Research Article
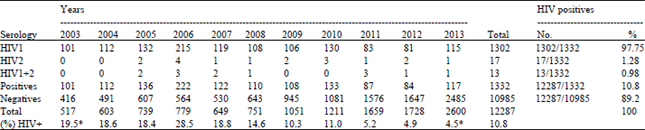
A Decade of Follow-up and Therapeutic Drug Monitoring in HIV-2 Immunocompromised Patients at St Camille and General Lamizana Military Medical Centers, Burkina Faso, West Africa
Pietro Annigoni Biomolecular Research Center (CERBA) (LABIOGENE), University of Ouagadougou, Burkina Faso
S. T. Soubeiga
Pietro Annigoni Biomolecular Research Center (CERBA) (LABIOGENE), University of Ouagadougou, Burkina Faso
F. Bationo
Epidemiology and Bio statistic Pole, Clinical and Experimental Research Institute (IREC), School of Public Health, Catholic University of Louvain, Brussels, Belgium
T. R. Compaore
Pietro Annigoni Biomolecular Research Center (CERBA) (LABIOGENE), University of Ouagadougou, Burkina Faso
T. M. Zohoncon
Pietro Annigoni Biomolecular Research Center (CERBA) (LABIOGENE), University of Ouagadougou, Burkina Faso
G. N. Diatto
General Sangoule Lamizana Military Medical Center, Clinical Laboratory Unit, Ministry of Defence and Veterans Affairs, Ouagadougou, Burkina Faso, Healthcare Unit Training, (UFR-SDS), University of Ouagadougou, Ouagadougou, Burkina Faso
P. Ouedraogo
St Camille Medical Center, 01 BP 364, Ouagadougou
V. Pietra
Pietro Annigoni Biomolecular Research Center (CERBA) (LABIOGENE), University of Ouagadougou, Burkina Faso
B. M. Nagalo
Endicott College, School of Arts and Sciences, Beverly, Massachusetts, USA
C. Bisseye
University of Sciences and Techniques of Masuku, Franceville, Gabon
R. Ouedraogo Traore
Charles de Gaulle University Pediatric Teaching Hospital, Ouagadougou, Burkina Faso
J. Simpore
St Camille Medical Center, 01 BP 364, Ouagadougou