Research Article
Evaluation of Anti Measles IgG Prior to Mass Vaccination in Soldiers in Iran
Military Health Research Center, Baqiyatallah Medical Sciences University, Iran Immunology Research Center Baqiyatallah Medical Sciences University, Iran
Measles caused by the paramyxovirus, which spreads through airborne droplets. The disease has an incubation period of between 6 and 19 days. People with measles are usually infectious for one to two days before the rash appears but the total period during which an individual is infectious is not known (Bedford, 2004).
Measles is a highly contagious respiratory virus infection, with typical clinical symptoms including maculopapular rash, fever, cough, coryza and conjunctivitis. Measles is a highly infectious, acute viral illness that can cause severe pneumonia, diarrhea, encephalitis and death. Despite implementation of widespread vaccination programs throughout the world, the rates of global morbidity and mortality are still considerable (Roodbari et al., 2003).
Measles, in spite of available vaccination, remains a heavy public health burden worldwide especially in developing countries with 30-40 million cases and 745000 deaths in the year 2001. This represents 50-60% of the estimated million deaths attributable to vaccine-preventable diseases of childhood. Measles may be ultimately responsible for more child deaths than any other single agent because of complications may from pneumonia, diarrhea and malnutrition. Measles is also the major cause of preventable blindness in the world, affecting the same disadvantaged populations (Epidemiology of Measles, 2004).
Of the deaths attributable to measles, 98% occur in developing countries. Case-fatality rates in these countries were been usually estimated to be in the range 1-5% but may reach 10-30% in some situations (Roodbari et al., 2003; Epidemiology of Measles, 2004; WWW. WHO, 2003). Measles vaccination is one of the most cost effective health interventions available and one of the most powerful tools for providing health equity to poor children (WWW. WHO, 2003).
As the natural route of infection for measles virus is the respiratory tract, administration of live attenuated measles vaccine through the respiratory tract was been investigated as an alternative to injection (WWW. WHO. measles initiative, 2003; http://www.nicd.ac.za/pubs/comdis/ 2004/nov 04_5.htm).
An outbreak of measles in adult may be due to unvaccinated in childhood or primary and secondary vaccine failure. Life attenuated measles vaccines have dramatically reduced measles morbidity and mortality worldwide. Despite high vaccination coverage, measles outbreaks continue to occur in both developed and developing countries. While secondary vaccine failure may be responsible for measles outbreak (Pannuti et al., 2004; WWW.WHO. Measles vaccine, 2002; Loo et al., 2003; Mrazova et al., 2003).
Herd immunity and cellular immunity can prevention of measles outbreaks in adult (Gidding and Gilbert, 2001; Gdalevich et al., 2002; Lee et al., 1999). Despite almost universal use of measles vaccines, in recent decades epidemics of the disease continue to occur in adult especially in soldiers of army Iran (Roodbari et al., 2003; Loo et al., 2003; WHO/UNICEF, 2004). For this reasons we evaluated antimeals antibody and protectivity of measles in soldiers.
This evaluation is across-sectional descriptive study that was been carried out in 360 soldiers of army in capital city of Iran in 2003.
Question chart contain age smoking, education level, verbally history of anti measles vaccination, post history of measles and history of contact with measles patients in their family were been evaluated.
We determined the presence of anti measles IgG antibody by Enzyme Linked Immuno-Sorbent Assay (ELISA). Blood samples were been taken in 5 mL volume and sera were separated by centrifugation. The sera were been kept at -20°C until use. Antibody was titrated using whole virus Enzyme-Linked Immuno-Sorbent Assay (ELISA) for IgG isotype. Briefly, the 96 wells microtitration plates (flat bottom-Costar Co.) were coated with one hundreds antigens (Ag) (Razi Vaccine and Serum Res.) (35 μg protein mL-1 prepared in coating buffer (0.2/M Carbonate- Bicarbonate buffer pH, 9.6). The plates were been left at RT for 3 h. Then they were washed three times in PBS (pH, 7.4) containing 0.05% Tween 20. All wells were blocked using 100 μL PBS-T containing BSA 3% for 1 h incubation. After three additional washings in PBS-Tween, measles antibody was been quantified using a serum dilution at 100 μL. The WHO standard serum was diluted in to 1/5, 1/10, 1/20, 1/40 and 1/80. Negative and positive control serum was also included in each plate. Incubation was been continued for further 1 h. The plates were been washed three times in PBS-Tween and 100 μL of 1/250 dilution of Polyclonal anti-human IgG or IgM antibody conjugated to horseradish peroxidase (HRP) (Sigma Co.) were added in to appropriate wells. The plates were incubated for 30 min at RT and washed three times before the addition of 100 μL of substrate solution (6 mg ABTS in 10 mL citrate buffer 0.1M, PH 4.1 and 8 μL Hydrogenproxid 30%). The reaction was been stopped after 10 min at RT by the addition of 100 μL of H2SO4 1 mol. The optical Density (OD) was been read at 450 nm using an ELISA reader (Lab Systems Mutiskan MS). Titers of the sera with OD less than the mean OD of the 0/5 dilution of standard serum were classified as negative. This data were been analyzed in SPPS program computer.
In this study, all soldiers were men with mean age 20.4±0.89 SD. Anti measles IgG antibody was positive in 279 persons (77.7%) and 81 persons (22/5%) was negative. Education level was 53 (14.6%) nine years class, 276 (76.7%) diploma, 31 (8.6%) pre college that significant statically different between educating and IgG antibody (Table 1).
The cigarette smoking in 328 (91%) were negative and 32 (8.8%) were positive without statically different between smoking and antibody (Table 1).
Verbally history of vaccination was positive in 264 (73.3%) and 77 (21.3%) was negative 19 (5.3%) was unknown, without statically different between vaccination and antibody (Table 1).
Close contact with patients of measles was positive in 30 (8.3%), negative in 325 (90%) and five (1.4%) unknown, without statically different (Table 1).
Past history of measles was negative in 279 (77.5%), positive in 70 (19.4%) and 11 (3.1%) unknown without statically different.
Present study was been evaluated anti measles IgG antibody in soldiers because measles outbreaks were occurred in army of our country in recent decades. The incidence of measles declined after the introduction of the measles vaccination in children but in recent year's measles, outbreaks were been seen in adult especially in soldiers (Gidding and Gilbert, 2001; Gdalevich et al., 2002; Lee et al., 1999).
This study suggested that 22/5% of soldiers have not immunity against measles and it is a risk factor for outbreaks of measles in soldiers of our army. In other study confirmed that people without immunity than 5-10% were susceptible to measles outbreak for a reason our army forces were very high susceptible to measles outbreak (Gdalevich et al., 2002; Tariq, 2003; Lee et al., 2002).
| Table 1: | Antimeasles antibody IgG and education, smoking, history vaccination, close contact |
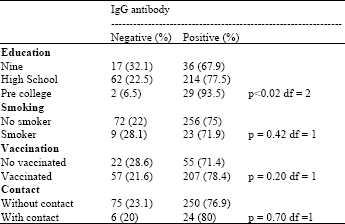 | |
Although in this study education was under college but in lower graduate have, the most susceptible to measles that may be this group did not had availability to vaccination program and vaccination coverage was low in their childhood on 15-20 years ago in our country. However, in recent years, vaccination coverage is very high and all children take two measles vaccine in 15 month after birth and 4-6 years old of age (WHO/UNICEF, 2004).
History of close contact with measles cases and measles in their family may be important to give up the herd immunity and causes periodic controlled the outbreak of measles but we cannot confirmed this question (Ehresmann et al., 2004; Lee et al., 1999).
Verbally history of vaccination confirmed that coverage of vaccination in two decade ago was low in our country, although it is not reliable but measles outbreak in our soldiers resemble to other studies may be to secondary failure of measles vaccine or lower coverage vaccine program in their childhood (Pannuti et al., 2004; Lee et al., 1999; Chiu et al., 1997; CDC, MMRW, 2004; WHO/UNICEF, 2004).
The smoking in earlier study was very low and we cannot determine the effects on immunity against measles (Apatzidou et al., 2005).
In this study, all soldiers were men that opposite to other study that woman was been evaluated because in our country we have not woman soldier in army.
Present results indicated that 22.5% of soldiers have not protectively against measles. For this reason and risk of the outbreak for measles in ours army, anti measles vaccination was be recommended for soldiers.
This study is part of research program that funded by Military Health Research Center, Military Medicine Institute, Baqiyatallah Medical Sciences University.