Research Article
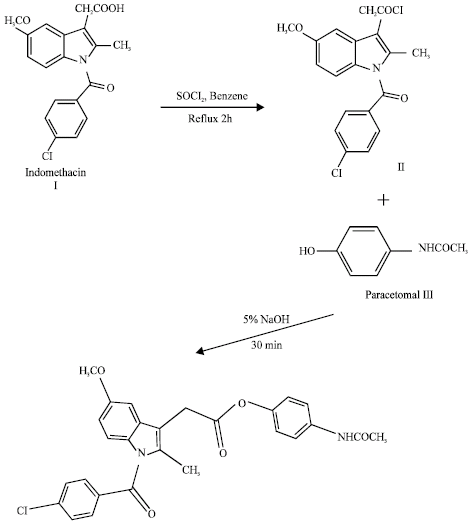
Synthesis and Physicochemical Characterization of Mutual Prodrug of Indomethacin
School of Pharmaceutical Sciences, Rajiv Gandhi Proudyogiki Vishwavidhyalaya, Airport Bypass Road, Gaudhi Nagar, Bhopal-462036, Madhya Pradesh, India
N.S. Hari Narayana Moorthy
School of Pharmaceutical Sciences, Rajiv Gandhi Proudyogiki Vishwavidhyalaya, Airport Bypass Road, Gaudhi Nagar, Bhopal-462036, Madhya Pradesh, India