Research Article
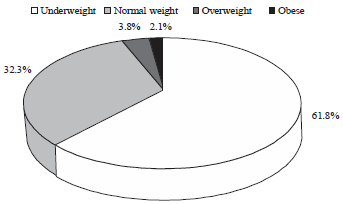
The Prevalence of Underweight, Overweight and Obesity Among Primary School Learners in the Eastern Cape Province, South Africa
Faculty of Health Sciences, University of Fort Hare, East London, South Africa
LiveDNA: 234.28637
Eunice Seekoe
Faculty of Health Sciences, University of Fort Hare, East London, South Africa
Daniel Ter Goon
Faculty of Health Sciences, University of Fort Hare, East London, South Africa
LiveDNA: 234.16603
Philemon Lyoka
Faculty of Health Sciences, University of Fort Hare, East London, South Africa
Chioneso S Marange
Faculty of Science and Agriculture, University of Fort Hare, East London, South Africa