Research Article
Effect of Tight Naqab on Intraocular Pressure: A Prospective Study
Medical School, King Faisal University, P.O. Box 2247 Al-Ahsa 31982, Kingdom of Saudi Arabia
In Saudi Arabia, wearing Naqab is an Islamic tradition among ladies. In a hospital based study in the western Saudi Arabia, researchers reported 17.7% prevalence of glaucoma (Eid et al., 2009). While community based surveys in the neighboring Arab countries revealed that the prevalence of glaucoma was 2% in Qatar (Al-Mansouri et al., 2011) and 4.75% in Oman (Khandekar et al., 2008). Females accounted for 10 and 50% of the population with glaucoma, respectively in these two studies. Elevated intraocular pressure (IOP) due to various reasons remains the most important known risk factor for the development and progression of glaucomatous damage to optic nerve head (Prata et al., 2011). Therefore, accurate measurement of IOP is crucial in making decisions regarding its management. Majority of elderly Saudi women wear tight headgear called ‘Naqab’ encircling the forehead throughout the day and continue wearing them during IOP measurements. The clinicians have observed that use of such naqab for a longer period result in change of color and texture of skin of the forehead and part of face. The investigators hypothesized that this may elevate IOP by increasing episcleral venous pressure and/or by lymphatic drainage obstruction. During routine examination, if a patient was wearing a tight Niqab, the increased IOP could lead to an erroneous diagnosis of ocular hypertension or even glaucoma. Moreover, if the patient consistently wears a tight Niqab as a normal preference in daily life, this could lead to a sustained increase in IOP and could predispose to the development of glaucomatous optic neuropathy, thereby rendering a tight Naqab a risk factor as well as a confounder of accurate IOP measurement. Therefore, the main aim of this study was to evaluate the effect of Naqab on IOP measurement by Goldmann applanation tonometry.
The study was conducted in a hospital of Eastern Province of Saudi Arabia. It is university affiliated tertiary eye unit. A permission was sought from the local ethical committee of Al-Ahsa to undertake this study. A series of such case studies were conducted in 2011.
It was assumed that the use of Naqab can increase the mean IOP from 17 mmHg (SD±3 mmHg) to 19 mmHg (SD±4 mmHg). In order to achieve 95% confidence level, it was required to examine 100 eyes of 50 participants before and after use of Naqab. To compensate the loss of data, the sample size was increased by 20%, thus bringing the total number of final sample of study to 120 eyes of 60 Saudi ladies using Naqab.
Adult lady patients, using Naqab and attending the hospital, were the study sample population. Also, those agreed to participate in this study and were not suffering from infectious eye disease were included for examination. The ladies, who had undergone eye surgery in the past or did not agree to remove Naqab for one hour, were excluded from the study.
The field investigation team consisted of 2-senior ophthalmologists. They measured IOP using applanation tonometer (Goldmann, Germany) attached to the slit-lamp bio-microscope (Topcon, Japan). The IOP was measured before and after 1, 2 and 3 h wearing Naqab. To measure the IOP, Naqab was removed and the first measurement of IOP was taken after 15 min. This was followed by 3 measurements by keeping the Naqab in place and the IOP was measured through the eye openings of the naqab. The face and the eyes of the patients were not touched in the entire examination.
If the ophthalmologist had already diagnosed glaucoma in the past and given medication to control the IOP, the eye was labeled as glaucomatous. A detailed eye examination was carried to rule out glaucoma for the rest of the participants. Those subjects with IOP = 21 mmHg (by Goldmann applanation tonometry), normal optic disc appearance based upon clinical examination and the normal automated perimetry were considered normal. Normal optic disc appearance was defined as vertical cup to disc asymmetry = 0.2, cup/disc ratio = 0.6 and an intact neuroretinal rim without peripapillary haemorrhages, notches or localised pallor. Glaucoma patients had glaucomatous optic disc changes damage and associated visual field loss in the corresponding hemifield location. Glaucomatous optic neuropathy was defined as the cup/disc asymmetry between the eyes of >0.2, rim thinning, notching or excavation.
Data analysis: The data was entered in Microsoft XL spreadsheet. The statistical analysis was carried using SPSS, version 12 software (IBM, Boston, USA). The IOP measurements were subjected to paired t tests. A p value of 0.05 or less was considered statistically significant. Histogram was used to review distribution of IOP among participants. As distribution was skewed, the log values of IOP calculated and then performed the univariate analysis by parametric method. A LOG10 function of Microsoft xl was used to calculate log value of IOP. Also, the mean and standard deviation of log of IOP were calculated and then used formula of 10Y (y = mean antilog of IOP) to calculate mean of IOP, standard deviation, difference of mean and its 95% confidence intervals.
The data for the rise of IOP after two hours of wearing Naqab into = 2 and <2 mmHg was grouped. Using this rise of IOP as dependent variable, multi-nominal regression analysis was carried out. The dependent variables were IOP without Naqab, glaucoma status of eye, investigator and the eye involved. The mean and standard deviation of IOP were calculated. The IOP of eyes among subgroups of glaucoma and non-glaucoma, right and left eyes were compared.
Sixty subjects with age between 20 to 70 years having 120 eyes were enrolled in the study. Thirty ladies were using medications for controlling glaucoma while the same number was those without glaucoma. The intraocular pressures (IOPs) without wearing Naqab and after 1, 2 and 3 h of wearing naqab were compared (Table 1). Mean IOP in normal subjects increased by 1.3 mmHg (p = 0.05) and in glaucoma patient by 1 mmHg (p = 0.067) one hour after using the Naqab, but after 2 and 3 h of wearing Naqab the mean IOP in normal subjects increased by 2.1 mm Hg (p = 0.0001) and in glaucoma patients by 1.3 mm Hg (p = 0.02) and 1.25 (p = 0<.02) mm Hg, respectively.
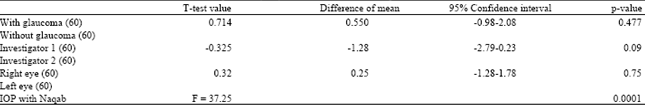
The binominal regression analysis showed that apart from Naqab (p = 0.0001, paired t-test), no other covariates such as glaucoma (p = 0.477, paired t-test), laterality (p = 0.75, paired t-test), investigators (p = 0.09, paired t-test) showed significant influence on the rise of IOP by 2 mm Hg or more after 2 h wearing the Naqab (Table 2).
Accurate measurement of IOP is necessary for the detection and proper management of glaucoma. The IOP readings can be affected by different factors such as instrumental, physiological, examiner induced and patient induced which can lead to erroneous and inaccurate readings.
In the present study, a rise in IOP following the use of Naqab (Patient induced) was clearly established. There was a significant rise of intraocular pressure with the mean IOP increasing at 2 h and remaining the same at 3 h after the use of Naqab. Apart from IOP without naqab, no other factors significantly influenced the rise of IOP after the use of Naqab. Both in monkeys and human beings, lymphatic drainage of orbit and intraocular tissues have been documented to take place to the cervical lymph nodes (McGetrick et al., 1989; Camelo et al., 2008). Any mechanism that hampers free flow of lymph and reduce the drainage of aqueous humor could increase the intraocular pressure (IOP). According to one research, tight neck-tie increased IOP in both the normal and glaucomatous subjects (Teng et al., 1987). Elevated jugular vein pressure resulting in elevated episcleral established that orbital venous pressure plays an important role in IOP homeostasis and ocular hemodynamic (Herbert and Kiel, 2002). In one study, the researcher noted about 4.5 mm Hg rises in IOP after using the swimming goggles (Morgan et al., 2008). Therefore, Tight fitting Naqab might be responsible for alteration in venous and lymphatic flow contributing to rise of IOP.
The removal of such Naqab might bring the IOP to its original level in Saudi ladies in the present study. There was no significant difference in the IOP elevation two hours after the use of Naqab among ladies with and without glaucoma. The glaucoma patients using medications have shown improved outflow of aqueous humor in their eyes (Greve et al., 1997).
| Table 1: | Goldmann applanation tonometry means IOP (SD) (range) measurements before and after one, two and three hours of application of naqab |
 | |
| Table 2: | Factors associated for the rise of Intra ocular pressure (IOP) two hours after use of naqab |
 | |
Most of the venous pressure was presumed to be the cause of this high IOP. In an experimental study on rabbit, it has been glaucoma medications do not significantly affect drainage aqueous beyond schelemn’s canal. Perhaps, the use of Naqab might cause back pressure and reduce drainage of aqueous. As Naqab equally affects the reduced drainage of aqueous in glaucomatous eyes treated with medications and non glaucomatous eyes, no significant difference was observed in these two groups.
The absence of significant variation in measurement of IOP at different times by two investigators in each eye of a lady suggests uniform pattern of measuring IOP and minimum influence of measurement bias in the present study. If the target pressure in a female patient following glaucoma surgery is not achieved, judicious use of Naqab in Saudi ladies could be attempted to increase IOP especially by 2 to 4 mm Hg during peaks in diurnal variations especially in person with glaucoma (Goel et al., 2010; Draeger, 2010).
To the best of our knowledge, this is the first such study to review the influence of Naqab on IOP. However, the present study being a case series had few limitations. Further studies of longitudinal type with larger sample are recommended to confirm the hypothesis of influence of using naqab on rise of IOP.
Naqab that encircles head and face seems to influence the intraocular pressure among Saudi ladies and is a confounder of accurate IOP measurement. However, this observation needs to be confirmed with a larger sample. Even the factors causing this rise of IOP after the use of Naqab needs further investigation. The rise of IOP after wearing Naqab should be accounted for before interpreting the IOP in ladies using Naqab. The ophthalmologist conducting comprehensive eye examination of adult lady patients should note change in IOP among ladies who usually wear naqab.