Research Article
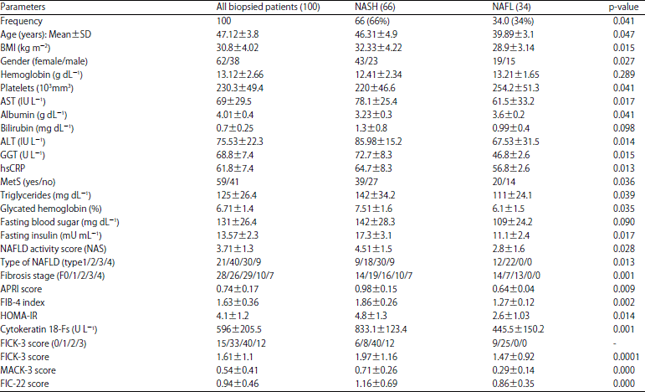
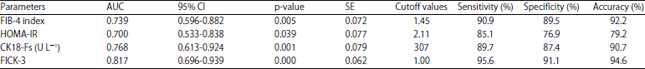
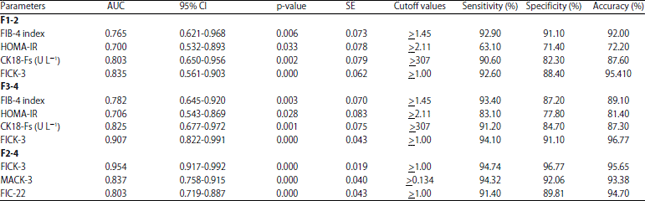
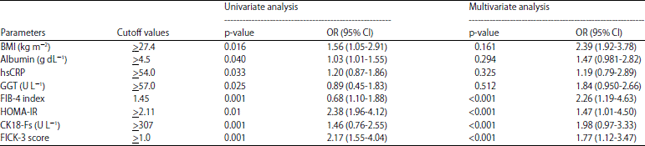
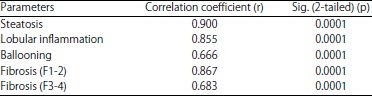
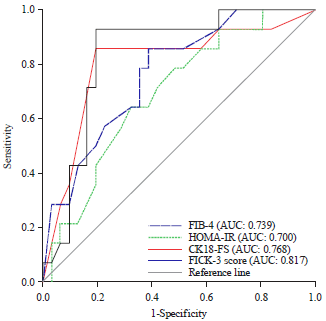
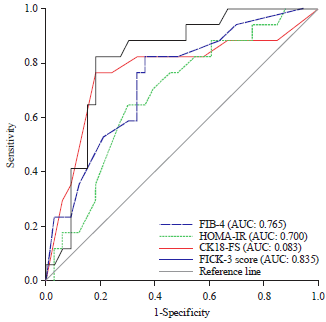
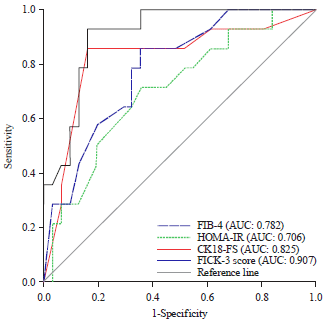
FICK-3 Score Combining Fibrosis-4, Insulin Resistance and Cytokeratin-18 in Predicting Non-alcoholic Steatohepatitis in NAFLD Egyptian Patients
Department of Internal Medicine, Gastroenterology, Hepatology and Endoscopy Unit, Faculty of Medicine, Mansoura University, Egypt
LiveDNA: 20.15383
Nesreen Moustafa Omar
Department of Histology and Cell Biology, Faculty of Medicine, Mansoura University, Egypt
Soad Amin Mohammed
Department of Microbiology, Faculty of Pharmacy, Al-Azhar University, Egypt
Ahmed Mohammed Amin
Medical Student, Faculty of Medicine, Mansoura University, Egypt
Doaa Farouk Gad
Department of Internal Medicine, Gastroenterology, Hepatology and Endoscopy Unit, Faculty of Medicine, Mansoura University, Egypt