Research Article
Outcomes of Coronary Artery Bypass Grafting in Patients with a History of Opiate Use
Department of Cardiothoracic Surgery, Shahid Madani Hospital, Tabriz University of Medical Sciences, Tabriz, Iran
Although Myocardial Infarction (MI) mainly occurs in patients older than 45, young men or women can suffer MI. Fortunately, its incidence is not common in patients younger than 45 years. However, the disease carries a significant morbidity, psychological effects and financial constraints for the person and the family when it occurs at a young age. The causes of MI among patients aged less than 45 can be divided into four groups: 1-atheromatous coronary artery disease; 2-non-atheromatous coronary artery disease; 3-hypercoagulable states and 4-MI related to substance misuse. There is a considerable overlap between all the groups (Abdollahi et al., 2007; Egred et al., 2005).
Opiate abuse is a major problem for every society including our country. It is estimated that the prevalence of opiate addiction has grown up by three folds for the past 20 years in Iran and now it is presumed to be 2-2.8% according to official address. It is surprisingly reported that the rate of opiate use is higher in patients undergoing Coronary Artery Bypass Grafting (CABG). The prevalence of opium addiction in CABG patients is relatively high and the majority of addicted patients are on this belief that opiates have positive effects on improvement of their chest pain and cardiovascular function (Abdollahi et al., 2007). There is a misconception among people that opioids may prevent or have ameliorating effects in the occurrence of cardiovascular diseases (Sadr-Bafghi et al., 2005). Because the effects of opioids on chest pain are palliative, the necessity of education for correction of this idea has been identified (Abdollahi et al., 2007).
This study aimed at evaluating the outcome of CABG in patients with a history of opiate use.
The descriptive-analytic and prospective study was performed on 200 consecutive patients underwent Coronary Artery Bypass Graft (CABG) in Tabriz Shahid Madani Heart Center from 2006 to 2007. The patients were classified in three groups: 1-with previous history of opiate use (oral or parentral), 2-active opiate users (oral or parentral) before or after CABG and 3-without any history of opiate use. The state of opiate use was determined by observation and laboratory test in admission. The patients were followed up for 6 months and readmission for cardiovascular accidents, acceptance of medical treatment and nutritional and physical activity recommendations and use of opiate or cigarette was assessed and recorded. The local ethics committee approved the study and all participants gave informed written consent. The patients were confirmed that their information remain secret. Exclusion criteria were death, migration and non agreement for participation in the study.
Age, sex, hypertension history, smoking, Ejection Fraction (EF) measured by echocardiography before and after CABG, hospital stay, postoperative complications, NYHA function class, analgesic or NSAID use were recorded.
Statistical analysis: The collected data were expressed as percentage and Mean±SD. Continuous (quantitative) variables were compared by Student t-test (Independent samples) or one way ANOVA. Categorical (qualitative) variables were compared by contingency tables and Chi-square test or Fisher’s exact test. A p-value ≤0.05 was considered statistically significant.
Out of 200 studied patients, 177 (88.5%) had no history of opiate use (group N) and 23 (11.5%) had used opiate (group P), of which 9 had the previous history of opiate use (group A) and 14 were active users (group B). The opiate type was Opium (19 cases), Extract or Sap (3 cases) and Heroin (1 case). The route of opiate use was inhalation in 14 cases (60.87%), oral in 8 cases (34.87%) and injection in one case (4.35%). Patients’ characteristics and findings in each group have been compared in Table 1.
Postoperative complications were pericardial effusion (5 cases), pleural effusion (4 cases), ventricular or supraventricular arrhythmia (4 cases). The patients obey from physician recommendations after CABG have shown in Table 2. To some extant obey and No obey medical (p<0.001), nutritional (p = 0.004) and activity (p = 0.001) recommendations after CABG were significantly more in opiate users.
Multivariate analysis for finding independent factors effective on postoperative prognosis showed that no obey medical (p = 0.045), nutritional (p = 0.008) and activity (p = 0.006) recommendations after CABG and also, re-hospitalization for cardiovascular problems after CABG (p = 0.001) was significantly more in opiate users than nonuser patients.
| Table 1: | Comparison of patients’ characteristics and findings in each group |
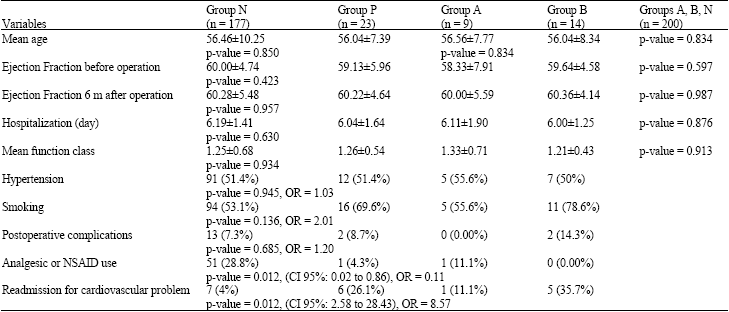 | |
| Table 2: | The patients obey from physician recommendations after CABG |
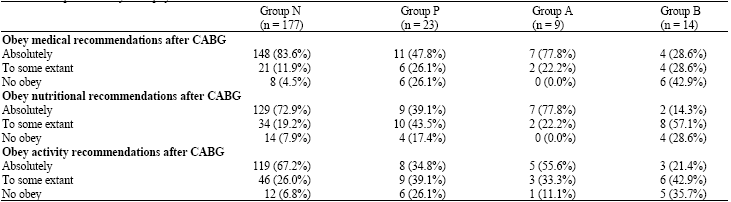 | |
Comparative analysis of groups A and N showed that there was not significant difference between two groups about age (p = 0.581), sex (p = 0.450), diet (p = 0.148), hypertension history (p = 1), smoking (p = 1), ejection fraction before (p = 0.323) and after (p = 0.880) CABG, hospitalization period (p = 0.860), functional class (p = 0.716), postoperative complications (p = 1), using analgesic or NSAIDs after CABG (p = 0.449) and re-hospitalization for cardiovascular problems (p = 0.333).
Comparative analysis of groups N and B showed that there was not significant difference between two groups about age (p = 0.849), diet (p = 0.257), hypertension history (p = 0.919), smoking (p = 0.065), ejection fraction before (p = 0.786) and after (p = 0.960) CABG, hospitalization period (p = 0.617), functional class (p = 0.853), postoperative complications (p = 0.302). The number of males (p = 0.0.013) and re-hospitalization for cardiovascular problems (p = 0.001) was significantly more in group B and using analgesic or NSAIDs after CABG (p = 0.023) was significantly more in group N.
Comparative analysis of groups A and B showed that there was not significant difference between two groups about age (p = 0.452), sex (p = 0.391), diet (p = 0.431), hypertension history (p = 1), smoking (p = 0.363), ejection fraction before (p = 0.619) and after (p = 0.862) CABG, hospitalization period (p = 0.878), functional class (p = 0.618), postoperative complications (p = 0.502) and re-hospitalization for cardiovascular problems (p = 0.340).
According to some earlier reports prevalence of addiction estimated to be 3% in Iran. One of the most important key points about addiction is the identification of predisposing factors for starting substance use (Abdollahi et al., 2007). In this study, the frequency of opiate use in patients undergoing CABG was 11.5% of which 60.87% were active users. Abdollahi et al. (2007) intended a cross-sectional analytical study to evaluate situation of opiate dependency among 1329 CABG patients in Yazd Afshar hospital. In addition 131 patients (9.9%) containing 127 men (98.9%) and 4 women (1.1%) were opium dependent.
Sadr-Bafghi et al. (2005) evaluated 556 consecutive male patients hospitalized due to acute Myocardial Infarction (MI) in city of Yazd, from May 2000 to October 2001 and compared the characteristics of opium addicts to non opium users. Prevalence of opium addiction in MI patients was 19% in comparison with 2-2.8% in general population. There were not any differences in prevalence of traditional risk factors between opium users and non-users. Overall, in-hospital mortality was 18.6% among opium users and 6.2% among non-opium users.
Misra et al. (2003) conducted a study on 161 patients undergoing CABG. The frequency of opiate use in patients undergoing CABG was 9.94% of which 62.5% were active users. They suggested that current illicit drug use is a significant predictor of cardiovascular complications in the first 6 months after coronary artery bypass grafting. In this study, there was not significant difference between age of patients with and without previous history of opiate abuse. In study of Misra et al. (2003) active abusers was younger than other patients. However, in Abdollahi et al. (2007) study, opiate abusers were significantly older than other patients. Further studies are needed for obtaining definite results.
In this study, the rate of readmission for cardiovascular problems in 6 months follow up was significantly more in patients with previous history of opiate use (active users). This is in compatible with Misra et al. (2003) study in which the rate of readmission for cardiovascular problems in 6 months follow up was 60% in active users and 7% in others.
It seems that opium addiction may work as a risk factor in cardiovascular disease (Sadr-Bafghi et al., 2005). Herning et al. (2008) suggested that EEG, cerebral blood flow velocity, cardiovascular and thyroid function alterations in marijuana abuser with an extended period of use.
Opioids inhibit the autonomic nervous system. Opioids are known to inhibit the release of catecholamines both in vitro and in vivo resulting in decreased effector responses to nerve stimulation. In fact, adrenergic second messenger stimulation increased enkephalin production in isolated cardiomyocytes (Barron, 2000). Opiates inhibit GnRH release by affecting on hypothalamus, with subsequent decrease of LH and FSH and ultimately serum testosterone (Barron, 2000; Yue et al., 1995; Webb et al., 1999). Both hyperestrogenemia and hypotestosteronemia have been reported in association with Myocardial Infarction (MI) in men. It was earlier observed that the serum testosterone concentration correlated negatively with the degree of Coronary Artery Disease (CAD) in men who had never had a known MI (Phillips et al., 1996). Until menopause, women appear to be protected from coronary heart disease. Evidence suggests that estrogen may play a role in the protection of the cardiovascular system by exerting a beneficial effect on risk factors such as cholesterol metabolism and by a direct effect on the coronary arteries (Yue et al., 1995; Webb et al., 1999).
Cannabis is a common substance of drug abuse among the young adults because of its euphoric and addictive effects. The pathophysiological effects of cannabis smoking and its relation to adverse cardiovascular events are well known (Dwivedi et al., 2008). Cannabis has cardiovascular effects and complications (Fisher et al., 2005). Delta-9-tetrahydrocannabinol (THC) is increasingly used for the long-term treatment of nausea, vomiting, cachexia and chronic pain. Recent reports, however, have indicated an increased risk of myocardial infarction and thromboangiitis obliterans after THC intake. Blood platelets have an essential role in the pathogenesis of these two diseases, but it is unclear whether platelets are potential target cells for cannabinoids (Deusch et al., 2004). Bachs and Mørland (2001) reported six cases of possible acute cardiovascular death in young adults, where very recent cannabis ingestion was documented by the presence of THC in postmortem blood samples. A broad toxicological blood analysis could not reveal other drugs. Several reports, however, indicate an association of chronic THC intake and myocardial infarction. Aside from the observed activation of primary hemostasis, adverse side effects of THC on the cardiovascular system may contribute to the pathogenesis of thromboangiitis obliterans and myocardial infarction. Among them, a concentration-dependent increase in heart rate and arterial blood pressure, leading to an increased myocardial workload and oxygen demand, have been documented (Jones, 2002). Compromised oxygen supply by the increased generation of carboxyhemoglobin during marijuana smoking further deteriorates the myocardial oxygen balance. Clinical in vivo studies are warranted to determine the relevance of these potential cardiovascular and coagulation side effects of THC in seriously ill patients (Deusch et al., 2004).
The continuous increase in availability and popularity of cocaine has caused a dramatic rise in cardiac emergencies (Heesch et al., 2000; Meltser et al., 2004). Acute myocardial infarction may occur following cocaine use (20). Many case reports suggested that there is significant progression of coronary artery disease in cocaine users. Inhibition of the uptake of catecholamines by the cell and the resultant effects, including hypertension, has the potential of accelerating atherosclerosis. Arteries with or without coronary artery disease will have spasm and increased platelet aggregation. The associated increase in blood pressure and heart rate adds insult to the injury (Rezkalla and Kloner, 2007). Cocaine use has been associated with myocardial infarction, stroke and intestinal infarction (Heesch et al., 2000; Havranek et al., 1996; Satran et al., 2005). Abnormal endothelial function could contribute to focal vasospasm and thrombosis and predispose to premature atherosclerosis, all of which have been demonstrated in cocaine users with myocardial infarction (Heesch et al., 2000; Havranek et al., 1996; Keller and Lemberg, 2003). Cocaine blocks the presynaptic reuptake of epinephrine, norepinephrine, serotonin and dopamine, thereby enhancing sympathomimetic activity and affecting the cardiovascular system via multiple mechanisms (Satran et al., 2005). Cocaine exposure causes platelet activation, alpha granule release and platelet containing microaggregate formation. These data support the view that cocaine, even at the relatively low doses commonly self administered by occasional abusers, may promote thrombosis and predispose healthy individuals to ischemic events. Platelet inhibitors should be considered early in any patient with suspected cocaine related ischemia (Heesch et al., 2000).
Marijuana is the most widely used illicit drug in the United States. Marijuana use in the age group prone to coronary artery disease is higher than it was in the past. Smoking marijuana is known to have hemodynamic consequences, including a dose-dependent increase in heart rate, supine hypertension and postural hypotension (Mittleman et al., 2001; Mukamal et al., 2008). Smoking marijuana is a rare trigger of acute myocardial infarction and have a vasospastic effect (Mallaret et al., 2005; Lane et al., 2005). Understanding the mechanism through which marijuana causes infarction may provide insight into the triggering of myocardial infarction by this and other, more common stressors (Mittleman et al., 2001). Thus, some marijuana-associated infarctions may be caused by a myocardial oxygen supply that is inadequate to cope with the increased oxygen demands that occur as result of smoking Marijuana (Mittleman et al., 2001).
Myocardial infarction is a rarely reported complication of amphetamine use (Waksman et al., 2001). Marmor et al. (2004) showed that over the past 20 years, there was a paucity of morbidity and mortality due to cardiovascular disease among drug users in a methadone maintenance clinic. They investigated whether long-term exposure to opiates or opioids is associated with decreased severity of coronary artery disease (CAD) by comparing 98 decedents with methadone or opiates (M/O) in their blood at autopsy with 97 frequency-matched decedents without M/O. Severe CAD was found significantly less often in M/O-positive decedents (5 of 98) than in M/O-negative decedents (16 of 97). Long-term opiate exposure thus may mitigate CAD severity and its often fatal consequences (Marmor et al., 2004).
Disobey from physician’s medical, nutritional and activity recommendations after CABG is not at least, the sole cause of higher readmission rate due to cardiac complications in patients with current (active) opiate abuse. Carrying out the educational programs to correct the misconception about the beneficial effects of illicit drugs on cardio-vascular disease makes sense.