Case Study
Retronychia in a Renal Transplant Recipient
Department of Dermatology, Baskent University Faculty of Medicine, Ankara, Turkey
A. Tulin Gulec
Department of Dermatology, Baskent University Faculty of Medicine, Ankara, Turkey
Retronychia, which is actually a subtype of onychomadesis was first described by De Berker et al. (2008). Up till now there are approximately only 13 cases of retronychia and another case series of 19 patients reported in the literature. It is believed to be diagnosed underestimated. Retronychia is an incomplete form of nail shedding that leads to embedding of the nail into the proximal nail fold and subsequent inflammation (Dahdah et al., 2008; Baumgartner and Haneke, 2010). The etiology of this nail disorder is mainly based on chronic repeated minor trauma mostly caused by improperly fitted shoes or a single major traumatic event. The initial symptom of retronychia is often the disturbance of the longitudinal growth of the nail as a result of an acute physical or systemic traumatic process (Baran et al., 2001).
Up till now longitudinal ridging, leukonychia, onycholysis, transverse ridging, Muerchke’s nail, sirolimus-induced oncychopathy, sirolimus-associated chronic pyogenic periungual infection, ungual alternariosis and proximal white subungual onychomycosis have all been widely-recognized in renal transplantation recipients (Mahe et al., 2005; Baykal et al., 2000; Saray et al., 2004). Retronychia in a renal transplant recipient hasn’t been reported. Herein, we present a 24-year-old renal transplant recipient, presented with retronychia appeared on her left toenail.
CASE
A 24-year-old woman presented with hesitation of the growth and yellow discoloration of her both toenails for 3 years. She also complained about the split of her right toe nail that she noticed 3 months before. She also admitted the presence of the similar nail changes on her left toe nail 3 years ago. She had a renal transplantation 9 years ago for the renal insufficiency due to the familial Mediterranean fever and amyloidosis. Her medical history was otherwise unremarkable. Her medications included oral corticosteroid 5 mg day-1 and cyclosporine 175 mg day-1 since her transplantation. She also took mycofenolate mofetile which was discontinued 2 years after the transplantation. She didn’t remember any history of trauma or any pain.
Dermatological examination revealed that her left great toe nail was incompletely separated proximally from the underlying epithelium. This detached distal part of the nail was located above the level of the proximal nail (Fig. 1). As her both great toe nails were too short due to the discontinuation of the nail growth, a slight ingrown was also noticed in the distal lateral edges of the nail apparatus. The central part of the distal nail unit was partially detached and hang by its lateral edges. While this detached distal part was lusterless and yellow in color, the nail adjacent to the proximal nail fold was more viable, translucent and whitish. Her right great toe nail was normal except than a linear transverse line on the proximal (Fig. 2). No any periungal erythema or swelling was noticed.
 | |
| Fig. 1: | The detached distal part of the left great toe nail located above the level of the proximal nail |
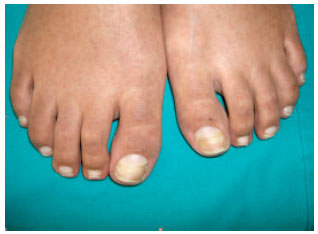 | |
| Fig. 2: | A proximal transverse line on her right great toe nail. The lusterless and yellowish detached distal part and more viable, translucent and whitish nail adjacent to the proximal nail fold |
Her finger nails were unremarkable except than the Terry nails seen in all her fingers. She was reassured and advised expectant observation for at least 3 months rather than the nail avulsion.
Retronychia actually describes an acute onychomadesis involving patients with a 3-6 months history of inflammation in the affected digits mostly seen in older individuals (Dahdah et al., 2008). Nearly all of the reported cases in the literature are known to be caused by a traumatic process. Up to now of the first five cases reported with retronychia, two; were seen in only one finger nail, the other two; in unilateral great toe nail and one; in bilateral great toe nails (Dahdah et al., 2008). No other toe nails except than the great toe nails were involved in these 5 patients.
Recently, a case series of 19 patients have also been reported. All these cases were described in meetings of the European Nail Society and collected from 5 different dermatology centers in Europe in 8 years (De Berker et al., 2008). The median age was reported to be 39 years (14-71). There was a significant female predominance (84%). While unilateral hand fingers were included in two patients, bilateral involvement was seen in only one. The remaining 13 patients reported unilateral toe nail changes and the other 3 patients also informed about their bilateral toe nail complaints. The duration of the nail alteration up to the time of the diagnosis was in between 2 to 24 months (De Berker et al., 2008). While in 7 of the 19 patients, no any cause was found, hiking, jogging, trauma, thrombophlebitis, arthritis, paronychia, poor footwear and high-heeled shoes were the other etiological factors reported (De Berker et al., 2008). All patients except than one patient were treated with nail avulsion with complete resolution. One patient was reported to improve spontaneously. CO2 laser of nail fold granulation tissue, antibiotics, topical and intra-lesional corticosteroids were also added to 7 of these patients (De Berker et al., 2008).
As the nail plaque grows through the outward direction, embedding mostly occurs into the lateral nail folds or the distal digital pulps. On the other hand retroncychia is known as one of the causes of the proximal nail ingrown. Failure of the longitudinal growth combined with a wedge-like effect of the new nail beneath, directs the overlying nail upwards into the proximal nail fold (Baran et al., 2001). This nonrecurrent pathology resolves by loss of the nail and may be due to the latent onychomadesis with nail retention favored by posterolateral ligamentous attraction of the nail plate (Baran et al., 2001). If the detachment of the nail from the proximal part of the nail unit is omitted for a long time, the ingrown of the nail to the ventral part of the proximal nail fold is usually inevitable. As the distal part of the nail is forced through the ventral part of the proximal nail fold, inflammation, periungal erythema and an increase in local temperature occurs commonly. Nail avulsion of the nail with retronychia may also reveal 3 generations of nails embedded into the proximal nail folds (Baumgartner and Haneke, 2010; Baran et al., 2001). Retronychia involves not only the toe nails but also the fingernails, mostly the single digits. It is also noted that retronychia may accompany with the synchronous development of the Beau’s lines on the other fingernails (De Berker et al., 2008; Dahdah et al., 2008).
In a case control study comparing the nail disorders in hemodialysis patients and renal transplant recipients, leukonychia was reported to be the most frequent nail pathology (21.5%) (Saray et al., 2004). Longitudinal ridging, leukonychia, onycholysis, transverse ridging, Muerchke’s nail were reported to be significantly more common in the renal transplant recipients rather than in the hemodialysis patients. Absence of lunula, splinter hemorrhage, onychomycosis, half-and-half nails, Terry’s nail were all the other nail disorders reported in the renal transplantation recipients (Saray et al., 2004). In the renal transplant recipients, the overall frequency of nail pathology was noted to increase significantly with age but not with the post-transplantation interval or the treatment protocol (Saray et al., 2004).
Up to now our case is the first reported renal transplant recipient presented with retronychia. As the onset of the retronychia was 6 years after the transplantation, no any possible etiological link between the nail changes and the transplantation or the immunosuppressive medication was confirmed. The initiation of the nail changes was completely independent from the post-transplantation time interval. The coexistence of the retronychia and renal transplantation seems to point out a coincidence rather than a possible etiological link in our case. This coincidental occurrence is not enough to argue in favor of a causal relationship between the retronychia and the renal transplantation, although the history of trauma was also questionable in our case. The involvement of only the left great toe nail rather than bilateral great toe nails also does not confirm the possible etiological link of trauma with retronychia in our case. Especially the chronic minor frictional trauma is thought to be responsible for the separation of the nail plaque seen in retronychia. However, the linear transverse line on the proximal part of her right great toe nail was remarkable for onychomadesis which points out the presence of a past traumatic process. Besides, the association of the onset of the nail disease with some medications like cyclosporine should also be considered, as some of the chemotherapeutics like bleomycin, busulphane, immunosuppressive drugs and isotretinoin may also cause nail diseases like onychomadesis, Beau’s lines, longitudinal melanoychia and periungal granulation tissue formation. On the other hand, the long-term use of the immunosuppressive drugs may have a probable cumulative toxic effect on the nail matrix tissue like in our case. As the immunosuppressive treatment of our patient was continued since transplantation, we cannot confirm the exact etiopathogenetic mechanism of the nail disease with the immunosuppressive drugs like cyclosporine or mycofenolate mofetile.
As a result retronychia is accepted as proximal nail plate ingrowth in to the proximal nail fold with multiple generations of nail plate misalignment beneath the proximal nail (De Berker et al., 2008). Retronychia should be kept in mind in the presence of a delete in nail growth and chronic paronychia, accompanied with history of trauma. Nail avulsion seems to be the best treatment to provide normal nail plaque growth and to prevent the beginning of paronychia. Almost all of the patients with retronychia reported in the literature were successfully treated with simple avulsion of the superimposed nails without any irreversible nail matrix damage. One of these five cases was first treated with only the avulsion of the distal top nail, without removing the underlying nail. Finally after the recurrence of the symptoms, the nail avulsion had to be repeated. Expectant observation of the underlying nail may sometimes lead to recurrence of the retroncyhia. If the new nail plaque growing from the proximal nail fold is shiny, viable and healthy, clinical observation may also be performed like in our case.