Research Article
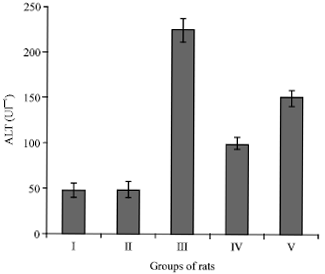
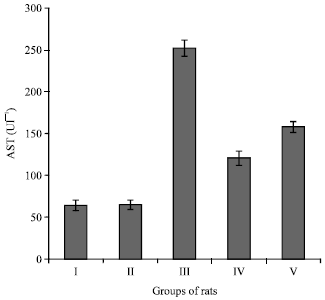
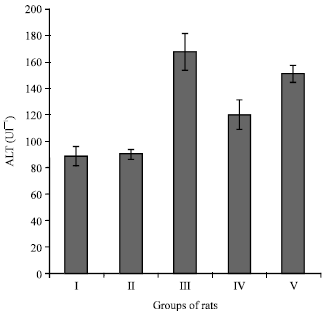
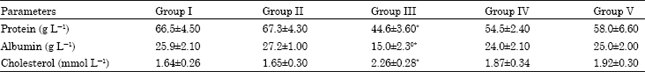
Hepatoprotective Effects of Camel Milk against CCl4-induced Hepatotoxicity in Rats
Department of Medical Laboratories, College of Applied Medical Sciences, Qassim University, Qassim-51452, Saudi Arabia
LiveDNA: 91.2879
Mohammad A. Alzohairy
Department of Medical Laboratories, College of Applied Medical Sciences, Qassim University, Qassim-51452, Saudi Arabia