Research Article
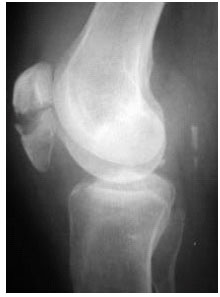
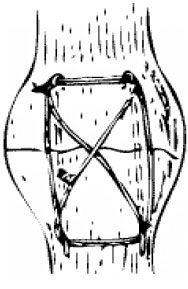
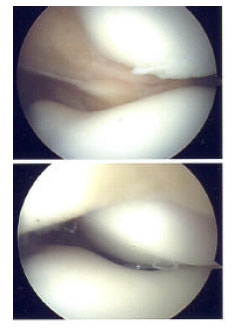
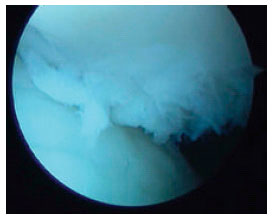
A Study of the Long Term Effects of Anatomical Open Reduction of Patella on Patellofemoral Articular Cartilage in follow up Arthroscopy
Department of Orthopedics, Ward of Orthopedics, Besat Hospital, Hamadan University of Medical Sciences, Tabriz, Hamadan, Iran
Khashayar Davoudpour
Department of Orthopedics, Ward of Orthopedics, Besat Hospital, Hamadan University of Medical Sciences, Tabriz, Hamadan, Iran
Gholamreza Ghorbani Amjad
Department of Orthopedics, Ward of Orthopedics, Besat Hospital, Hamadan University of Medical Sciences, Tabriz, Hamadan, Iran