ABSTRACT
Arteriovenous Fistulae (AVF) for hemodialysis access provide good long-term solutions for the patient with end stage renal disease. However, complications are common and require a multimodality approach to maintain their patency and continued use. In the present study, a prospective analysis was made on 15 patients who received a brachial artery-external/internal jugular polytetra-fluoro-ethylene graft for hemodialysis access. The procedure was chosen because of exhaustion of the veins in the upper extremity owing to previous multiple failures. The procedure was successful in 12 cases (80.0%), 2 cases (13.3%) needed revision (they required secondary procedures to maintain graft patency, in the form of multiple thrombolysis and venous angioplasty) and 1 case (6.7%) failed at 16 months postoperatively (she was 61 old hypertensive female who had previous 5 fistulae and developed thrombosis 12 months after intervention, which was treated with clot removal and venous angioplasty. She developed second thrombus at 16 months after intervention catastrophically deteriorated and died before secondary intervention was carried out. The brachial artery-external/internal jugular vein graft represented an important alternative procedure used for vascular access when all upper extremity veins cannot be used.
PDF Abstract XML References Citation
How to cite this article
URL: https://scialert.net/abstract/?doi=tmr.2014.53.57
INTRODUCTION
In cases with end stage renal disease, renal transplantation is the curative and most reasonable treatment, but due to long waiting list, long term hemodialysis is the main resort for End Stage Renal Disease (ESRD) patients (Mathys et al., 2011). To initiate hemodialysis, the first step is the creation of Arteriovenous (AV) fistula (Froger et al., 2005). Arteriovenous fistulae are recommended by several clinical guidelines committees as the vascular access of choice for routine outpatient hemodialysis (Fluck and Kumwenda, 2011). Unfortunately, AV fistulae had many complications, ranging from infection, aneurysm formation, stenosis or thrombosis and ultimately the formation of intimal hyperplasia (Kumbar, 2012).
Constant care to maintain vascular access patency is of great importance. However, failure of AV access is a major cause of morbidity, rising the need for advanced intervention to regain AV access patency (Vascular Access Work Group, 2006). In recent years, there is a growing increase in techniques of brachial artery to distal axillary vein graft, that allow for continued use of an arm after previous lower arm and upper arm access sites have exhausted (Teruya et al., 2009). Using these methods forms a framework for new vascular access procedures (Rosas et al., 2003).
The jugular vein is rarely used in graft procedures. Here, we presented our preliminary experience of brachial artery-jugular vein graft, using straight Polytetrafluoroethylene (PTFE) grafts to connect the brachial artery to the external or internal jugular vein under local anesthesia. It may be a good and unique alternative when there is no other possibility to regain AV access for patients on hemodialysis.
MATERIALS AND METHODS
The present study was carried out at Al-Azhar University hospital (New Damietta), during the period from June 2010 to June 2012. Fifteen patients underwent the brachial artery-jugular vein graft. All patients were examined preoperatively and underwent duplex scanning to evaluate the external and internal jugular veins for stenosis or occlusion. These included cases with multiple previously failed fistulas due to different causes, such as thrombosis, stenosis or occlusion. In all cases, the brachial-subclavian veins of both upper extremities were evaluated by doppler ultrasonography.
Surgical technique
Anesthesia: We used local anesthesia by lidocaine 2%. External jugular vein was accessed by a horizontal supraclavicular incision (Fig. 1 and 2). Internal jugular vein was used when the external jugular vein was inappropriate (inadequate in diameter (<4 mm) or had been previously used for intravenous (IV) access). Another short incision was made in the middle-third of the arm or in the antecubital region to approach the brachial artery. The PTFE 8 mm diameter (GoreTex, W.L. Gore and Associates, Inc) is anastomosed with the jugular vein using 6-0 polypropylene suture and it is driven down through a subcutaneous tunnel to the arm incision. In cases with a brachial-jugular graft, the graft was used 3 weeks after operation (Motamedi and Shirvani, 2010).
Outcome measures: Failure was defined as thrombosis not amenable to revision. Patency rate was defined as the number of grafts with satisfactory performance at the time of follow-up divided by the total number of grafts placed. Revision was defined as a graft requiring thrombectomy, angioplasty, or stent placement to maintain adequate flow rates (Teruya et al., 2009).
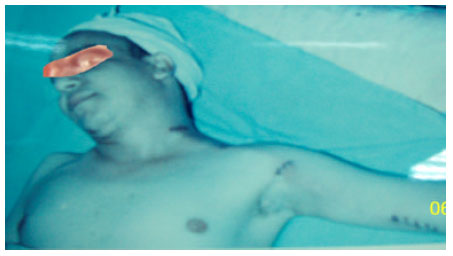 | |
| Fig. 1: | Postoperative mark of incisions made to reach the external jugular vein and the brachial artery |
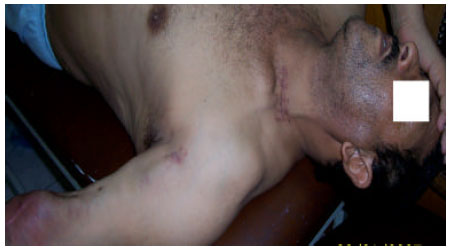 | |
| Fig. 2: | Postoperative mark of incisions made to reach the external jugular vein and the brachial artery with myxomatous degeneration at the site of the brachial artery |
RESULTS
The present study included 15 cases; 8 of them (53.3%) were males and 7 (46.7%) were females; their age ranged from 38 to 63 years with a mean of 53.33±7.05; the cause of renal failure was diabetic nephropathy in 7 cases (46.7%), hypertensive nephropathy in 6 cases (40.0%); polycystic kidney in two cases (13.3%); the number of previous fistulae ranged from 3 to 6 with a mean of 4.26±1.03; the mean follow up duration ranged from 12 to 22 months with follow up time of 16.93±2.91 months. The procedure was primary successful in 12 cases (80.0%), two cases (13.3%) needed revision (they required secondary procedures to maintain graft patency, in the form of multiple thrombolysis and venous angioplasty) and one case (6.7%) failed at 16 months postoperatively (she was 61 old hypertensive female who had previous 5 fistulae and developed thrombosis 12 months after intervention, which was treated with clot removal. She developed second thrombus at 16 months after intervention (graft) catastrophically deteriorated and died before secondary intervention was carried out (Table 1).
DISCUSSIONS
The End Stage Renal Disease (ESRD) is continued to increase worldwide. While waiting for a renal transplantation or inability to perform transplantation, patients with ESRD are treated hemodialysis (HD) which requires efficient vascular access and arteriovenous fistula (AVF) is the preferred form of vascular access, as it had low rate of complications (Roy-Chaudhury et al., 2005). However, thrombosis of AVF remains a major cause of morbidity in these patients and it is the most common cause of access failure (Danis et al., 2009; Montagnana et al., 2011). In addition, fistulae lost its proper function due to periodic hemodialysis and ultimately the formation of intimal hyperplasia. In this situation, patients had developed various complications such as upper extremity edema, venous hypertension, venous or graft thrombosis or stricture with their previous fistulas or grafts and had no other option available for vascular access (Romero et al., 1986). In this situation, regaining patency or vascular access is of utmost importance. This can be achieved by brachial artery-external/internal jugular vein graft placement.
In the present study we presented our preliminary experience for brachial artery-jugular vein graft as a convenient substitute in cases with exhausted AFV in their upper limb. Results of the present study yielded 80% primary success rate at mean of 16.93±2.91 months of follow up.
| Table 1: | Results of the studied cases |
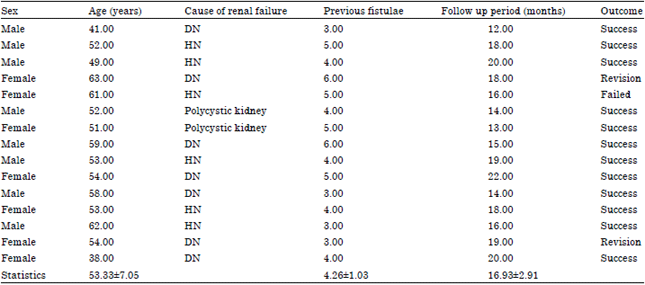 | |
| DN: Diabetic nephropathy; HN: Hypertensive nephropathy | |
These results are comparable to those reported by Motamedi and Shirvani (2010) who reported a success rate of 81.8% (9 cases out of 11 cases). They added, this technique not only bypasses the stenotic or occluded axillary-subclavian vein, but also provides a longer conduit for future vascular access. Subsequently, this allows better needle insertion spacing for HD and decreased the risk of pseudoaneurysm formation or graft damage. It also has the advantage of being technically easier to use the external instead of the internal jugular vein for venous drainage of the graft and obviously the internal jugular vein can be saved for later use when the external jugular vein ultimately fails.
In addition, our results are comparable to those reported by Teruya et al. (2009) who reported that, the average time of follow-up was 16 months, with a median follow-up of 18 months (range 9-22). The overall patency rate was 78%.
Finally, Shibutani et al. (2013) performed Transposed Brachiobasilic Arteriovenous (TBBAVF) in 24 patients. The primary patency rates at one and two years were 89.7 and 69.0%, respectively. The secondary patency rates at one and two years were 95.7 and 73.6%, respectively. TBBAVF has good primary and secondary patency rates with few severe complications.
In the present work, two cases had been needed revision due to thrombosis and both cases were diabetic; and the relation between diabetes and complications may be present. In study done by Tuka et al. (2006), 48 cases out of 106 cases were diabetic. With diabetes, higher wall shear rate in feeding artery was reported in diabetic patients and vascular access creation. This shear could be relevant in the pathogenesis of AVF thrombosis with subsequent lower patency rates in diabetic patients. In addition, Resic et al. (2005) conducted a study to estimate risk factors for AVF adequacy in 40 patients. Their results revealed that, predictors of AVF malfunction were age, diabetes and overweight. However, other studies did not find this correlation between diabetes and AVF malfunction and complications (Murphy and Nicholson, 2002; Lin et al., 1998).
One of the limiting steps in the present study is the small sample size; it can be attributed to the fact that, I included cases with exhausted AVF, aiming to provide an alternative to continue HD. Additional limiting step is the observational nature of the present study, but we would not be able to include cases for control or comparison as the present study provided our preliminary experience. In the future, this limitation can be avoided.
In short, results of the present study provided our preliminary results of brachial artery-jugular vein graft for exhausted AVF. It can be concluded that, the brachial artery-external/internal jugular vein graft represented an important alternative procedure used for vascular access when all upper extremity veins, cannot be used.
REFERENCES
- Danis, R., S. Ozmen, D. Akin, S. Batun and S. Kahvecioglu et al., 2009. Thrombophilias and arteriovenous fistula dysfunction in maintenance hemodialysis. J. Thromb. Thrombolysis, 27: 307-315.
CrossRef - Fluck, R. and M. Kumwenda, 2011. Renal association clinical practice guideline on vascular access for haemodialysis. Nephron. Clin. Pract., 118: c225-c240.
CrossRefDirect Link - Froger, C.L., L.E. Duijm, Y.S. Liem, A.V. Tielbeek and A.B. Donkers-van Rossum et al., 2005. Stenosis detection with MR angiography and digital subtraction angiography in dysfunctional hemodialysis access fistulas and grafts. Radiology, 234: 284-291.
PubMed - Kumbar, L., 2012. Complications of arteriovenous fistulae: Beyond venous stenosis. Adv. Chronic Kidney Dis., 19: 195-201.
CrossRef - Lin, S.L., C.H. Huang, H.S. Chen, W.A. Hsu, C.J. Yen and T.S. Yen, 1998. Effects of age and diabetes on blood flow rate and primary outcome of newly created hemodialysis arteriovenous fistulas. Am. J. Nephrol., 18: 96-100.
Direct Link - Mathys, C., D. Blondin, H.J. Wittsack, F.R. Miese and K. Rybacki et al., 2011. T2' imaging of native kidneys and renal allografts-a feasibility study. Fortschr Rontgenstr, 183: 112-119.
CrossRefDirect Link - Montagnana, M., T. Meschi, L. Borghi and G. Lippi, 2011. Thrombosis and occlusion of vascular access in hemodialyzed patients. Semin Thromb Hemost, 37: 946-954.
CrossRef - Murphy, G.J. and M.L. Nicholson, 2002. Autogeneous elbow fistulas: The effect of diabetes mellitus on maturation, patency and complication rates. Eur. J. Vasc. Endovasc. Surg., 23: 452-457.
CrossRef - Vascular Access Work Group, 2006. Clinical practice guidelines for vascular access. Am. J. Kidney Dis., 48: S248-S273.
CrossRef - Romero, A., J.R. Polo, E. Garcia Morato, J.L. Garcia Sabrido, A. Quintans and J.P. Ferreiroa, 1986. Salvage of angioaccess after late thrombosis of radiocephalic fistulas for hemodialysis. Int. Surg., 71: 122-124.
PubMed - Rosas, S.E., M. Joffe, J.E. Burns, J. Knauss, K. Brayman and H.I. Feldman, 2003. Determinants of successful synthetic hemodialysis vascular access graft placement. J. Vasc. Surg., 37: 1036-1042.
CrossRefDirect Link - Roy-Chaudhury, P., B.S. Kelly, M. Melhem, J. Zhang and J. Li et al., 2005. Vascular access in hemodialysis: Issues, management and emerging concepts. Cardiol. Clin., 23: 249-273.
CrossRef - Shibutani, S., H. Obara, S. Ono and Y. Kitagawa, 2013. Transposed brachiobasilic arteriovenous fistula. Ann. Vasc. Dis., 6: 164-168.
Direct Link - Teruya, T.H., D. Schaeffer, A.M. Abou-Zamzam and C. Bianchi, 2009. Arteriovenous graft with outflow in the proximal axillary vein. Ann. Vasc. Surg., 23: 95-98.
CrossRefDirect Link - Tuka, V., M. Slavikova, J. Svobodova and J. Malik, 2006. Diabetes and distal access location are associated with higher wall shear rate in feeding artery of PTFE grafts. Nephrol. Dial. Trans., 21: 2821-2824.
PubMed - Motamedi, A.R. and A. Shirvani, 2010. Brachial artery-jugular vein jump graft: a salvage procedure for vascular access. Ann. Vasc. Surg., 24: 1147-1149.
CrossRefPubMedDirect Link








