Research Article
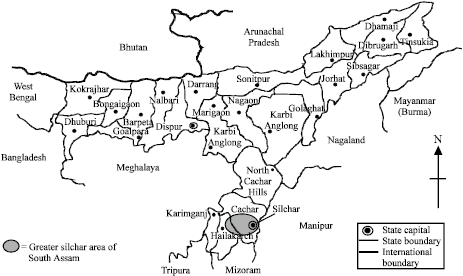
Pollen, Fungus and House Dust Mites Survey at the Residence of 90 Allergic Patients in Greater Silchar Area of Assam, India
Microbiology Laboratory, Centre for Biodiversity, Faculty of Life Science, Rajiv Gandhi University, Rono Hills, Itanagar-791 112, Arunachal Pradesh, India
B.K. Dutta
Deptartment of Ecology and Environmental Science, Assam University, Silchar, Assam-788011, India
A.B. Singh
Institute of Genomics and Integrative Biology, CSIR, Mall Road, Delhi-110 007, India