Research Article
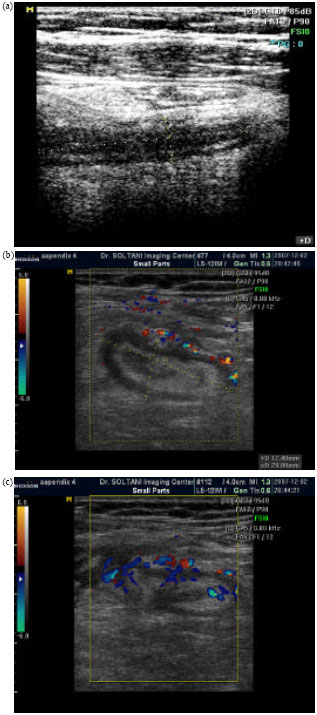
Accuracy of Sonography in Diagnosis of Acute Appendicitis Running
Department of Radiology, Golestan Hospital, Ahvaz Jundishapur University of Medical Sciences, Ahwaz, Iran
M. Sametzadeh
Department of Radiology, Golestan Hospital, Ahvaz Jundishapur University of Medical Sciences, Ahwaz, Iran
R. Kamankesh
Department of Radiology, Golestan Hospital, Ahvaz Jundishapur University of Medical Sciences, Ahwaz, Iran
F. Rahim
Physiology Research Center, Ahvaz Jundishapur University of Medical Sciences, Ahwaz, Iran