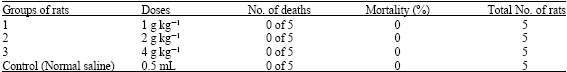Research Article
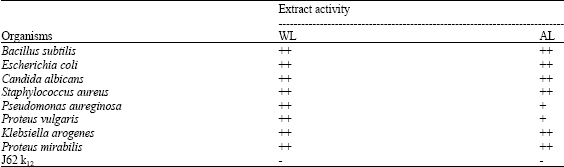
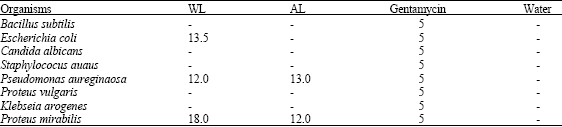
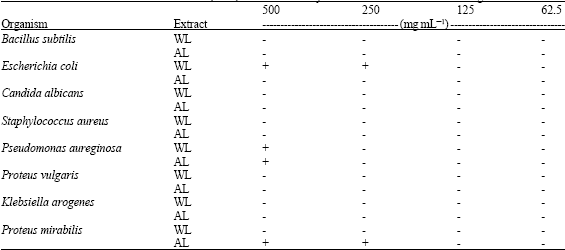
Preliminary Phytochemistry, Antimicrobial Properties and Acute Toxicity of Stachytarpheta jamaicensis (L.) Vahl. Leaves
Department of Botany, University of Benin, P.M.B. 1154, Benin City, Nigeria
E.K.I. Omogbai
Department of Pharmacology, University of Benin, P.M.B. 1154, Benin City, Nigeria
G.E. Aghimien
Department of Botany, University of Benin, P.M.B. 1154, Benin City, Nigeria
F. Amaechina
Department of Pharmacology, University of Benin, P.M.B. 1154, Benin City, Nigeria
O. Timothy
Department of Botany, University of Benin, P.M.B. 1154, Benin City, Nigeria
S.E. Omonigho
Department of Microbiology, University of Benin, P.M.B. 1154, Benin City, Nigeria