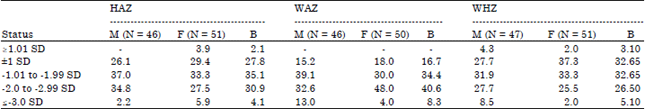Research Article
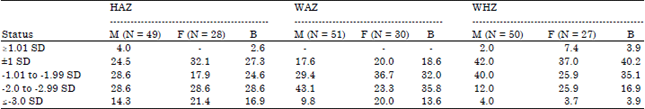
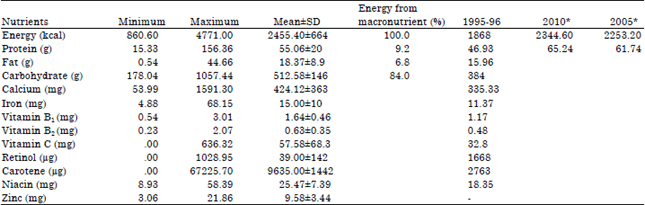
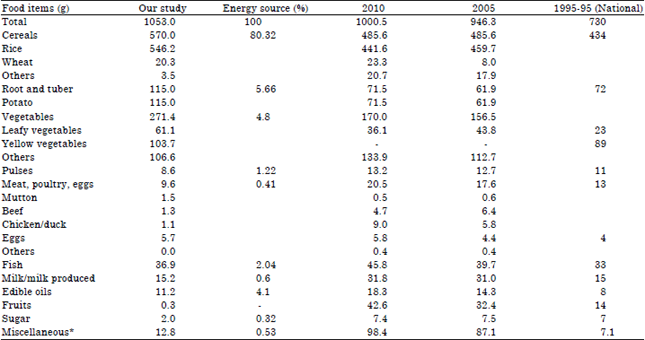
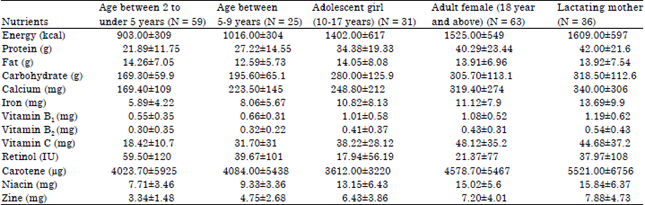
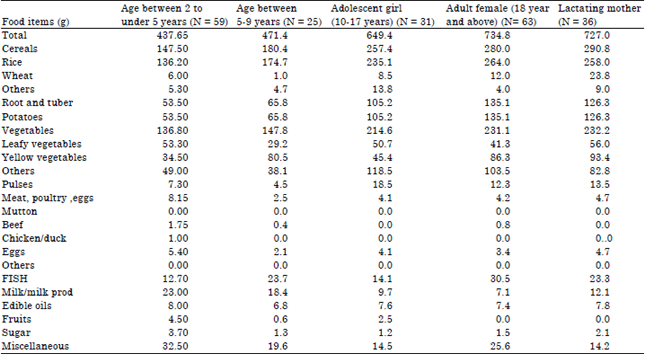
Nutritional Status, Dietary Food and Nutrient Consumption Patterns in Monga Affected Area of the Northern Part of Bangladesh
Institute of Nutrition and Food Science, University of Dhaka, Dhaka, 1000, Bangladesh
Tasmia Tasnim
Department of Nutritional Sciences Division, School of Biosciences, University of Nottingham, Sutton Bonington Campus, United Kingdom