numbers of health workers; (2) excessive and increasing workload; (3) low remuneration issues; (4) lack of training; and (5) poor quality of care. Long term strategies will entail development of an effective human resource development plan, which can be operationalized and leads to universal access to skilled attendance during childbirth.
CONCLUSION
In order to achieve MDGs 4 and 5 targets, countries must prioritize programs and packages that provide a continuum of care for maternal, newborn and child health. Proven, simple, cost-effective and feasible solutions to save the lives of mothers and newborns already exist. These should be provided within an integrated health service delivery mechanism throughout the lifecycle and need to be supported by effective linkages to well-functioning referral systems. Improvements in maternal and perinatal health must go together with efforts to revitalize primary health care and strengthen the six pillars of health system to ensure that gains are sustained over the longer term. As countries increase coverage of skilled attendants, it is important to mainstream quality of care activities so that further progress can be made. Quality improvement has potential to reduce a large number of early neonatal deaths, stillbirths and maternal deaths but it is a long term process which needs sustained commitment and ownership. Human Resource shortages are the most critical bottleneck in the Region and effective human resource strategies need to be formulated and operationalized. More than any other time in history, a momentum towards accountability and transparency is gaining ground and all partners must work together to institutionalize these values.
REFERENCES
- Shahraki, A.D., J.H. Akhtar and E. Moazam, 2007. Maternal mortality in Isfahan province 2001-2006. J. Medical Sci., 7: 1340-1344.
CrossRefDirect Link - Campbell, O.M.R. and W.J. Graham, 2006. Strategies for reducing maternal mortality: Getting on with what works. Lancet, 368: 1284-1299.
CrossRef - De Brouwere, V., V. De Brouwere, R. Tonglet and W. Van Lerberghe, 1998. Strategies for reducing maternal mortality in developing countries: What can we learn from the history of the industrialised West? Trop. Med. Int. Health, 3: 771-782.
CrossRef - Mobasheri, E. and M.J. Golalipour, 2007. The effect of pre-pregnancy body mass index on gestational weight gain and pregnancy outcome in Gorgan, North Iran. J. Med. Sci., 7: 905-908.
CrossRefDirect Link - Ferdous, F.B. and A.T.M. Zafrul Azam, 2009. Utilization of child health care services in Thana health complex of Bangladesh: A study of Keraniganj. Asian J. Epidemiol., 2: 20-32.
CrossRefDirect Link - Khoushabi, F. and G. Saraswathi, 2010. Association between maternal nutrition status and birth weight of neonates in selected hospitals in Mysore city, India. Pak. J. Nutr., 9: 1124-1130.
CrossRefDirect Link - Borazjani, F., S.S. Kulkarni and K.A. Ahmadi, 2011. Impact of maternal factors on birth parameters in urban affluent pregnant women. Pak. J. Nutr., 10: 325-327.
CrossRefDirect Link - Greb, A.E., R.M. Pauli and R.S. Kirby, 1987. Accuracy of fetal death reports: Comparison with data from an independent stillbirth assessment program. Am. J. Public Health, 77: 1202-1206.
Direct Link - Harter, L., P. Starzyk and F. Frost, 1986. A comparative study of hospital fetal death records and Washington State fetal death certificates. Am. J. Public Health, 76: 1333-1334.
Direct Link - Lawn, J.E., A.C. Lee, M. Kinney, L. Sibley and W.A. Carlo et al., 2009. Two million intrapartum stillbirths and neonatal deaths: Where, why and what can we do?. Int. J. Gynecol. Obstet., 107: S5-S19.
Direct Link - Lim, S.S., L. Dandona, J.A. Hoisington, S.L. James, M.C. Hogan and E. Gakidou, 2010. India's janani suraksha yojana, a conditional cash transfer programme to increase births in health facilities: An impact evaluation. Lancet, 375: 2009-2023.
CrossRef - Zadkarami, M.R., 2008. Risk factors for perinatal mortality: Random effect model. Asian J. Epidemiol., 1: 53-63.
CrossRefDirect Link - Simkhada, P., E. van Teijlingen, S. Kadel, J. Stephens, S. Sharma and M. Sharma, 2009. Reliability of national data sets evidence from a detailed small area study in rural kathmandu Valley, Nepal. Asian J. Epidemiol., 2: 44-48.
CrossRefDirect Link - Farahbakhsh, M., S. Fozounkhah, H. Sadeghi-Bazargani, A. Zakeri, N. Houshiyan, N. Asmani and A. Naghili, 2007. The study of health information system performance from managers and expert's viewpoints. Inform. Technol. J., 6: 227-231.
CrossRefDirect Link








