ABSTRACT
Childhood obesity is escalating rapidly, both in industrialized and developing countries. It will emerge as a potential public health burden faced by the developing countries in the near future. In children, Non Alcoholic Fatty Liver Disease (NAFLD) is mainly associated with obesity and metabolic syndrome and is therefore considered as a metabolic complication of obesity. NAFLD comprises of a range of chronic liver diseases from simple steatosis, steatohepatitis and cirrhosis with liver failure. Since the prevalence of obesity in children is increasing, the prevalence of NAFLD in children is expected to increase as well. Prevention of obesity and identification of children with an increased risk of NAFLD are important steps in preventing irreversible liver damage. This prospective study was carried out in the primary schools of Dera Ismail Khan History City having mixed population. Clinical examination of the children excluded those suffering from chronic health ailments. History from the parents excluded the intake of hepatotoxic drugs. Body mass status of child was determined according to World Health Organization s' criteria and Centers for Disease Control and Prevention (CDC)'s gender and age specific growth charts. Randomly selected normal weight and obese children have undergone abdominal ultrasound examination to confirm or rule out hepatic steatosis (Fatty Liver) by detecting the alteration in ultrasound/hyperechogenicity of the organ. Randomly selected children (normal weight and obese) among the 1336 school going children were subjected to ultrasound examination, comprising of 55 boys (59.13%) and 38 (40.86%) girls. 67 (72.04%) were obese and 26 (27.95) as normal weights. Hepatic ultrasound alterations/hyperechogenic liver was found in 7 (7.52%) obese boys. None of the obese girls and normal weight children was found to exhibit any alteration in ultrasound findings.
PDF Abstract XML References Citation
How to cite this article
DOI: 10.3923/pjn.2009.797.799
URL: https://scialert.net/abstract/?doi=pjn.2009.797.799
INTRODUCTION
Fatty liver or hepatic steatosis is a pathological condition characterized by abnormal excessive/extensive accumulation of lipids mainly triglyceride in liver. When accumulation of lipid becomes chronic; it induces pressure effect on the architecture of liver; produces inflammation, fibrosis and cirrhosis of liver, leading to a chronic condition known as Non-alcoholic Steatohepatitis (NASH). Simple steatosis (fatty liver), which rarely has any sequelae, is also a part of the condition termed as non alcoholic fatty liver decrease (NAFLD) (Angulo and Lindor, 2001 and Angulo et al., 1999). Hepatic steatosis has increased markedly in all segments of the population and now extends to children. The rising prevalence of obesity and type 2-diabetes in the population is likely to be responsible for the increasing number of individuals with hepatic steatosis (Flegal et al., 2001 and Rashid and Roberts, 2000). Fatty liver is associated with two main types. The first type is associated with raised levels of plasma Free Fatty Acids (FFAs) resulting from lipolysis of the extra hepatic tissues (muscles and adipose tissue) through the action of lipoprotein lipase. Liver is unable to produce VLDL due to the heavy influx of FFAs. FFAs are esterified to produce triglyceride that accumulates in liver causing fatty liver. This commonly occurs in children taking high fat diet, obesity, uncontrolled diabetes mellitus and starvation. The second type is due to the metabolic block in the production of plasma lipoproteins, thus allowing the triglyceride to accumulate. This block may be in the synthesis of apolipoproteins, synthesis of lipoproteins from lipids and apolipoproteins, failure in the provision of phospholipids for lipoproteins and failure in the secretary mechanism itself (Peter and Kathleen, 2003). Certain medications are known to produce fatty liver. These include glucocorticoids, synthetic estrogens. Calcium channel blockers, methotraxate, tetracycline, valporic acid, cocaine, Zidovudine (AZT) and Didianosines (ddL) (Angulo, 2002). Petroleum and organic solvents in cigarette smoke, paints, automobile exhaust, pesticides, air fresheners and solvents used for cleaning and dry cleaning are also included in this category (Cotrim et al., 1999). Majority of the patients with hepatic steatosis are asymptomatic at the time of diagnosis. They may complain of discomfort in the right upper quadrant of abdomen, fatigue and malaise. Hepatomegaly may occur but does not accompany symptoms (Kumar and Malet, 2000).
MATERIALS AND METHODS
The present study was carried out to evaluate the school children (obese as well as healthy/normal weights), 6-11 years for fatty liver or hepatic steatosis. 93 children, 67 (72.04%) obese and 26 (27.95%) as normal/healthy weights were involved in this study. 55 (59.13%) were boys and 38 (40.86%) as girls. They were amongst the school children (1336) examined for this purpose and belong to the different schools of Dera Ismail Khan NWFP, Pakistan. All of them have undergone thorough medical examination to exclude those suffering from chronic health diseases. Body mass status of each child (Obese and healthy weights) was calculated through World Health Organization and Centers for Disease Control and Prevention (CDC)’s age and gender specific growth charts 2-20 years. Those falling between 5th to less than 85th BMI-for-age percentile were considered as normal/healthy weights and those at and above 95th percentile (BMI-for-age %) as obese compared with CDC reference population of the same age and gender. Hepatic steatosis or fatty liver in children was evaluated by imaging through ultra- Sonography. It does not differentiate fatty liver (Hepatic steatosis), steatohepatitis and steatohepatitis with fibrosis. Computed tomography is more specific but is expensive. Ultra-Sonography is slightly more sensitive; simple, cheap, easily available and requires no preparations. Children were usually accompanied by their parents after school timings to make the atmosphere friendlier. They were briefed about this harmless and non-invasive procedure. Abdominal ultra- Sonography also explored the other intra abdominal organs especially spleen, kidneys, urinary bladder, intestines and lymph nodes. Reproduction organs, however, were not imaged. Hyperechogenic liver on ultra-Sonography was declared as fatty liver.
RESULTS
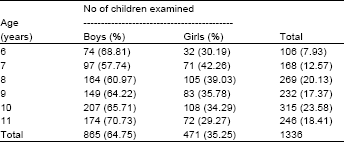
1336 school going children were involved in this study with 865 (64.74%) boys and 471 (35.25%) as girls. Children were divided into six groups according to their age and gender. Number and percentage of either gender or age is given in Table 1.
Randomly selected 93 children amongst 1336 local pediatric population were subjected to abdominal ultra sonography. Body mass status and gender of these children is shown in Table 2.
There were 55 (59.13%) boys and 38 (40.86%) girls. Obese were 67 (72.04%) and normal weights as 26 (27.95%).
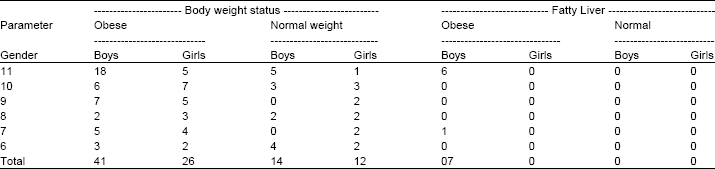
Table 3 shows the distribution of the sample according to age group and gender. It also reveals that 7 (7.52%) of obese children (boys) were having hyperechogenic / fatty liver of normal size and shape.
Ultra sonography of normal/healthy weight boys and girls revealed normal echogenic liver with no change in size and shape. It is remarkable to note that all the children with fatty liver were boys. Girls (normal weight as well as obese) were not having fatty liver. Majority (6 of 7) obese boys were of 11 years except one of 7 years.
| Table 1: | Number of students examined according to age and gender |
 | |
| Table 2: | Body mass status and gender |
 | |
DISCUSSION
The Present study was carried out to determine the magnitude of obesity and fatty liver among the children in the local pediatric population. Fatty liver, was restricted to the boys of 11 years in this study which is against common finding that there is no gender and age difference among the individuals (Angulo et al., 1999). The reason for this discrepancy is unexplainable The percentage of fatty liver was 7.52% among the children (93) subjected to ultrasound examination. Hepatic steatosis in the present study can be compared with the similar findings in Iran (Seyed et al., 2008) where fatty liver was diagnosed by ultrasound, is 7.1% among 996 school children reflecting the similar conditions in both the countries. Ours findings can be compared with the reports released from the studies performed in tertiary medical centers of India that NAFLD in obese children was of the range from 20-77%. The conditions in densely populated cities in developing countries may have the same conditions as in industrial countries (Prashant et al., 2007). In another developing country like Brazil (Suano-de et al., 2008), hepatic steatosis in obese children was found to be 56.5 and 48.9% in control group of children with an average age of 8.6 years. Similar studies in Turkey (Tuba et al., 2008) reported hepatic steatosis as 52.4% in obese children. Fatty liver is reported 44% in obese children of Italy in a sample of 280 obese ones (Sartorio et al., 2007). Prevalence of fatty liver in children and adolescents, adjusted for age, gender, race and ethnicity is estimated to be 9.6% in the United States of America. It differs significantly according to race and ethnicity. Fatty liver in Asians is 10.2%, Blacks 1.5%, Hispanics 11.8% and Whites as 8.6%.The highest rate was seen in obese children as 38% out of a total sample of 784 children with ages of 2-19 years who had autopsy from 1993-2003 (Jeffery et al., 2006).
| Table 3: | Body weight status, age, gender and ultra sonographic findings |
 | |
Conclusion: Prevention of obesity and identification of children with an increased risk of hepatic steatosis are important steps in preventing irreversible liver damage. Ultra Sonography is a useful tool in identifying and monitoring the process. Lifestyle changes aimed at improving insulin sensitivity through healthy food and sufficient physical activity are essential in the treatment of non alcoholic fatty liver disease. Pharmacological treatment may have additional value.
REFERENCES
- Angulo, P. and K.D. Lindor, 2001. Insulin resistance and mitochondrial abnormalities in NASH. Gastroenterology, 120: 1281-1285.
Direct Link - Angulo, P., J.C. Keach, K.P. Batts and K.D. Lindor, 1999. Independent predictors of liver fibrosis in patients with nonalcoholic steatohepatitis. Hepatalogy, 30: 1356-1362.
Direct Link - Angulo, P., 2002. Nonalcoholic fatty liver disease. N. Engl. J. Med., 346: 1221-1231.
CrossRefDirect Link - Cotrim, H.P., Z.A. Andrade and R. Parana, 1999. Non alcoholic steatohepatitis, a toxic liver disease in industrial workers. Liver, 19: 299-304.
Direct Link - Jeffery, B., R.D. Schwimmer, E.L. Joel, S. Christina and B. Synthia, 2006. Prevalence of fatty liver disease in children and adolescents. Pediatrics, 118: 1388-1393.
Direct Link - Prashant, M., K.D. Manoga and K.A. Narendra, 2007. Non alcoholic fatty liver disease and childhood obesity. Int. J. Pediatrics, 74: 401-408.
CrossRef - Sartorio, A., A. Delcoil, M. Agostef, S. Bellenteni, C. Tiribelli and G. Bedogni, 2007. Predictors of non alcoholic fatty liver disease in obese children. Euro. J. Clin. Nutr., 61: 877-883.
Direct Link - Tuba, F.E., M.O. Camurdan, O.O. Suna, B. Aysun and D. Buket, 2008. Factors related to nonalcoholic fatty liver disease in obese children. Turkish J. Gastroenterol., 19: 85-91.
Direct Link








